Red welts suddenly cropping up on your skin can be alarming, but chances are they are hives, which in most cases are more itchy than dangerous. How to get rid of hives? One mild or moderate episode can usually be treated at home. If you have chronic hives, your dermatologist can develop a hives treatment plan for you.
What do hives look like?
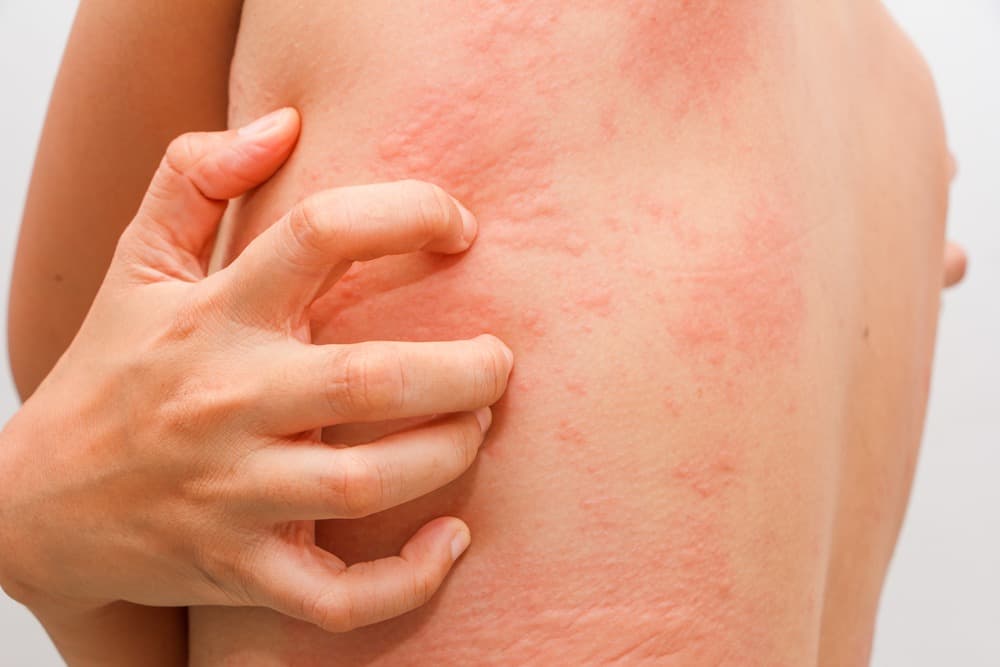
Hives, also called urticaria, are raised bumps or swollen-looking welts on the skin. “They can be as small as a pencil point or larger than your hand,” said Tara Duquette, PA-C, a certified physician assistant with Riverchase Dermatology.
The hives rash is usually pink or red in people with lighter skin, and skin-colored in people with darker complexions. Pressing on the bumps makes them turn light.
Hives can show up anywhere on the body, but they often appear on the torso, buttocks, upper arms and upper legs. They are typically very itchy, though you may feel a burning or tingling sensation instead. Sometimes they form large patches called plaques.
Along with hives, some people develop swelling deep in the lips, tongue or eyelids, a condition known as angioedema.
What causes hives?
Hives develop when your immune system releases a chemical called histamine in response to an allergen or something else you’re sensitive to. Histamine causes a chain reaction that results in inflammation and itching.
Allergens that can trigger hives include:
- Food
- Medication
- Pet dander
- Pollen
- Latex
- Bug bites
Other hives causes include:
- Hot or cold weather
- Sunlight (even without heat)
- Emotional stress
- Sweating
- Pressure on your skin from tight clothes or a purse strap
- Scratching your skin (dermatographic urticaria)
- Infections such as strep throat and COVID-19
- Radiation therapy
- Blood transfusions
Sometimes no cause can be identified. In many people with chronic hives, a trigger is never found.
How long do hives last?
Hives usually disappear in anywhere from a few minutes to a few days. Chronic hives, also called chronic spontaneous urticaria, can last much longer.
“Chronic hives come and go and can last for six weeks or more,” said Duquette. “They can be very itchy and can make it hard to sleep.”
When to see a doctor for hives
Make an appointment with your dermatologist if your hives last longer than a few days or they affect a large part of your body.
Call 911 or go to the emergency room immediately if you have swelling in your mouth or throat, you have trouble breathing or swallowing, you feel faint or you have a racing heartbeat.
How to get rid of hives: At-home and professional hives treatment
Hives treatment aims to reduce the inflammation caused by the release of histamines.
“In many cases, all you need is an oral antihistamine and cold compresses to soothe the itching,” said Duquette. If your hives are more severe, you may need something stronger.
If you have chronic hives, your dermatologist may refer you to an allergist to be tested for allergies, or to another doctor to be tested for underlying diseases, including autoimmune diseases. Some autoimmune diseases, such as lupus, can make you more susceptible to hives.
At-home care
To soothe your hives at home, apply cool compresses and take a non-drowsy over-the-counter antihistamine, following the instructions on the package. If you have it handy, apply Prax lotion (sold in drugstores), calamine lotion or an anti-itch lotion or cream that contains menthol.
While you’re waiting for the welt to disappear, wear soft, loose clothing, and avoid hot baths or showers and harsh or scented soaps.
Prescription treatment for hives
For a more severe hives outbreak, your dermatologist might prescribe a stronger antihistamine, such as desloratadine (Clarinex), and/or a corticosteroid cream. In some cases, an oral corticosteroid such as prednisone is needed to control the itching and inflammation.
Other hives treatments include doxepin (Silenor, Zonalon), which is an antidepressant that blocks histamine, and montelukast (Singulair), which is most often used to prevent and treat asthma attacks.
Chronic hives treatment
Chronic hives is often treated with antihistamines. If they don’t help enough, your dermatologist may suggest adding UV light therapy, also called phototherapy. An injectable medication called omalizumab is another option. It works by blocking the action of an immune substance called immunoglobulin E, which plays a role in hives.
If all else fails, immunosuppressant drugs may be prescribed to prevent the immune system from overreacting to hives triggers. These drugs can have serious side effects, so they usually aren’t prescribed unless you haven’t responded to other treatments. Examples of immunosuppressants used to treat hives include cyclosporine, methotrexate and hydroxychloroquine (Plaquenil).
For severe reactions: Epinephrine (EpiPen)
If you’ve had severe hives attacks or angioedema, or if the attacks continue despite treatment, your dermatologist may prescribe an EpiPen for you to carry. Self-injecting epinephrine works quickly to open a swollen airway if you develop swelling in the mouth or throat that prevents you from breathing.
Medically reviewed by Tara Duquette, PA-C
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.