Of all the rashes you or your child could develop, the scabies rash may be one of the most unexpected, and one of the hardest to ignore. The pimple-like bumps could be mistaken for symptoms of any number of other rashes and dermatitis, but another hallmark scabies symptom, severe itching, sets scabies apart.
“The itching can be relentless. In some cases, it’s almost unbearable,” said Ashley Falzone, MD, a dermatologist with Riverchase Dermatology. “It’s typically more intense at night and may prevent you from sleeping.”
Not everyone with scabies experiences this level of itching, but most do.
A scabies diagnosis often comes as a shock, since many people assume scabies affects only people in developing nations and those living in unsanitary conditions. But in fact, anyone can get it.
What is scabies?
Scabies is a parasitic infestation that develops when microscopic scabies mites (Sarcoptes scabiei var hominis) burrow into the outer layer of skin to lay eggs. Mite proteins and droppings in the burrowed tunnels trigger an allergic reaction that causes itching. Scratching may lead to sores, which could become infected.
Scabies mites exist around the world, but scabies infestations are more common in tropical countries and in crowded places where close physical contact is common. Young people, old people and those who have a compromised immune system are the most susceptible.
If you suspect scabies, see a dermatologist right away. Prompt scabies treatment will help avoid the spread of this contagious skin condition.
How to identify scabies
Severe itching is usually the first scabies symptom. The scabies rash may look like pimples or hives or bites, which may or may not form a line. In people with lighter skin tones, the bumps are pink or red. In people with dark skin, they may be skin colored, lighter than the skin or darker than the skin.
You’ll likely see the bumps on certain areas of the body, such as:
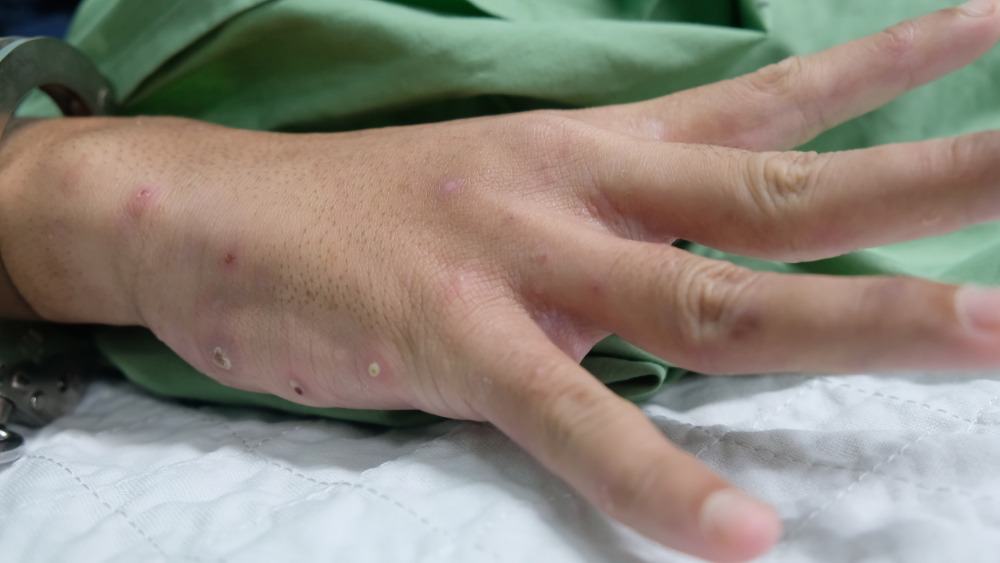
- Between the fingers and around the nails
- The inner wrist and elbow
- The armpit
- The waistline
- The lower buttocks
- The shoulder blades
- The penis
- The areola (the area around the nipple)
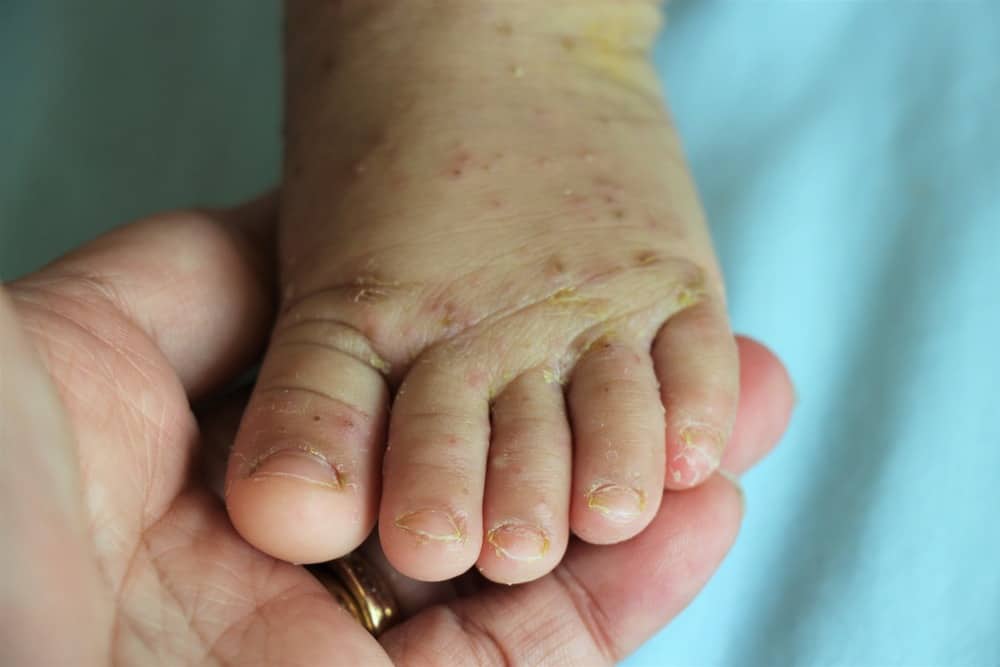
The scabies rash may be limited to one of these places, or you may see it on most of the body. In adults, the only places the mites doesn’t usually burrow are the head, face, neck, palms and soles of the feet. Babies and small children who develop scabies, on the other hand, often get it on their palms, the soles of their feet, their head and their neck.
In some cases, you may be able to detect the burrows the mites made when they tunneled into the skin.
“If you notice tiny, short, crooked, raised lines that are grayish-white or skin colored, you’re probably looking at burrows,” said Dr. Falzone.
To see pictures of scabies, scroll to the bottom of this article.
Crusted scabies (Norwegian scabies)
Crusted scabies, also called Norwegian scabies, is a severe form of scabies. People with classic scabies are typically infested with 10 to 15 mites, but people with crusted scabies may have up to 2 million mites in their skin.
What does crusted scabies look like? Bumps may or may not form (and if they do, they may or may not itch). The main symptom of crusted scabies is thick, crusty patches of skin, which may be yellowish or grayish. These patches are filled with mites and eggs.
The risk of developing crusted scabies is higher in people who use corticosteroids or immunosuppressants for a long period of time, and people who have certain other risk factors. Those risk factors include:
- A weakened immune system
- Advanced age
- HIV/AIDS
- Systemic lupus erythematosus
- Dementia
- Down syndrome
- Leprosy
Crusted scabies is extremely contagious and requires immediate treatment.
How does scabies spread?
Lengthy skin-to-skin contact spreads scabies, as does sharing items such as bedding, clothing and towels. In adults, scabies is often spread through sex.
“You typically won’t get classic scabies from a handshake or quick hug,” said Dr. Falzone.
Crusted scabies can be spread through briefer physical contact. It can also be spread when the skin crusts fall off. The mites and eggs they contain can survive and infect others for up to a week.
Infestations in the United States most often occur in nursing homes, long-term care facilities, schools and prisons.
Scabies treatment
If you, your child or another loved one is diagnosed with scabies, your dermatologist will prescribe a cream or lotion that contains a scabicide, a medication that kills the mites.
“It’s important that close contacts are treated at the same time, even if they don’t have scabies symptoms, to prevent spreading and re-infection,” said Dr. Falzone.
Permethrin cream is the go-to scabies treatment. Sulfur ointment may be even more effective, but many people are put off by its strong, unpleasant odor. Crotamiton lotion or cream is sometimes prescribed, but it’s less effective than permethrin and often requires two applications.
If the first treatment doesn’t work, the dermatologist might prescribe Lindane lotion, which is highly effective but may cause side effects, or an oral medication called ivermectin. Lindane lotion is not for use in small children.
Crusted scabies is often treated with a topical medication such as permethrin, plus ivermectin. The dermatologist may also recommend a keratolytic cream — a cream that breaks down the outer layer of skin — to reduce crusting. De-crusting the skin helps the topical medicine reach the mites.
Thoroughly cleaning and vacuuming the person’s surroundings is also a must. You’ll also need to do laundry. Throw bedding, towels and clothes used during the three days before treatment into the washer. Wash them on hot, then dry them on the hottest setting. Items that can’t be machine washed should be sealed in plastic bags for four to seven days.
Medically reviewed by Ashley Falzone, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
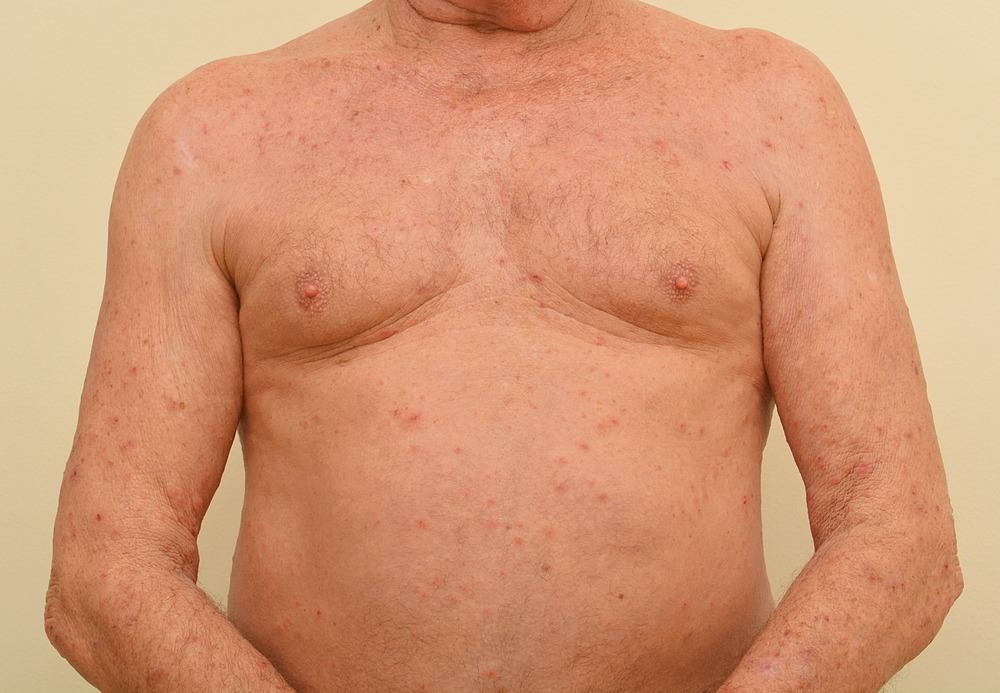
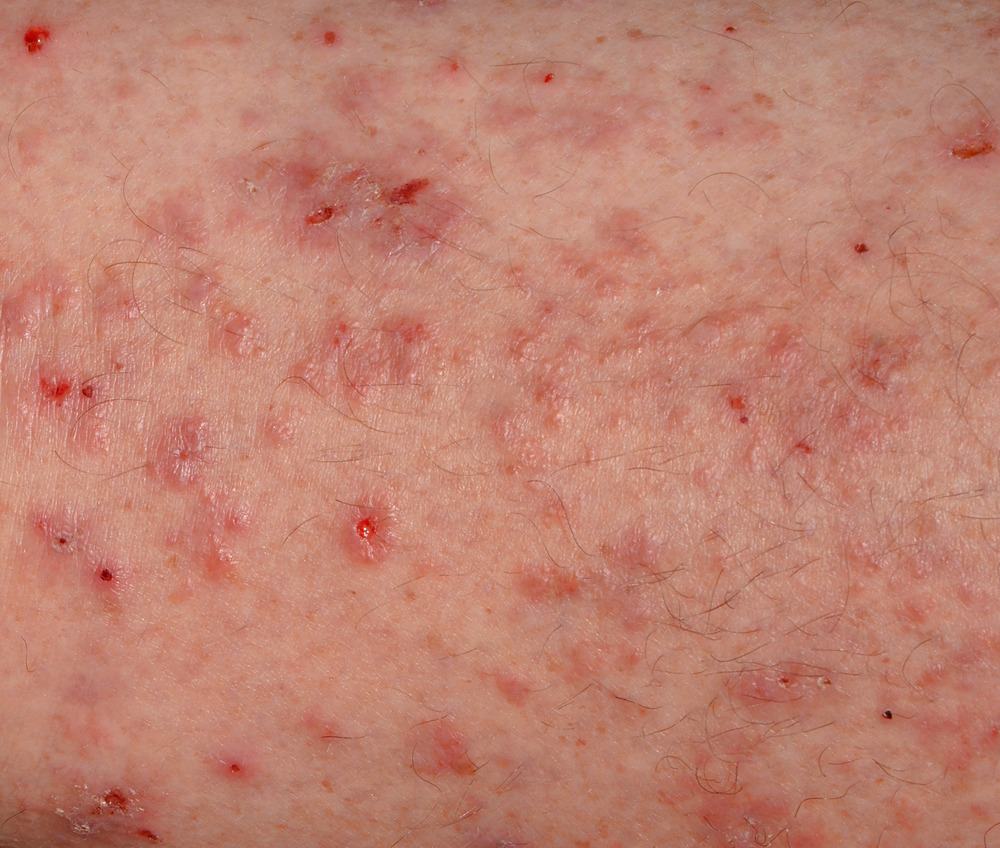
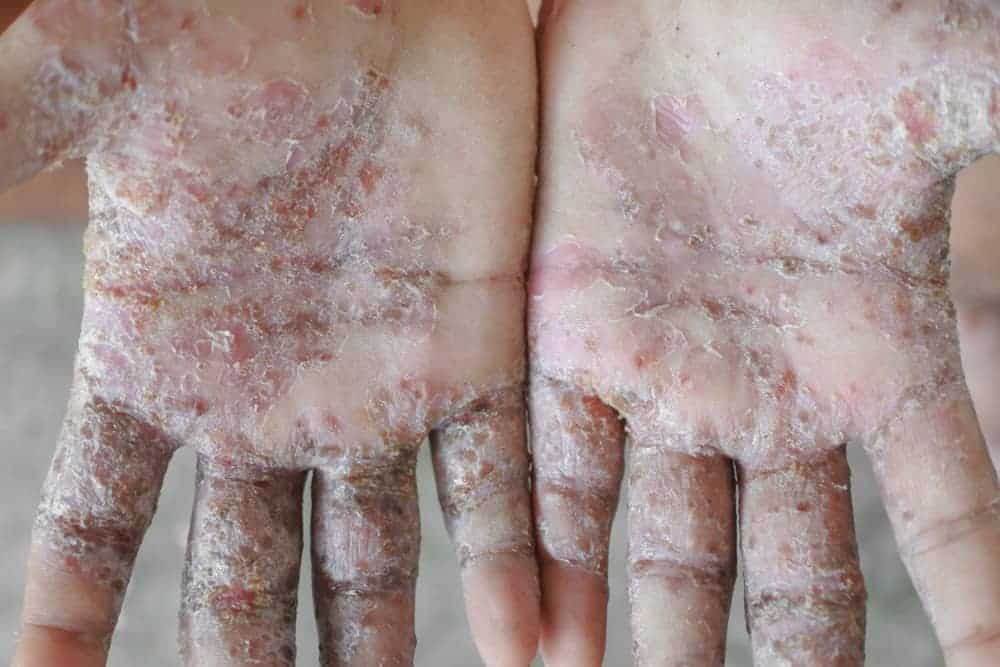
Scabies pictures
Scabies can look different in different people and at different stages. These pictures of scabies are examples. Your dermatologist can determine whether you or a loved one has scabies.