Psoriasis
Get the treatment you need at Riverchase Dermatology.
Psoriasis is a chronic or lifelong condition in which there is an abnormal and rapid cycling of the skin’s cells, resulting in a buildup of immature cells on the surface of the skin in the form of patches, plaques or pustules. It is not contagious but its unsightly appearance can be embarrassing for the sufferer. There are many different types of psoriasis of varying degrees of severity. This disease of the immune system can occur anywhere on the body. It is not something you can “catch” or that others can catch from you, and its lesions are not infectious.
Psoriasis FAQs
In addition to itchy and/or painful patches of skin, psoriasis is commonly a source of anxiety or depression. The disorder can cause embarrassment because of its noticeable scaling and redness. It can be painful, restrict daily activities and interfere with a good night’s rest.
People who get psoriasis usually have one or more person in their family who has psoriasis. Not everyone who has a family member with psoriasis will get psoriasis. In the United States, about 7.5 million people have psoriasis. Most people, about 80%, have plaque psoriasis.
Psoriasis can begin at any age, but most people get it between 15 and 30 years of age. By age 40, most people who will get psoriasis will have experienced it. Another common time for psoriasis to begin is between 50 and 60 years of age.
Caucasians get psoriasis more often than people of any other race, and infants and young children are more likely to get inverse psoriasis and guttate psoriasis.
Scientific studies have shown that about 10% of the general population inherits genes that cause psoriasis, while only 2 or 3% actually develop the disease. The cause of psoriasis is not known, but researchers say the immune system and genes play important roles. You must have a combination of these psoriasis-causing genes and be exposed to external triggers. To complicate matters, what causes psoriasis to develop is different from one person to another.
Established triggers include:
- Stress
- Bacterial infection, such as strep throat (staphylococcus)
- Medications, including lithium, antimalarials and some types of heart and arthritis medicines
- Skin injury, including bruises, chafing, shaving, tattoos, vaccinations or sunburn
- Skin conditions like scabies, blisters, boils and dermatitis
Less understood triggers that may play a role include:
- Allergies
- Medicines for high blood pressure (beta blockers)
- Dry weather, including winter days and indoor heating, or air conditioning
- Hormone surges that occur after puberty and during pregnancy
- Smoking and excessive drinking
Psoriasis Types
There are a variety of psoriasis types with distinct characteristics. Sometimes, one type of psoriasis will coexist with another type or clear and another will form in response to a trigger. Regardless of the type, each outbreak can vary in intensity from a mild case contained in one spot to a severe outbreak that involves large patches of skin on multiple areas of the body.
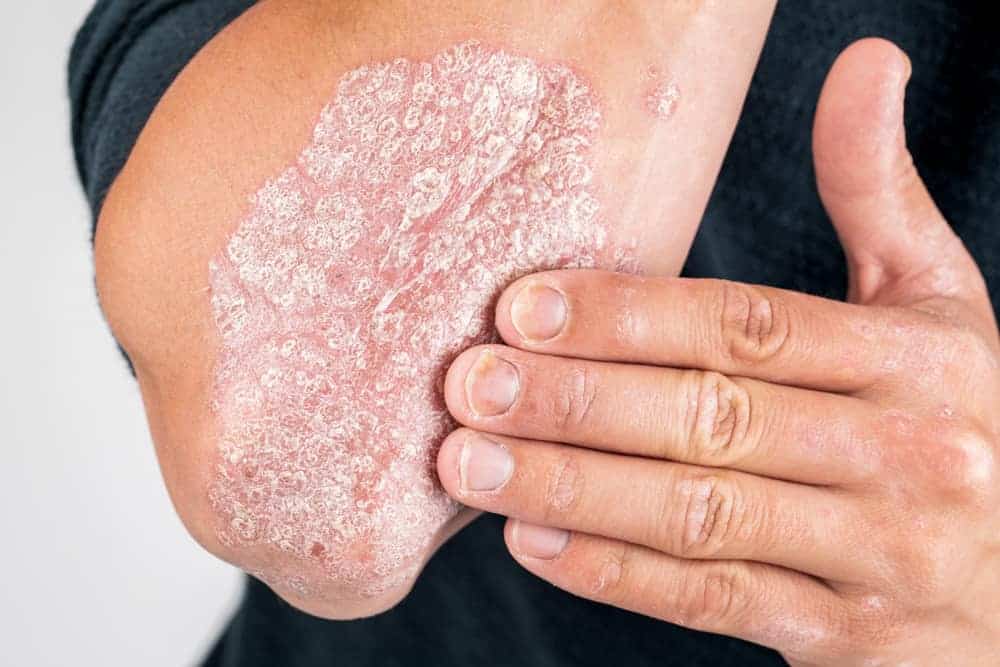
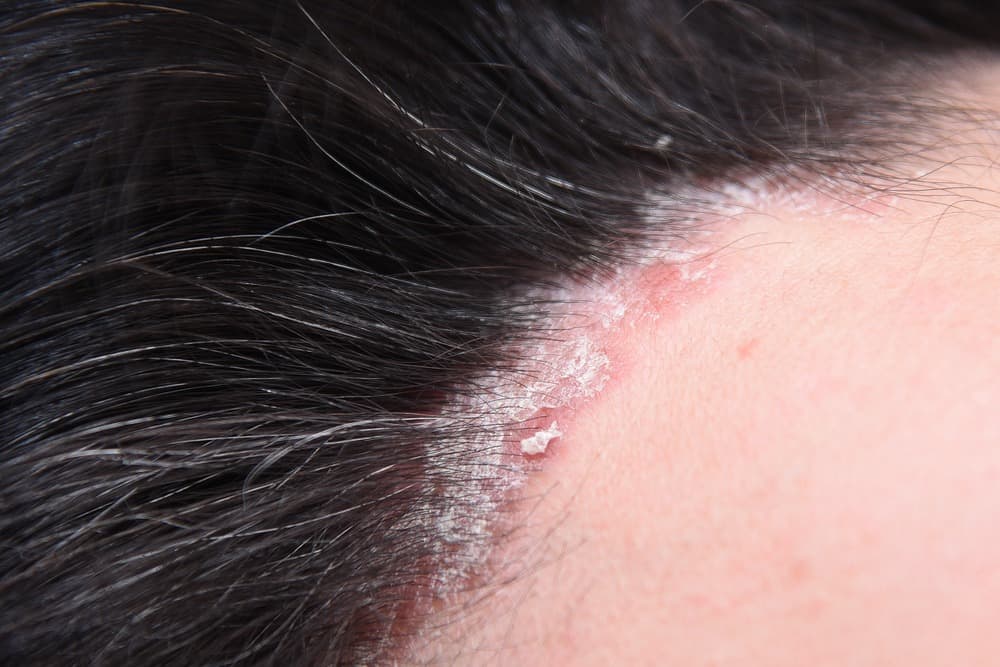
Plaque psoriasis
The most common type of psoriasis is plaque psoriasis, which is characterized by raised, red patches covered with silvery white scaling. This most often appears on the scalp, knees, elbows and lower back. Plaque psoriasis lesions can be itchy and painful, and the affected areas can crack and bleed. Plaque psoriasis affects about 80% of psoriasis sufferers.
Guttate psoriasis
The second-most common type of psoriasis appears as small red spots on the trunk, limbs and scalp and can precede or coexist with other types. Guttate is often triggered by bacterial infections like strep throat, tonsillitis and upper respiratory infections.
Inverse psoriasis
Inverse psoriasis, also known as intertriginous psoriasis, shows up as smooth and shiny, very red patches in body folds near the genitals, breasts or armpits. Many people have another type of psoriasis outbreak at the same time that they experience inverse psoriasis.
Pustular psoriasis
Pustular psoriasis is uncommon but consists of white pustules (pus-filled blisters) surrounded by red skin. The pus consists of white blood cells and is not contagious. Pustular psoriasis can be widespread or localized to the hands or feet.
Erythrodermic psoriasis
Erythrodermic psoriasis is a rare yet particularly inflammatory form that usually affects most of the skin on the body and sometimes happens at the same time as the pustular type. Fiery redness, itchiness and exfoliation of the skin occur, often accompanied by pain. Erythrodermic psoriasis can be life-threatening.
- Note: Call Riverchase Dermatology at 1-800-591-3376 or 911 immediately if you are experiencing an erythrodermic psoriasis flare-up.
Psoriatic arthritis
Psoriatic arthritis is not a type of psoriasis, but between 10-30% of psoriasis patients will develop this corollary condition, ranging from mild to severe symptoms. These include stiffness, pain and swelling in the joints, diminished mobility, and fatigue.
Treatment Options for Psoriasis
Riverchase Dermatology specializes in the treatment of psoriasis with care for the whole person, not just the disorder, in mind. Although there is no cure for psoriasis, your physician can provide a range of treatment options, both topical (on the skin) and systemic (throughout the body), that can clear psoriasis or lessen the severity of outbreaks for periods of time. Many advanced treatments for psoriasis are aimed at controlling the immune response, which is off balance in people with psoriasis.
You’ll likely need to try different treatments, such as topical and medications, phototherapy, and/or lasers (such as the Xtrac Excimer Laser) before finding the right treatment plan. Your doctor evaluates the type and severity of the psoriasis outbreak, its location on the body, ease and convenience of care, side effects and your treatment history before recommending care.
No blood test or tools can aid in the diagnosis of psoriasis. If you suspect that you or a loved one may have psoriasis, a Riverchase dermatologist can examine your skin and determine if psoriasis exists so you can begin treatment to lessen the impact that it can have on your health and lifestyle.
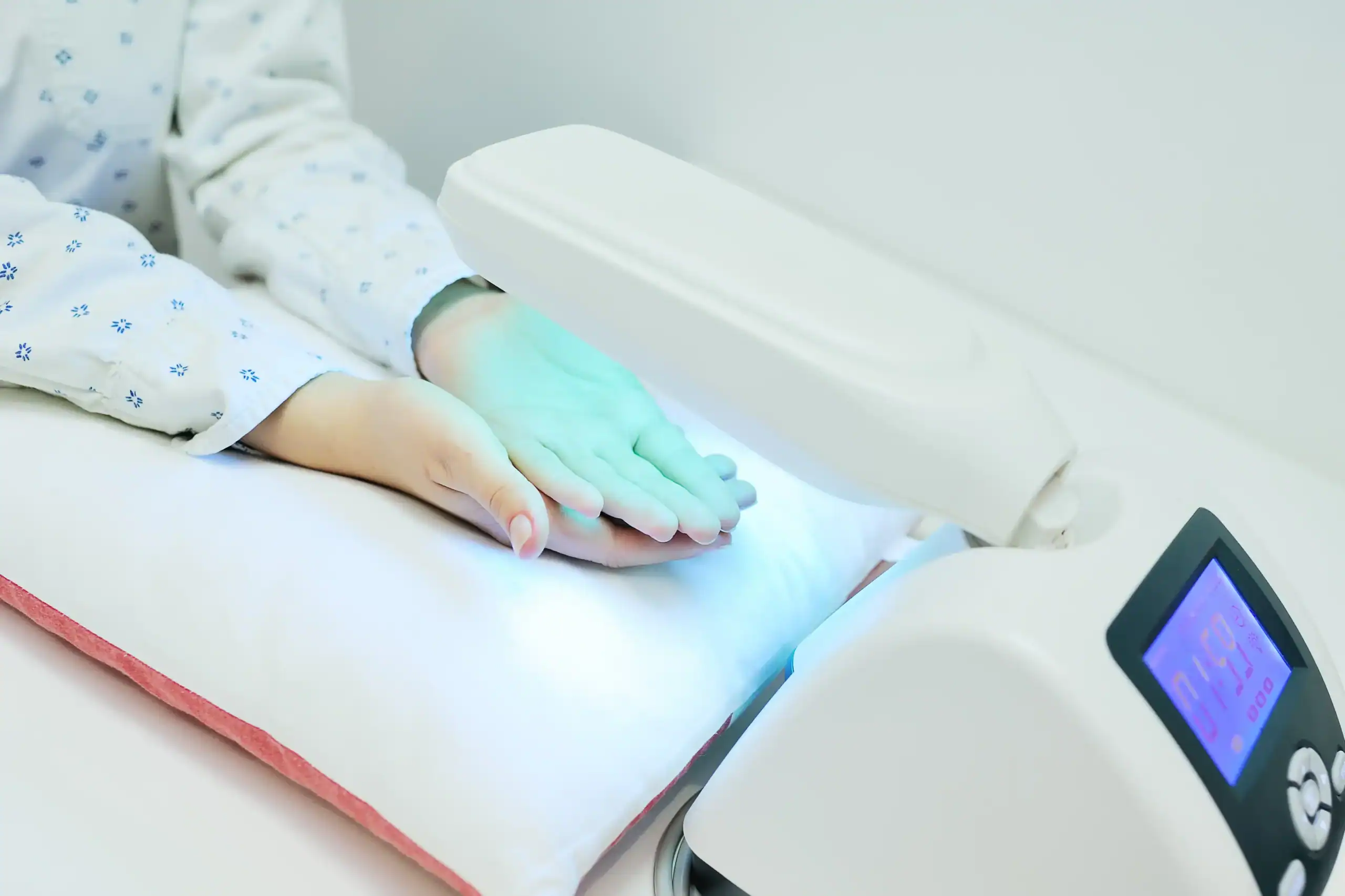
HOUVA III Phototherapy System
HOUVA III® Phototherapy System with DermaSense® Technology combines proven phototherapy treatment with the latest technology in UV light measurement. It is a high-output phototherapy system with integrated, removable sensors.
HAND/FOOT II
HAND/FOOT II is used in the treatment of hand and foot psoriasis. Extremely high outputs means we are able to treat the most difficult areas quickly and effectively using UVA, UVB, or Narrowband UVB.