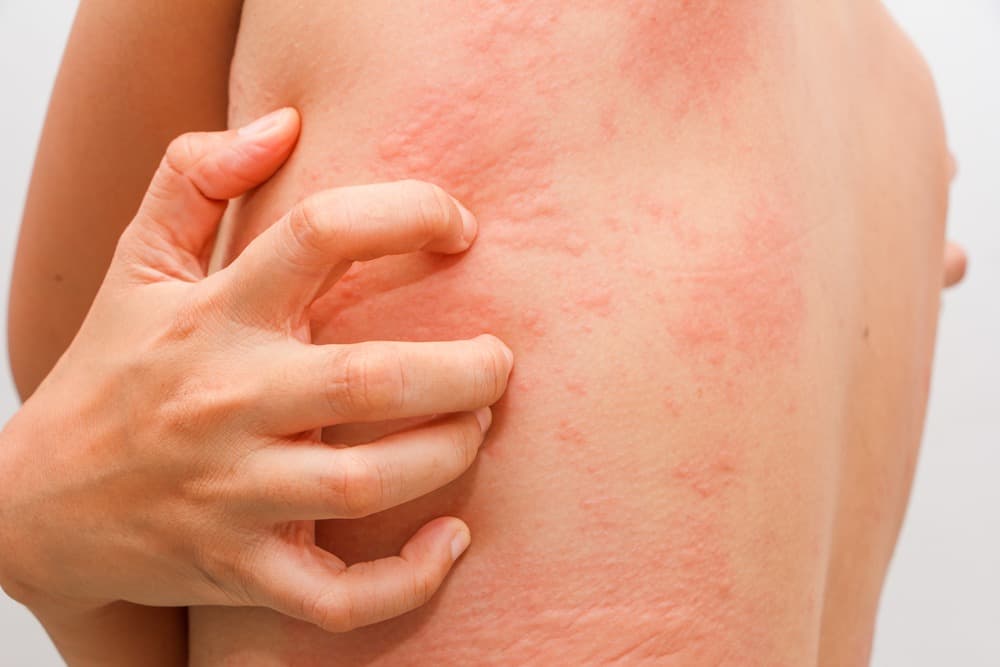
Eczema Flare-ups: 9 Ways to Minimize These Itchy Outbreaks
Just when you think your eczema has gone quiet, the dreaded itching starts again. It can drive you downright crazy. If you’re wondering how to get rid of eczema permanently, you probably can’t, unless it goes away on its own. But there’s plenty you can do to reduce eczema flare-ups, from avoiding your eczema triggers to managing stress.
Of course, following the eczema treatment plan your dermatologist developed for you is the best way to keep eczema under control long term, but the nine steps below can help those treatments work better and spare you some unnecessary itching.
1. Identify and avoid your triggers
Avoiding the irritants and allergens that bring on your eczema symptoms is essential to reducing flare-ups. If you’re having trouble identifying your triggers, try keeping a daily symptom diary. Write down your symptoms along with the foods you eat, the cleaning and beauty products you use, your stress levels, the weather and other potential triggers.
What causes eczema to flare up? Eczema triggers vary from person to person, but some common ones include:
- Dry skin
- Cleaning products such as laundry detergent and dish soap
- Personal products such as shampoo and body wash
- Perfume and products with added fragrance
- Stress
- Wearing rough fabrics such as wool and stiff synthetics
- Hot or cold weather
- Dry air
- Sweating
- Tobacco smoke
- Dust mites, pet dander, mold, pollen
2. Take shorter baths and showers
Spending too much time in the tub or shower can dry out your skin, especially if you use hot water. Limit baths and showers to 10 minutes or less and use lukewarm water. Gently pat yourself dry instead of rubbing your skin with the towel.
3. Keep your skin hydrated
Slather on a moisturizer at least twice a day, including right after your bath or shower. The less water—and therefore the more oil— it contains, the better. Ointments contain the least water. Creams have more water, and lotions typically have the most. Lotions are also more likely to sting skin that may already be sensitive from scratching.
Ointments, such as petroleum jelly and Aquaphor Healing Ointment, tend to be on the greasy side, so you might reserve them for nighttime use. If you prefer a less-greasy option, use a cream. Look for a thick one such as Cetaphil Moisturizing Cream or one designed for people with eczema, such as Cetaphil Eczema Restoraderm Cream or Eucerin Eczema Relief Body Cream.
If you have hand eczema, applying an ointment at night and covering your hands with cotton gloves can help.
4. Apply a barrier cream
Eczema weakens and damages the skin barrier, the uppermost layer of skin that defends against chemicals, irritants and harsh weather. A barrier cream contains ingredients that work together to strengthen and repair the skin barrier. They include ceramides, glycerin, dimethicone, squalene, hyaluronic acid and cholesterol, which is found in the skin barrier.
Good choices include Cetaphil Healing Ointment, Eczema Restoraderm Flare-Up Relief Cream and SkinCeuticals Triple Lipid Restore. Apply it once or twice a day, either after your daily moisturizer or at different times.
5. Use mild, unscented personal care products and detergents
Choose products that are free of fragrance and dyes and are formulated for sensitive skin. Using a bar soap instead of a liquid soap can be beneficial because bar soaps contain fewer ingredients and additives. Look for a product labeled non-soap cleanser, since true soaps can be harsh.
6. Wear sunscreen every day
Getting a sunburn inflames the skin and is likely to trigger an eczema flareup, so commit to wearing sunscreen every day. Choose a broad-spectrum sunscreen with an SPF of at least 30. Mineral sunscreen, which contains titanium dioxide and/or zinc oxide, is less likely to irritate the skin than chemical sunscreen.
7. Stop yourself from scratching
Eczema is known as the itch that rashes because scratching the itch leads to a rash. It can also make the itching worse. If your skin itches, apply calamine lotion or hydrocortisone cream or take a 15- to 20-minute lukewarm bath with colloidal oatmeal added to the water.
It’s a good idea to keep your fingernails short and filed to help minimize the damage if you do scratch. Need to stop the itch fast without scratching? The National Eczema Association recommends pinching the skin and then patting it.
8. Plan for weather changes
If dry air or cold weather triggers flares, run a humidifier in the room you spend the most time in and apply extra moisturizer. Bothered by hot and humid weather? Try to stay indoors when the heat is at its worst. Keep cool with a fan or air conditioner, and wear soft, breathable fabrics.
9. Minimize stress
Life is stressful, and so is living with eczema. The “stress hormone” cortisol increases inflammation in the body, which is the reason stress can lead to an eczema flare. People with eczema may benefit from meditation, mindfulness, music therapy or even a relaxing massage.
Keeping eczema flare-ups at bay may take some trial and error, but once you identify your eczema triggers and learn how to deal with eczema in a way that works for you and your skin, you can look forward to life with less itching.
Medically reviewed by Toluwalase Ogunsola, BSN, APRN
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How to Treat a Sea Lice Rash (Seabather's Eruption)
Is there any better way to spend the day than in the ocean? That depends on whether sea lice are present. If you’re unlucky enough to have a run-in with these tiny, transparent creatures during your dip, you may end up wishing you’d done something else. They leave swimmers with a red and bumpy sea lice rash, also known as seabather's eruption, that can be extremely itchy. In some cases, symptoms such as nausea, vomiting and fever develop as well, especially in children.
A sea lice rash is no one’s idea of summer fun, but since sea lice are nearly impossible to spot, you won’t know they’re there unless a sea lice warning has been posted at the beach. If you see warning signs or flags, spare yourself a rash by staying out of the water. Sea lice season in Florida and elsewhere runs spring through summer, with peak months in May and June, though the critters come and go.
If you do develop seabather’s eruption, there are steps you can take to limit the severity of the rash and ease the itching.
What is sea lice?
Despite their name, sea lice aren’t lice at all. Sea lice in Florida and other southeastern coastal states are the larvae of the thimble jellyfish, or Linuche unguiculata. You’re more likely to come across the other stinging larvae, that of the sea anemone Edwardsiella lineata, farther up the coast, from the mid-Atlantic states to New York.
The larvae feed on the blood of fish and aren’t interested in humans. But if they get trapped under your bathing suit, rash guard, T-shirt or wetsuit, the pressure causes the larvae’s stinging cells, called nematocysts, to sting you and release toxins that result in a rash. It’s similar to being stung by a full-grown jellyfish, though the stings, sometimes mistakenly called sea lice bites, aren’t nearly as painful.
In most cases, symptoms are mild to moderate. The reaction can be more severe in kids, especially those who have allergies or a weakened immune system, and in anyone who’s had seabather’s eruption before.
Sea lice rash symptoms
First you’ll feel a tingling sensation in areas where the larvae got trapped — under your clothing or even in the hair on your head and, for men, the chest hair. The tingling may start while you’re in the water or soon after you’re back on shore. Itching typically develops a few hours later. The rash, made up of small red bumps that may blister, typically appears four to 24 hours after swimming.
About 20% of people with seabather’s eruption develop additional symptoms such as fever, chills, fatigue and nausea.
Is sea lice contagious?
The sea lice rash isn’t contagious. That said, if you loan your bathing suit to someone else without washing or drying it, they could get a rash from the nematocysts that cling to it. You could get stung again yourself if you put the suit back on.
Be sure to wash your bathing suit, and whatever else you swam in, in hot water. If possible, dry it in a dryer. If you develop a severe sea lice rash, consider throwing out the item.
Sea lice treatment
You can’t avoid a rash if you’ve been stung by sea lice, but you can prevent a more severe reaction and treat the rash.
Limit the stings
If you start to feel that tingling sensation in the water or right after swimming, follow these do’s and don’ts to limit further stings for a less severe rash.
Do:
- Remove your bathing suit or other swimming clothing immediately and before taking any other steps.
- If you have it on hand, apply diluted vinegar or rubbing alcohol to the stung areas to neutralize toxins on the skin.
- Rinse your body in fresh water, such as a beach shower.
- Shower and scrub your skin with soap when you get home.
Don’t:
- Rinse yourself, jump in a pool or rub yourself with a towel while still wearing your bathing outfit (all of these can make the trapped sea lice sting you again)
Sea lice bite home remedies
If you develop a mild or moderate sea lice rash, you can treat the symptoms at home. Talk to your child’s doctor before giving the child a pain reliever or antihistamine.
- Wrap ice packs in a towel or cloth and place them on the stung areas.
- Take a non-steroidal anti-inflammatory drug such as ibuprofen to help relieve pain and inflammation.
- Apply calamine lotion or an over-the-counter topical corticosteroid cream (1%) according to the package directions to ease the itching.
- Take an antihistamine to calm the allergic reaction.
When to see a dermatologist
If the rash is severe, see your dermatologist for treatment. He or she may prescribe a topical corticosteroid that’s stronger than over-the-counter versions or an oral corticosteroid. Also contact a doctor if the rash develops signs of infection, such as pus drainage or increased pain, swelling or warmth.
A sea lice rash typically goes away in 10 to 14 days, though in some cases it may last as long as one or two months. The duration depends on the severity of the rash and how sensitive you are to the toxins released by the larvae.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Medically reviewed by Ashley E. Falzone, MD
How to Get Rid of Hives: At-Home and Prescription Treatments
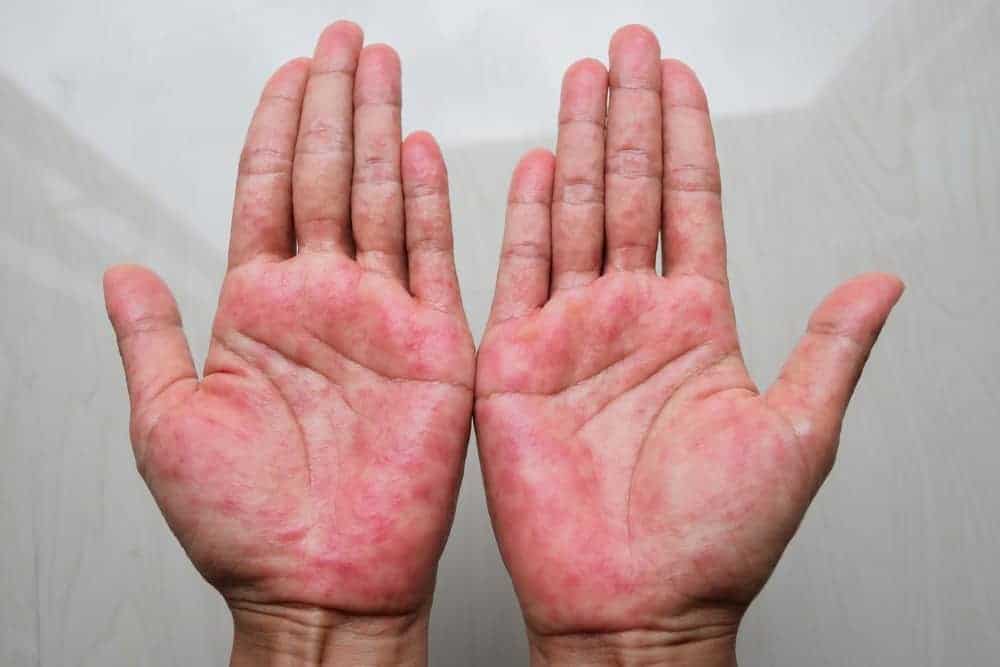
Red welts suddenly cropping up on your skin can be alarming, but chances are they are hives, which in most cases are more itchy than dangerous. How to get rid of hives? One mild or moderate episode can usually be treated at home. If you have chronic hives, your dermatologist can develop a hives treatment plan for you.
What do hives look like?
Hives, also called urticaria, are raised bumps or swollen-looking welts on the skin. “They can be as small as a pencil point or larger than your hand,” said Tara Duquette, PA-C, a certified physician assistant with Riverchase Dermatology.
The hives rash is usually pink or red in people with lighter skin, and skin-colored in people with darker complexions. Pressing on the bumps makes them turn light.
Hives can show up anywhere on the body, but they often appear on the torso, buttocks, upper arms and upper legs. They are typically very itchy, though you may feel a burning or tingling sensation instead. Sometimes they form large patches called plaques.
Along with hives, some people develop swelling deep in the lips, tongue or eyelids, a condition known as angioedema.
What causes hives?
Hives develop when your immune system releases a chemical called histamine in response to an allergen or something else you’re sensitive to. Histamine causes a chain reaction that results in inflammation and itching.
Allergens that can trigger hives include:
- Food
- Medication
- Pet dander
- Pollen
- Latex
- Bug bites
Other hives causes include:
- Hot or cold weather
- Sunlight (even without heat)
- Emotional stress
- Sweating
- Pressure on your skin from tight clothes or a purse strap
- Scratching your skin (dermatographic urticaria)
- Infections such as strep throat and COVID-19
- Radiation therapy
- Blood transfusions
Sometimes no cause can be identified. In many people with chronic hives, a trigger is never found.
How long do hives last?
Hives usually disappear in anywhere from a few minutes to a few days. Chronic hives, also called chronic spontaneous urticaria, can last much longer.
“Chronic hives come and go and can last for six weeks or more,” said Duquette. “They can be very itchy and can make it hard to sleep.”
When to see a doctor for hives
Make an appointment with your dermatologist if your hives last longer than a few days or they affect a large part of your body.
Call 911 or go to the emergency room immediately if you have swelling in your mouth or throat, you have trouble breathing or swallowing, you feel faint or you have a racing heartbeat.
How to get rid of hives: At-home and professional hives treatment
Hives treatment aims to reduce the inflammation caused by the release of histamines.
“In many cases, all you need is an oral antihistamine and cold compresses to soothe the itching,” said Duquette. If your hives are more severe, you may need something stronger.
If you have chronic hives, your dermatologist may refer you to an allergist to be tested for allergies, or to another doctor to be tested for underlying diseases, including autoimmune diseases. Some autoimmune diseases, such as lupus, can make you more susceptible to hives.
At-home care
To soothe your hives at home, apply cool compresses and take a non-drowsy over-the-counter antihistamine, following the instructions on the package. If you have it handy, apply Prax lotion (sold in drugstores), calamine lotion or an anti-itch lotion or cream that contains menthol.
While you’re waiting for the welt to disappear, wear soft, loose clothing, and avoid hot baths or showers and harsh or scented soaps.
Prescription treatment for hives
For a more severe hives outbreak, your dermatologist might prescribe a stronger antihistamine, such as desloratadine (Clarinex), and/or a corticosteroid cream. In some cases, an oral corticosteroid such as prednisone is needed to control the itching and inflammation.
Other hives treatments include doxepin (Silenor, Zonalon), which is an antidepressant that blocks histamine, and montelukast (Singulair), which is most often used to prevent and treat asthma attacks.
Chronic hives treatment
Chronic hives is often treated with antihistamines. If they don’t help enough, your dermatologist may suggest adding UV light therapy, also called phototherapy. An injectable medication called omalizumab is another option. It works by blocking the action of an immune substance called immunoglobulin E, which plays a role in hives.
If all else fails, immunosuppressant drugs may be prescribed to prevent the immune system from overreacting to hives triggers. These drugs can have serious side effects, so they usually aren’t prescribed unless you haven’t responded to other treatments. Examples of immunosuppressants used to treat hives include cyclosporine, methotrexate and hydroxychloroquine (Plaquenil).
For severe reactions: Epinephrine (EpiPen)
If you’ve had severe hives attacks or angioedema, or if the attacks continue despite treatment, your dermatologist may prescribe an EpiPen for you to carry. Self-injecting epinephrine works quickly to open a swollen airway if you develop swelling in the mouth or throat that prevents you from breathing.
Medically reviewed by Tara Duquette, PA-C
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
6 Types of Eczema: Which Do You Have?
Dry, itchy skin and rashes are signs of eczema, a common inflammatory skin condition. It’s often called atopic dermatitis — but that’s just one kind. There are several types of eczema, including the six below. Identifying the one you have can be challenging, since many of the symptoms are the same, but knowing exactly what causes your itch can help you tame it.
Your dermatology provider can give you an accurate diagnosis based on your eczema symptoms and other clues and get you the eczema treatment you need.
1. Atopic dermatitis
The most common form of eczema, atopic dermatitis usually develops during childhood, though it sometimes appears for the first time after age 18. Genetics are partly to blame. Having relatives with eczema, hay fever, asthma or food allergies increases your risk. Your environment also plays a role: If you are genetically prone to this type of eczema, you may be more likely to develop it if you live in a city or a cold, damp area.
Like many types of eczema, atopic dermatitis often comes and goes. You may have periods of flares and periods of remission, which can last for years.
What it looks like: Dry, cracked and swollen skin with rashes that are red in light skin and brown, purple or gray in darker skin. You may see tiny, fluid-filled blisters that ooze and crust.
How it feels: Itchy.
Where it appears: Anywhere on the body. Atopic dermatitis is common on the hands, elbows and knees. In infants, it’s common on the face.
2. Contact dermatitis
Contact dermatitis, also called irritant or allergic contact dermatitis, develops hours or days after you touch something that irritates your skin or causes an allergic reaction. A dermatologist can help you figure out your triggers. Common ones include fragrances, hair dyes, hair straighteners, nickel (found in jewelry and belts, for example), latex and plants such as poison ivy.
What it looks like: A rash that’s hot and swollen. Skin is dry and can crack. You may have fluid-filled blisters that ooze and crust. Round welts (hives) may appear.
How it feels: Itchy, stinging, tender, burning.
Where it appears: Anywhere, but most often the hands, as well as areas where you apply personal care products, such as your face, scalp and underarms.
3. Hand eczema
Hand eczema affects the hands only. It can be an occupational hazard for people such as hairdressers and metal workers. Hand eczema also affects people who wash their hands a lot, such as healthcare workers. You may be at increased risk of hand eczema if you have persistent or severe atopic dermatitis (or had it as a child) or are exposed to cold, dry weather and dry indoor air.
What it looks like: Dry, chapped and scaly hands with patches of red or dark brown skin, depending on your skin tone. You may develop blisters, crusting and deep cracks that could bleed.
How it feels: Itching, burning.
Where it appears: The top of the hands, the spaces between the fingers, and the palms. The wrist may also be affected.
4. Dyshidrotic eczema
Dyshidrotic eczema causes small blisters on the hands or feet. The condition isn’t well understood and can be hard to treat. It’s thought to be caused by a hypersensitivity to a substance such as metal (especially nickel), certain medications (such as aspirin and birth control pills), tobacco or ingredients in personal care products such as shampoo. If you have the condition, you may experience flares due to stress, changes in weather and sun exposure.
What it looks like: Small blisters that may be wet with sweat. As the blisters heal, the skin becomes dry and peels.
How it feels: Itching, burning, pain, prickly feeling.
Where it appears: The hands and feet, specifically the palms, fingers, toes and bottoms and sides of the feet.
5. Nummular eczema
This type of eczema, also called discoid eczema, has many possible triggers, including severe stress, a skin injury or infection, heavy alcohol use, dry air and heat and humidity. You may be more likely to develop nummular eczema if you have atopic dermatitis, contact dermatitis, very dry skin or poor blood flow in your legs. Some medications, particularly those that can dry the skin, can contribute to flares. They include isotretinoin (Accutane), statins and diuretics.
What it looks like: Tiny bumps or blisters that may join together to form raised, coin-shaped spots. In people with light skin, the spots are pink or red. In people with dark skin, the spots may be brown or lighter than your skin tone. They may ooze fluid. The skin between the spots is typically very dry.
How it feels: Very itchy, stinging.
Where it appears: The forearms, legs and backs of the hands.
6. Stasis dermatitis
Stasis dermatitis, also called venous eczema, can occur in anyone who has poor circulation in the legs caused by venous insufficiency. It usually affects the lower legs. You’re more likely to develop it if you have varicose veins, obesity, high blood pressure, heart disease or kidney disease or if you have been pregnant several times. Even standing or sitting for prolonged periods can lead to stasis dermatitis in people who are vulnerable.
What it looks like: Dry skin that may be scaly and discolored. Wounds may develop.
How it feels: Itchy, sore to the touch.
Where it appears: The lower legs, especially the skin on top of varicose veins.
Eczema treatments
Some types of eczema can be challenging to treat, but dermatologists have many ways to get even stubborn cases under control.
Your dermatologist can develop a custom treatment plan based on your type of eczema and its severity. The plan may include topical corticosteroids or non-steroid creams. Other eczema treatments are light therapy (phototherapy) and, for persistent cases that are moderate to severe, oral medicines or injectable biologic medicines that calm the immune system. If your eczema seems to be triggered by an allergy, your dermatology provider may recommend an antihistamine or suggest allergy testing.
Avoiding your eczema triggers, taking shorter, cooler showers and using a thick moisturizing cream or ointment to help keep the skin’s outer layer intact are other smart strategies for reducing flares.
Medically reviewed by Michael Cohen, DO
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
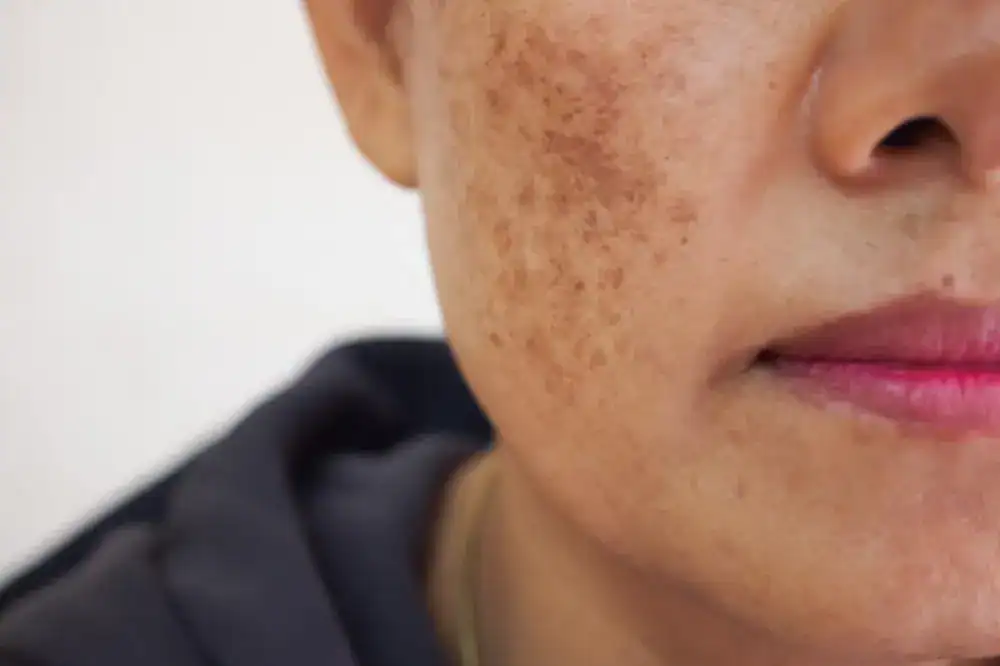
Melasma Treatment: How to Fade Brown Patches on the Skin
Melasma causes brown patches on the skin that many people find unsightly or embarrassing. It’s sometimes called “the mask of pregnancy,” but the condition isn’t limited to pregnant women. What triggers these dark splotches? And if you have them, what’s the best melasma treatment?
Read on to discover answers. There is no surefire melasma cure, and the condition can be difficult to treat without making it worse — a good reason to see a dermatologist or other qualified skin care provider rather than randomly picking an over-the-counter melasma cream. An experienced provider will help you zero in on treatments that offer the best possible chance at giving you back a more even complexion.
What is melasma?
Melasma is a type of hyperpigmentation, a condition in which cells that produce the skin pigment melanin make too much of it. In melasma, this results in dark patches. The patches are usually brown, but they may be blue-gray or gray-brown in people with darker skin. They usually appear on the face — the cheeks, the bridge of the nose, the upper lip or the chin. Patches on the upper lip are sometimes called a melasma mustache or a sunstache.
Occasionally, melasma appears on other parts of the body that get a lot of sun exposure, including the forearms, shoulders and neck.
Anyone can develop melasma, but 90% of cases happen in women. The condition is more likely if your skin tone is medium or dark. It typically appears in a person’s 20s, 30s or 40s.
For the best results, seek treatment ASAP. It’s harder to fade melasma patches if you’ve had them for years.
Melasma vs. sun spots
Brown patches on the face are sometimes mistaken for age spots, also known as sun spots or liver spots, but these two hyperpigmentation conditions are different.
Age spots are caused by years of sun damage. They are isolated small or large spots and are closer to the surface of the skin than melasma patches, which makes them easier to treat. They can appear on any body part that gets sun exposure, such as the hands.
Melasma, on the other hand, causes dark patches that most often appear on the face, usually on both sides. Sun exposure is just one of several possible triggers. Unlike age spots, melasma patches sometimes disappear on their own.
Melasma causes
Melasma causes aren’t well understood. The condition likely results from some combination of genes (up to half of people with melasma have or had a close relative with melasma), hormonal changes and sun exposure. In some cases, a medication is to blame.
Here are some common melasma triggers.
Pregnancy, birth control and HRT
As many as half of pregnant women develop melasma. The surges of estrogen and progesterone that occur during pregnancy are thought to send the cells that produce melanin, called melanocytes, into overdrive.
Starting or stopping hormonal forms of birth control or undergoing hormone replacement therapy can also trigger melasma.
Cortisol, the 'stress hormone'
Experts are divided on whether stress triggers melasma. Some studies suggest a connection. If there is one, fluctuating levels of cortisol could be to blame, since cortisol plays a major role in the body’s response to stress.
Sunlight
Exposure to ultraviolet (UV) light causes melanocytes to produce more melanin. It’s possible that melasma could result from uneven melanin production after sun exposure or tanning bed use.
Thyroid disease
Melasma is more common in people with hypothyroidism, a condition in which the thyroid gland doesn’t make enough thyroid hormone. More research is needed to determine whether there’s a direct relationship.
Medication
Some medications have been associated with melasma. They include certain:
- Anti-seizure medications
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Drugs that make you more sensitive to the sun, some blood pressure pills and some antibiotics
Sun exposure can intensify melasma that’s triggered by medications. Switching medications or reducing the dosage, if your doctor okays it, may improve it.
Skin irritants
Skin irritants can cause melasma or make it worse by causing inflammation that leads to increased pigment production. Potential irritants include makeup, harsh or scented soaps and even some skin treatments.
Melasma treatment
Melasma is difficult to treat. The patches sometimes go away, or at least fade, on their own. That’s more likely to happen if they developed during pregnancy or after starting birth control pills. For many people, however, the condition is chronic. Even if you treat it successfully, the patches may come back.
For the best results, seek treatment ASAP. It’s harder to fade melasma patches if you’ve had them for years. Before suggesting treatment options, your dermatologist will confirm that the brown patches on your face are in fact melasma and not another skin condition.
There is no one melasma treatment that works for everyone. Your dermatologist will likely recommend a combination of treatments as part of a custom management plan that’s based on your skin type, your melasma triggers and the depth of your skin patches. Avoiding sun exposure is critical.
Hydroquinone
Hydroquinone, a topical skin-lightening medication, is one of the most common treatments for melasma. Over-the-counter 2% hydroquinone products are available, as are stronger prescription versions. However, hydroquinone can’t be used long term because it may eventually cause a bluish discoloration of the skin called ochronosis.
Hydroquinone is often prescribed together with tretinoin (Retin-A) and a mild corticosteroid. The combination works better than hydroquinone alone. It’s available as a melasma cream that’s sometimes referred to as triple treatment cream.
Tretinoin plus a steroid
If you have dark skin, your doctor might prescribe topical tretinoin and a topical steroid, leaving out the hydroquinone.
Tranexamic acid
Extremely stubborn melasma may respond to skin-brightening tranexamic acid, which is available in topical and oral forms.
Vitamin C and other acids
Gentler topicals that may be used to fade melasma patches include vitamin C (ascorbic acid), azelaic acid and kojic acid.
In-office procedures
If other treatments deliver so-so results, your dermatologist may suggest adding one of several in-office treatments to remove excess pigment and/or increase skin cell turnover. Options include microneedling, a chemical peel or a laser treatment.
If you go the chemical peel or laser route, it’s important to see a board-certified dermatologist or a licensed aesthetician who has experience treating melasma. Peels that use strong acids can cause more brown patches, as can some laser therapies.
The one thing everyone with melasma should do is apply sunscreen liberally. Use a broad-spectrum sunscreen with an SPF of at least 30. Many dermatologists recommend choosing a mineral sunscreen rather than a chemical sunscreen. Try a tinted mineral sunscreen. The iron oxide helps to block blue light from cell phone and computer screens, which could contribute to skin discoloration.
Book a consultation today to get your melasma treatment started.
Medically reviewed by Jeriel Weitz, DO
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How to Get Rid of Athlete’s Foot
The burning and itching of athlete’s foot is bad enough. When you add ugly, cracked, scaly skin, the condition can go from irritating to embarrassing. If you have it, you’re probably wondering how to get rid of athlete’s foot permanently and in a hurry. Treating this foot fungus ASAP is key to banishing it, so read on to discover athlete’s foot treatments that work.
What is athlete's foot?
Athlete’s foot, also known as tinea pedis or ringworm of the foot, is a fungal skin infection of the foot. Athlete’s foot symptoms include an itching, burning rash, cracked, scaly skin and small blisters. The rash often occurs between the toes, but it can affect the bottom and sides of the feet in a type called moccasin athlete’s foot.
Athlete’s foot probably won’t go away on its own, so don’t ignore it. If you leave it to fester, you could end up with large, painful cracks (fissures) that let bacteria in. What’s more, the fungus could spread to other body parts, including your groin, hands, nails and underarms. You could even spread it to someone else.
What causes athlete’s foot?
Athlete’s foot is caused by a fungus that thrives in warm, humid environments such as locker room floors, gym showers and the sweaty insides of tight-fitting shoes.
Despite the name, you don’t have to be an athlete to develop it. In fact, athlete’s foot is most common in people over 60. Why? A few reasons. If you have trouble reaching your feet, it’s harder to keep them clean and dry and to change your socks as often as you should. Swollen feet, more common in older age, can make shoes too tight. Dry, cracked skin on the feet, common in people with diabetes, also makes the feet more susceptible to fungal invasions.
Athlete’s foot treatment
When it comes to how to get rid of athlete's foot, the answer is either over-the-counter products or prescription medicines. Over-the-counter products often cure mild to moderate cases, especially when the foot fungus is treated early on, though it may take some trial and error to find the product that works for you. The longer you wait to treat your athlete’s foot, the harder it is to cure, and the more likely the fungus will spread or reoccur.
If over-the-counter treatments aren’t working, you have a severe case or your athlete’s foot comes back, see your dermatology provider, who can prescribe stronger medicine.
Over-the-counter treatments
Over-the-counter treatments for athlete’s foot include creams, sprays and powders that kill or slow the growth of the fungus. Apply them to clean, dry feet, following the directions on the package.
- Athlete’s foot cream or ointment: These contain a medicine such as terbinafine. Spread the cream onto your foot in a thin layer and allow it to dry completely before putting on socks and shoes. If you’re in a rush, choose a spray or powder instead.
- Athlete’s foot spray: Spray may be a good option if you have a hard time reaching your feet or the infection covers a large area. Some sprays contain baking soda and are designed to reduce moisture and odor. Others are liquid.
- Athlete’s foot powder: Powders, such as ones that contain miconazole, may be a good option if you have sweaty feet or recurring infections.
While you’re treating your athlete’s foot, it’s important to practice good foot hygiene to encourage healing. Wash and dry your feet at least once a day. Change your socks daily and wash them in hot water. Switch shoes every day or two to give each pair a chance to dry out between wearings.
Prescription treatments
If an over-the-counter product hasn’t cured your athlete’s foot after two weeks of dedicated treatment, make an appointment to see your dermatologist, who can attack the problem with stronger medicine.
Prescription athlete’s foot treatments include creams and ointments such as ciclopirox, econazole and clotrimazole. Because they are powerful, be sure to apply them exactly as directed.
Your dermatology provider may prescribe an oral medication for athlete's foot if your case is severe or doesn’t respond to topical treatments. These antifungals need to be taken for several weeks or months, and they come with potential side effects, so you and your doctor should weigh the risks and benefits.
Preventing athlete’s foot
As with so many health conditions, prevention is the best medicine when it comes to athlete’s foot. These strategies will reduce your risk:
- Keep your feet clean and dry.
- Wear shoes, flip-flops or slippers in wet, humid or communal areas, including public gyms and pools and hotel rooms.
- Dry your feet thoroughly after the beach or pool before putting your shoes back on.
- Wear shoes that fit well.
- Favor sandals when possible to let your feet breathe.
- Choose socks made of moisture-wicking fabric such as a wool or polyester blend. The 100% cotton socks in your drawer are not the best choice for moving moisture away from your feet.
- Change your socks daily and after workouts.
- Don’t share shoes, socks or towels.
Medically reviewed by Toluwalase Ogunsola, APRN
Written by Johanna Neeson, a health and lifestyle writer in New York City. Her work focuses on dermatology, pediatrics, and autoimmune diseases and has appeared on Everyday Health, MSN, Reader’s Digest, and other publications.
Does Dairy Cause Acne? The Skinny on Milk and Breakouts
Milk and cereal go hand in hand. What about milk and acne? That’s a debate that’s raged for years. So what does the current science say about the diet and acne connection when it comes to dairy — does dairy cause acne?
The answer is: not exactly.
“Dairy, or any food for that matter, does not cause acne per se,” said Shanna Miranti, MPAS, PA-C, a certified physician assistant at Riverchase Dermatology. “However, if you’re already prone to acne, certain dairy products could make it worse.”
Read on to learn more about whether dairy has a place in an anti-acne diet.
How milk may aggravate acne
More research is needed, but several studies show a connection between milk and acne. Why milk could make your complexion spottier is — pun intended — not entirely clear, but sugar and hormones are two suspected culprits.
Acne, inflammation and milk
“Certain foods are pro-inflammatory, and milk may be one of them,” Miranti said. “Milk can worsen other inflammatory skin conditions, such as eczema and psoriasis, so it’s not surprising that it would have the same effect on patients with acne.”
Inflammation isn’t just an effect of acne after pimples develop. “We now know it’s present during the entire process of acne development,” said Miranti. In other words, more inflammation may equal more acne or more severe acne.
The sugar content of milk, while fairly low, could contribute to inflammation, especially if you consume a lot of milk. Sweet, high-carbohydrate foods and drinks cause spikes in blood sugar that raise inflammation. These same spikes may trigger increased production of pore-clogging sebum, and change the composition of that sebum.
Acne and hormones in milk
Then there are hormones. Artificial growth hormones are given to some cows to boost milk production. Organic milk is produced by cows that are not given added hormones, but all cows produce their own hormones.
“Hormones play a big role in stimulating acne in people of all ages,” Miranti said. “It’s possible that the hormones in cow’s milk could upset your natural hormone balance in a way that aggravates acne.”
For example, cows produce insulin-like growth factor-1 (IGF-1, which surges during puberty in humans and contributes to acne. They also produce sex hormones called androgens, which can also contribute to acne.
Skim milk vs. whole milk
Your choice of milk could affect whether it contributes to acne. Some of the few published studies on acne and milk suggest that skim milk and low-fat milk may be more likely to exacerbate acne than whole milk.
One reason may be that skim milk has a somewhat higher glycemic index than whole milk. The glycemic index indicates how fast a food increases your blood sugar.
Another possible explanation is that skim milk contains fewer skin-friendly fatty acids. These same fatty acids help your body absorb the vitamin A and vitamin D in milk, and both these nutrients are essential for healthy skin.
Does cheese cause acne?
Cheese has a bad rap when it comes to its effects on skin complexion. It’s true that cheese, especially hard cheese, contains a good deal of saturated fat, but cheese lovers can relax: According to the American Academy of Dermatology, there’s no evidence that cheese worsens acne. Yogurt’s story is even better: Eating yogurt is thought to decrease inflammation.
Does whey protein cause acne?
Whey is one of the two main proteins found in milk, along with casein. It constitutes the liquid portion of cheese and is the main ingredient in whey protein powders, popular with some athletes.
Whey has been shown to raise levels of the hormone insulin, which can make acne worse. Very small studies have suggested a link between whey protein supplements and acne, but not nearly enough research has been done to establish cause and effect.
The decision to cut milk
If you’re considering dropping milk from your diet to see if it improves your acne, follow these tips.
1. Talk to your dermatologist first
Talk to your skin care provider before cutting out milk, since it’s more likely that other factors are behind your breakouts.
Every acne patient is different, so avoiding milk may not have an effect on your acne,” Miranti said. “If it does help, it’s not going to clear your acne completely because there are other contributors, such as genetics, that altering your diet can’t solve.”
2. Consider how you’ll get calcium
Keep in mind that eliminating milk may have health consequences. Many people get most of their calcium from dairy products, and calcium is essential for bone health. Before you give up milk, talk to your doctor or a registered dietitian about how to make up for the lost calcium.
3. Try cutting back or switching to whole milk
Instead of giving up milk entirely, you could try changing your milk consumption habits. If you usually use skim milk, switching to whole milk might be enough to reduce breakouts if milk is in fact a trigger for you. Or you could cut back on the amount of milk you consume, since some studies suggest milk aggravates acne only if you drink a lot of it. Remember that even if you don’t drink milk by the glass, the milk you add to cereal, coffee and smoothies can add up.
4. Be patient
It could take several weeks or even months to see a difference in your skin when you make a change in your milk consumption. But don’t be surprised if your acne doesn’t budge as a result of a dietary tweak.
“Diet may be just one part of the puzzle,” Miranti said. “If you have persistent acne, see a dermatology provider, who can recommend treatments that have much more scientific evidence backing their effectiveness. Most acne patients will need an acne-friendly skin care regimen as well as prescription medications.”
Medically reviewed by Shanna Miranti, MPAS, PA-C
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Scabies Rash and Other Scabies Symptoms to Watch for
Of all the rashes you or your child could develop, the scabies rash may be one of the most unexpected, and one of the hardest to ignore. The pimple-like bumps could be mistaken for symptoms of any number of other rashes and dermatitis, but another hallmark scabies symptom, severe itching, sets scabies apart.
“The itching can be relentless. In some cases, it’s almost unbearable,” said Ashley Falzone, MD, a dermatologist with Riverchase Dermatology. “It’s typically more intense at night and may prevent you from sleeping.”
Not everyone with scabies experiences this level of itching, but most do.
A scabies diagnosis often comes as a shock, since many people assume scabies affects only people in developing nations and those living in unsanitary conditions. But in fact, anyone can get it.
What is scabies?
Scabies is a parasitic infestation that develops when microscopic scabies mites (Sarcoptes scabiei var hominis) burrow into the outer layer of skin to lay eggs. Mite proteins and droppings in the burrowed tunnels trigger an allergic reaction that causes itching. Scratching may lead to sores, which could become infected.
Scabies mites exist around the world, but scabies infestations are more common in tropical countries and in crowded places where close physical contact is common. Young people, old people and those who have a compromised immune system are the most susceptible.
If you suspect scabies, see a dermatologist right away. Prompt scabies treatment will help avoid the spread of this contagious skin condition.
How to identify scabies
Severe itching is usually the first scabies symptom. The scabies rash may look like pimples or hives or bites, which may or may not form a line. In people with lighter skin tones, the bumps are pink or red. In people with dark skin, they may be skin colored, lighter than the skin or darker than the skin.
You’ll likely see the bumps on certain areas of the body, such as:
- Between the fingers and around the nails
- The inner wrist and elbow
- The armpit
- The waistline
- The lower buttocks
- The shoulder blades
- The penis
- The areola (the area around the nipple)
The scabies rash may be limited to one of these places, or you may see it on most of the body. In adults, the only places the mites doesn’t usually burrow are the head, face, neck, palms and soles of the feet. Babies and small children who develop scabies, on the other hand, often get it on their palms, the soles of their feet, their head and their neck.
In some cases, you may be able to detect the burrows the mites made when they tunneled into the skin.
“If you notice tiny, short, crooked, raised lines that are grayish-white or skin colored, you’re probably looking at burrows,” said Dr. Falzone.
To see pictures of scabies, scroll to the bottom of this article.
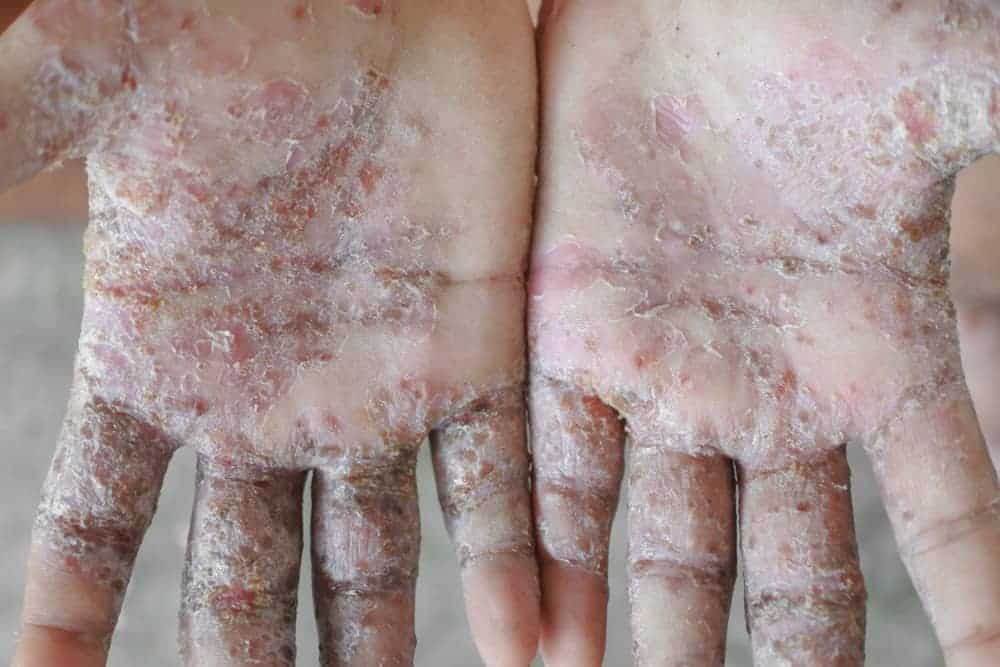
Crusted scabies (Norwegian scabies)
Crusted scabies, also called Norwegian scabies, is a severe form of scabies. People with classic scabies are typically infested with 10 to 15 mites, but people with crusted scabies may have up to 2 million mites in their skin.
What does crusted scabies look like? Bumps may or may not form (and if they do, they may or may not itch). The main symptom of crusted scabies is thick, crusty patches of skin, which may be yellowish or grayish. These patches are filled with mites and eggs.
The risk of developing crusted scabies is higher in people who use corticosteroids or immunosuppressants for a long period of time, and people who have certain other risk factors. Those risk factors include:
- A weakened immune system
- Advanced age
- HIV/AIDS
- Systemic lupus erythematosus
- Dementia
- Down syndrome
- Leprosy
Crusted scabies is extremely contagious and requires immediate treatment.
How does scabies spread?
Lengthy skin-to-skin contact spreads scabies, as does sharing items such as bedding, clothing and towels. In adults, scabies is often spread through sex.
“You typically won’t get classic scabies from a handshake or quick hug,” said Dr. Falzone.
Crusted scabies can be spread through briefer physical contact. It can also be spread when the skin crusts fall off. The mites and eggs they contain can survive and infect others for up to a week.
Infestations in the United States most often occur in nursing homes, long-term care facilities, schools and prisons.
Scabies treatment
If you, your child or another loved one is diagnosed with scabies, your dermatologist will prescribe a cream or lotion that contains a scabicide, a medication that kills the mites.
“It’s important that close contacts are treated at the same time, even if they don’t have scabies symptoms, to prevent spreading and re-infection,” said Dr. Falzone.
Permethrin cream is the go-to scabies treatment. Sulfur ointment may be even more effective, but many people are put off by its strong, unpleasant odor. Crotamiton lotion or cream is sometimes prescribed, but it’s less effective than permethrin and often requires two applications.
If the first treatment doesn’t work, the dermatologist might prescribe Lindane lotion, which is highly effective but may cause side effects, or an oral medication called ivermectin. Lindane lotion is not for use in small children.
Crusted scabies is often treated with a topical medication such as permethrin, plus ivermectin. The dermatologist may also recommend a keratolytic cream — a cream that breaks down the outer layer of skin — to reduce crusting. De-crusting the skin helps the topical medicine reach the mites.
Thoroughly cleaning and vacuuming the person’s surroundings is also a must. You’ll also need to do laundry. Throw bedding, towels and clothes used during the three days before treatment into the washer. Wash them on hot, then dry them on the hottest setting. Items that can’t be machine washed should be sealed in plastic bags for four to seven days.
Medically reviewed by Ashley Falzone, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
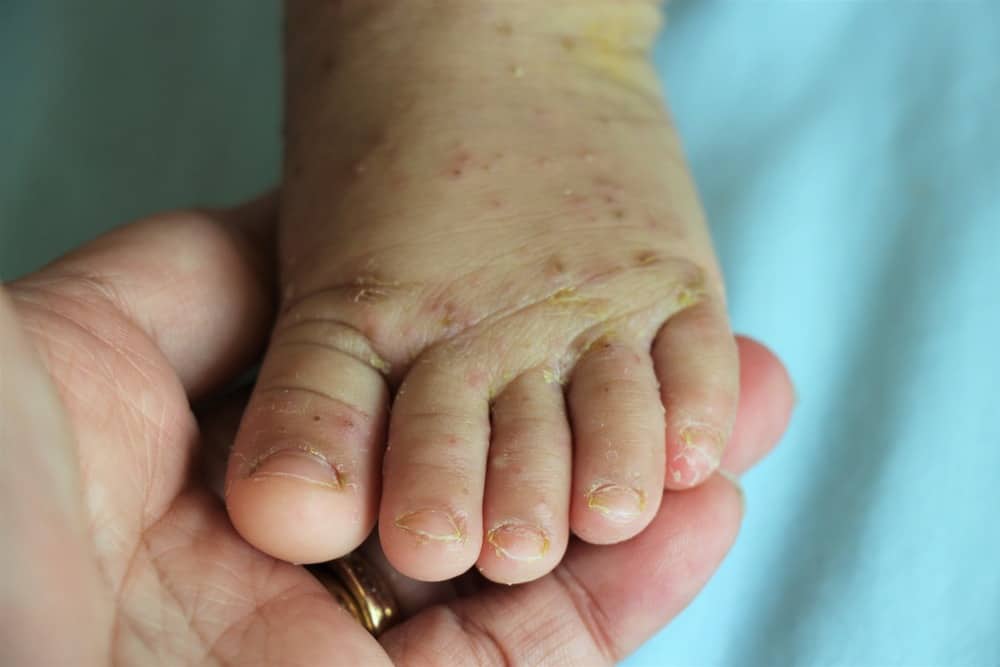
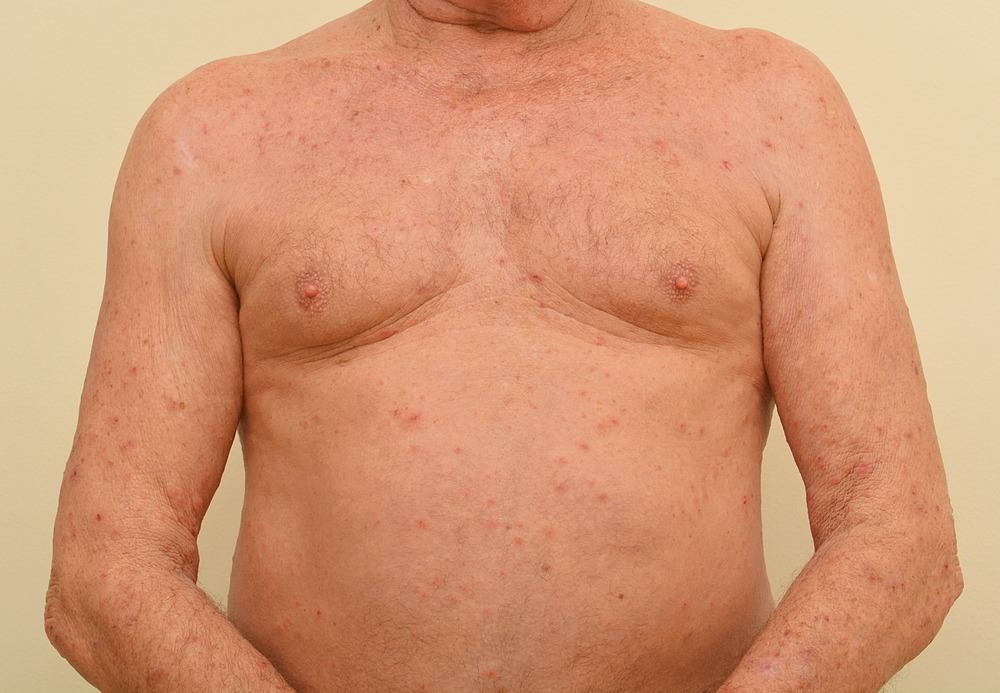
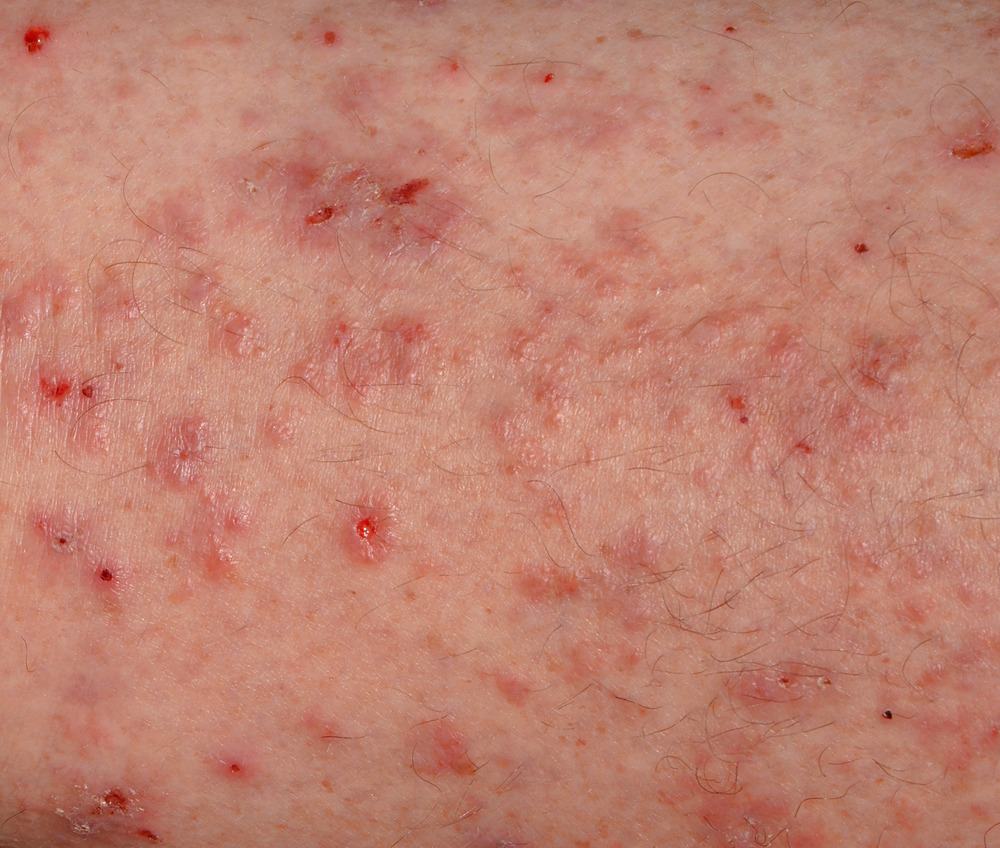
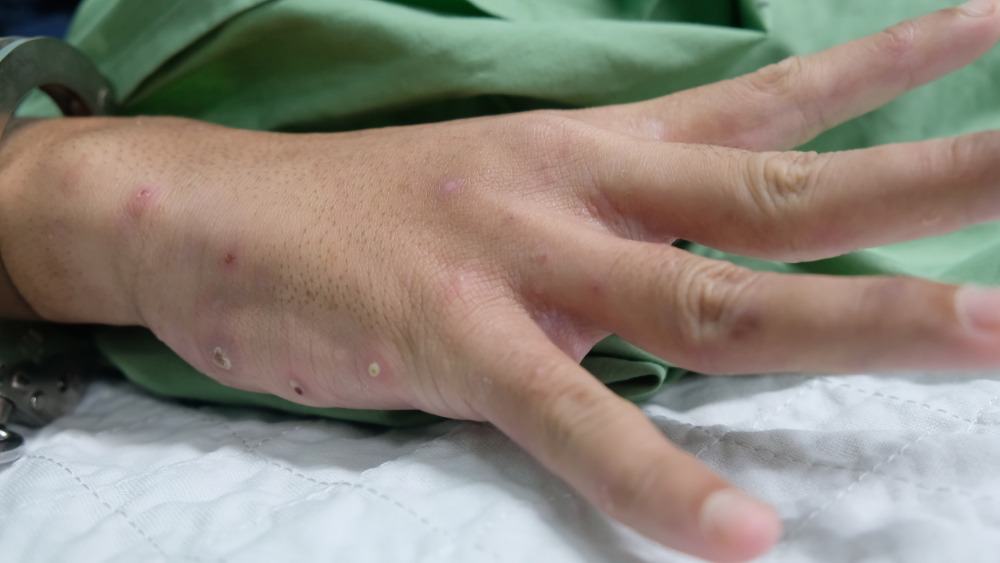
Scabies pictures
Scabies can look different in different people and at different stages. These pictures of scabies are examples. Your dermatologist can determine whether you or a loved one has scabies.
Fordyce Spots: Why They Develop and How to Get Rid of Them
At some point in your life, you’ve probably had little white bumps on your face, either pus-filled whiteheads or milia (firmer bumps caused by trapped keratin). But small bumps on the border of the lips or inside the lips or cheeks may be more of a mystery. In all likelihood, these bumps are Fordyce spots. They can also appear on the genitals, causing anxiety or outright alarm.
“People often worry when they find Fordyce spots on their genitals because they think they might have a sexually transmitted infection,” said Lucy Chen, MD, a board-certified dermatologist at Riverchase Dermatology. “But unlike STIs, Fordyce spots aren’t harmful or contagious.”
In most cases, Fordyce spots treatment isn’t necessary. But because the spots can resemble STIs as well as other harmful skin conditions, such as basal cell carcinoma, it’s a good idea to have your dermatologist make a diagnosis.
“In most cases, it’s possible to distinguish Fordyce spots from other skin conditions through a visual examination,” said Dr. Chen.
What are Fordyce spots?
Fordyce spots, also called Fordyce granules or Fordyce glands, are enlarged oil glands. They got their name from the dermatologist who first described them. They are very common, especially in men and people with oily skin. The cause is unclear, but it’s thought that the spots are present at birth and become noticeable during puberty or adulthood, possibly due to increased oil production and natural changes in hormone levels.
The spots are small, ranging from 1 millimeter to 3 millimeters in diameter (between the size of a pinhead and a sesame seed), and slightly elevated. Some people have just one spot, but it’s more common to have multiple spots, which may be scattered or clustered together. They’re usually a whitish-yellow color, but spots on the genitals can be reddish. The spots are more obvious when you stretch the affected area of skin. They are not contagious.
Though Fordyce spots are usually just a cosmetic issue, there are exceptions. “They can sometimes itch, which may be embarrassing if the spots are located on the genitals,” said Dr. Chen.
Fordyce spots on the lips
Fordyce spots on the lips typically occur on the edges of the lips, where the lip meets the surrounding skin, an area known as the vermillion border. They’re distributed symmetrically, cropping up on both sides of the lips. They can also appear on the inside of the lips.
Fordyce spots on the genitals
Fordyce spots can occur on the genitals in men and women. Because they can resemble herpes sores or early-stage genital warts, see a doctor to get an accurate diagnosis if you discover spots or bumps on your genitals.
Certain clues can distinguish these spots from sexually transmitted infections. For instance, herpes causes painful blisters, and Fordyce spots don’t blister. As for genital warts, they can appear in places Fordyce spots don’t, such as inside or around the anus, inside the vagina, and in men, on the groin and thighs. Anogenital warts (warts on the anus or genitals) are caused by human papilloma virus (HPV).
Fordyce spots on the penis
Fordyce spots on the penis are common. They can appear on the shaft of the penis, the head of the penis or the scrotum. Because they are more prominent when the skin is stretched, you might notice them most when you have an erection. The spots may feel uncomfortable during sex or start bleeding, but normally they don’t cause a problem.
Fordyce spots on the labia
In women, Fordyce spots can appear on the labia, the folds of skin around the vaginal opening. They are more common on the inner labia, the folds closest to the opening. Less commonly, they occur on the outer labia or the clitoris. Like Fordyce spots elsewhere, they appear in a symmetrical pattern (the same on both sides).
Fordyce spots on the labia can sometimes resemble milia, genital warts or molluscum contagiosum, a viral outbreak that causes small, pink or flesh-colored bumps. Molluscum contagiosum is contagious, as its name implies.
Fordyce spots treatment
If the spots itch or make sex uncomfortable, or you simply don’t like how they look, there are several treatments your dermatologist can use to remove them or make them less noticeable. He or she may recommend combining topical or oral treatments with laser treatments for the best outcome.
- Topical tretinoin (Retin-A). This cream, also used to treat acne, can reduce Fordyce spots or make them disappear through the process of exfoliation
- Oral isotretinoin. A brief course of this vitamin A derivative is sometimes effective in erasing Fordyce spots. The drug works best when combined with laser treatment.
- Laser treatment. Fordyce spots can be eliminated with CO2 lasers or pulsed-dye lasers. Pulsed-dye laser treatments may be preferred because the risk of scarring is lower
- Cryotherapy. Freezing the spots with a very cold substance such as liquid nitrogen or argon gas can destroy them.
- Topical trichloracetic acid (TCA). This acid shrinks or removes Fordyce spots by cauterizing (burning) them. It works best when used in conjunction with laser treatment.
- Electrohyfrecation. The doctor uses a small, handheld device to deliver a low-level electric current to the spot, which burns it away.
- Micro-punch surgery. After applying a local anesthetic, the doctor uses a small, pen-like device to remove the spots.
If you don’t feel the need to treat your Fordyce spots — they are perfectly natural, after all — you can help prevent them from getting larger by skipping the use of oily lotions, creams and other heavy skin care products. If you’re tempted to pop the spots, don’t. You may get a cheesy or watery liquid out of them, but they won’t go away, and you may end up with an infection. Scraping them off doesn’t work, either.
Medically reviewed by Lucy Chen, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Get Riverchase Updates in Your Inbox
"*" indicates required fields
13 Best Lip Balms for Dry Lips According to a Dermatologist
Choosing a lip balm seems pretty simple — flavored or unflavored? Tinted or untinted? Stick, pot or tube? But not all lip balms are created equal, and as you may have come to suspect, some can make dry lips feel worse. If you’re less than thrilled with your current lip balm, it’s time to start looking at ingredient lists or product recommendations to find the best lip balm to soothe and protect your dry, irritated or flaky lips.
“A surprising number of popular lip balms on the market contain ingredients that can irritate dry, chapped lips,” said Jeriel Weitz, DO, a board-certified dermatologist with Riverchase Dermatology. “If your lip balm makes your lips tingle, sting or burn, or if it makes your lips feel drier shortly after you apply it, stop using it.”
The best lip balms seal in moisture without inflaming or exfoliating the lips. Read on to learn what ingredients and products Dr. Weitz recommends.
Why are my lips so dry?
First things first: Why do you have dry lips to begin with? There are a few possible dry lip causes.
The skin on the lips is very thin, and unlike the skin on the rest of the face, it lacks oil glands, which makes lips vulnerable to dryness, peeling, itching and cracking. Dry, cold air makes lips more parched, as does sun exposure. Other factors that can cause dry lips include:
- Dehydration from not drinking enough fluids
- Breathing through your mouth
- Taking certain medications, such as Accutane (used to treat severe cystic acne), lithium and certain chemotherapy drugs
- Licking, biting or picking at your lips
- Holding jewelry, paper clips or other metal objects in your mouth
How to get rid of dry lips: Lip balm ingredients to embrace
To moisten and heal dry, chapped lips, choose a lip balm with one or more of the ingredients below. All of these ingredients act as occlusives, which means they create a physical barrier to seal in moisture and protect the lips from irritants.
- Petroleum jelly (petrolatum)
- Sunflower oil
- Cocoa butter
- Sweet almond oil
- Argan oil
- Castor seed oil
- Ceramides
- Dimethicone
- Hemp seed oil
- Mineral oil
- Shea butter
- Titanium oxide or zinc oxide (sun protective ingredients)
In addition to these occlusive ingredients, some lip balms contain humectants, which attract water. Humectants include glycerin, hyaluronic acid, aloe vera, honey, propylene glycol and urea.
Antioxidants such as vitamin C, vitamin E, niacinamide and polyphenols can also be beneficial. “Antioxidants work by preventing damage caused by environmental aggressors such as UV rays and pollution,” Dr. Weitz explained.
Lip balms ingredients to avoid
To avoid irritating dry, chapped lips, steer clear of lip balms with these ingredients. Some of them, such as camphor and menthol, are commonly found in “medicated” lip balms.
- Camphor
- Eucalyptus
- Flavors such as cinnamon, citrus and mint
- Fragrance
- Menthol
- Octinoxate or oxybenzone
- Phenol (phenyl)
- Propyl gallate
- Salicylic acid
Best lip balm picks
Below are Dr. Weitz’s favorite lip balms for day and night, all of which feature rich, hydrating, non-irritating ingredients.
Best lip balms with SPF
Wear a lip balm with SPF 30 or higher during the day so the sun won’t dry out or burn your lips. SPF lip balms also help protect you against lip cancer. Add one of the picks to your morning skincare routine and reapply as needed.
- Aquaphor Lip Protectant + Sunscreen
- Vanicream Lip Protectant/Sunscreen
- Sun Bum Mineral SPF 30 Sunscreen Lip Balm
- Raw Elements Lip Rescue SPF 30
- Salt & Stone Sunscreen Lip Balm SPF 30
- EltaMD UV Lip Balm Broad-Spectrum SPF 36
Best nighttime lip balms
Once the sun has set, you can switch to a lip balm that doesn’t contain SPF. Even if your lips don’t feel dry before you get in bed, it’s a good idea to apply lip balm to keep them from drying out overnight, especially if your bedroom is dry or you tend to breathe through your mouth when you sleep.
- Vaseline Lip Therapy
- Aquaphor Lip Repair
- SkinCeuticals Antioxidant Lip Repair
- La Roche Posay Nutritic Lip Balm
- Ilia Lip Wrap Reviving Balm
- Bioderma Atoderm Restorative Lip Balm
- Dr. Dan's CortiBalm (contains 1% hydrocortisone)
When to see a dermatologist
Using a non-irritating lip balm, drinking plenty of water and running a humidifier when the indoor air is overly dry should go a long way toward preventing and healing dry, chapped lips. Still have a parched pucker after a few weeks of TLC? Make an appointment with your dermatologist to rule out an underlying condition.
Health conditions that can contribute to dry lips include hypothyroidism (low thyroid) and certain autoimmune diseases, such as Sjögren’s syndrome and Crohn’s disease. Another condition, angular cheilitis, can lead to redness, inflammation and cracks in the corners of the lips. It’s caused by an overgrowth of a yeast called Candida that can happen when saliva collects in the corners of the lips. If your lips are constantly inflamed and scaly, it’s possible that you’re allergic to or sensitive to an ingredient in your lipstick or toothpaste.
Outdoor laborers and long-term sun worshippers have one more condition to look out for: farmer’s lip or sailor’s lip, known medically as actinic cheilitis. This precancerous lip condition is caused by chronic sun exposure. Symptoms include chronically dry, scaly or peeling lips that may have a sandpapery texture, whitish or yellowish patches and a blurred border between the lip and the skin. Treating this condition can prevent it from progressing to lip cancer.
Medically reviewed by Jeriel Weitz, DO
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water's Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.