Dry, itchy skin and rashes are signs of eczema, a common inflammatory skin condition. It’s often called atopic dermatitis — but that’s just one kind. There are several types of eczema, including the six below. Identifying the one you have can be challenging, since many of the symptoms are the same, but knowing exactly what causes your itch can help you tame it.
Your dermatology provider can give you an accurate diagnosis based on your eczema symptoms and other clues and get you the eczema treatment you need.
1. Atopic dermatitis
The most common form of eczema, atopic dermatitis usually develops during childhood, though it sometimes appears for the first time after age 18. Genetics are partly to blame. Having relatives with eczema, hay fever, asthma or food allergies increases your risk. Your environment also plays a role: If you are genetically prone to this type of eczema, you may be more likely to develop it if you live in a city or a cold, damp area.
Like many types of eczema, atopic dermatitis often comes and goes. You may have periods of flares and periods of remission, which can last for years.
What it looks like: Dry, cracked and swollen skin with rashes that are red in light skin and brown, purple or gray in darker skin. You may see tiny, fluid-filled blisters that ooze and crust.
How it feels: Itchy.
Where it appears: Anywhere on the body. Atopic dermatitis is common on the hands, elbows and knees. In infants, it’s common on the face.
2. Contact dermatitis
Contact dermatitis, also called irritant or allergic contact dermatitis, develops hours or days after you touch something that irritates your skin or causes an allergic reaction. A dermatologist can help you figure out your triggers. Common ones include fragrances, hair dyes, hair straighteners, nickel (found in jewelry and belts, for example), latex and plants such as poison ivy.
What it looks like: A rash that’s hot and swollen. Skin is dry and can crack. You may have fluid-filled blisters that ooze and crust. Round welts (hives) may appear.
How it feels: Itchy, stinging, tender, burning.
Where it appears: Anywhere, but most often the hands, as well as areas where you apply personal care products, such as your face, scalp and underarms.
3. Hand eczema
Hand eczema affects the hands only. It can be an occupational hazard for people such as hairdressers and metal workers. Hand eczema also affects people who wash their hands a lot, such as healthcare workers. You may be at increased risk of hand eczema if you have persistent or severe atopic dermatitis (or had it as a child) or are exposed to cold, dry weather and dry indoor air.
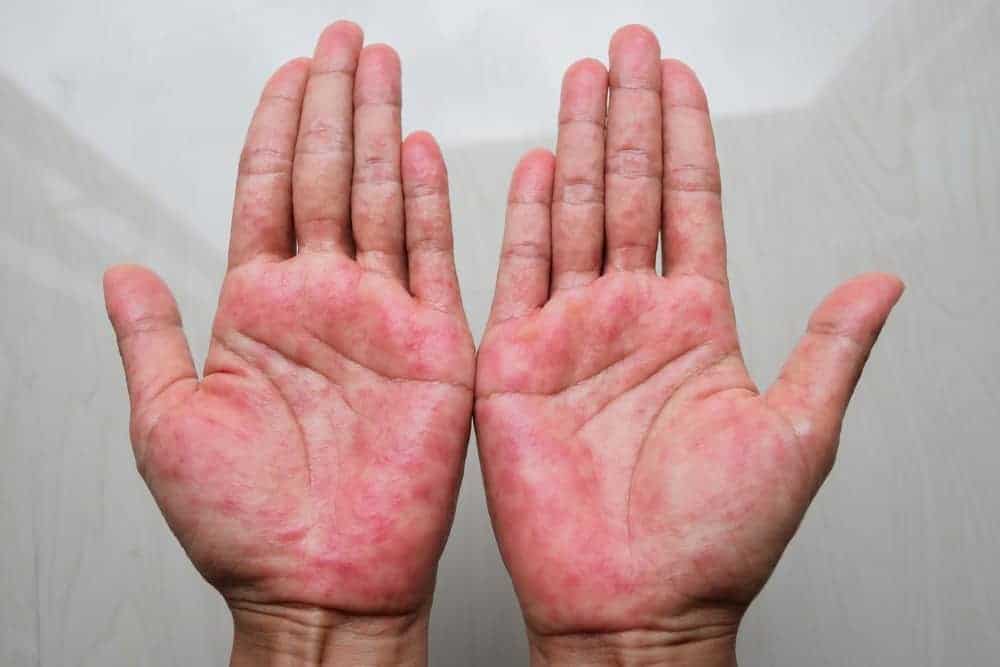
What it looks like: Dry, chapped and scaly hands with patches of red or dark brown skin, depending on your skin tone. You may develop blisters, crusting and deep cracks that could bleed.
How it feels: Itching, burning.
Where it appears: The top of the hands, the spaces between the fingers, and the palms. The wrist may also be affected.
4. Dyshidrotic eczema
Dyshidrotic eczema causes small blisters on the hands or feet. The condition isn’t well understood and can be hard to treat. It’s thought to be caused by a hypersensitivity to a substance such as metal (especially nickel), certain medications (such as aspirin and birth control pills), tobacco or ingredients in personal care products such as shampoo. If you have the condition, you may experience flares due to stress, changes in weather and sun exposure.
What it looks like: Small blisters that may be wet with sweat. As the blisters heal, the skin becomes dry and peels.
How it feels: Itching, burning, pain, prickly feeling.
Where it appears: The hands and feet, specifically the palms, fingers, toes and bottoms and sides of the feet.
5. Nummular eczema
This type of eczema, also called discoid eczema, has many possible triggers, including severe stress, a skin injury or infection, heavy alcohol use, dry air and heat and humidity. You may be more likely to develop nummular eczema if you have atopic dermatitis, contact dermatitis, very dry skin or poor blood flow in your legs. Some medications, particularly those that can dry the skin, can contribute to flares. They include isotretinoin (Accutane), statins and diuretics.
What it looks like: Tiny bumps or blisters that may join together to form raised, coin-shaped spots. In people with light skin, the spots are pink or red. In people with dark skin, the spots may be brown or lighter than your skin tone. They may ooze fluid. The skin between the spots is typically very dry.
How it feels: Very itchy, stinging.
Where it appears: The forearms, legs and backs of the hands.
6. Stasis dermatitis
Stasis dermatitis, also called venous eczema, can occur in anyone who has poor circulation in the legs caused by venous insufficiency. It usually affects the lower legs. You’re more likely to develop it if you have varicose veins, obesity, high blood pressure, heart disease or kidney disease or if you have been pregnant several times. Even standing or sitting for prolonged periods can lead to stasis dermatitis in people who are vulnerable.
What it looks like: Dry skin that may be scaly and discolored. Wounds may develop.
How it feels: Itchy, sore to the touch.
Where it appears: The lower legs, especially the skin on top of varicose veins.
Eczema treatments
Some types of eczema can be challenging to treat, but dermatologists have many ways to get even stubborn cases under control.
Your dermatologist can develop a custom treatment plan based on your type of eczema and its severity. The plan may include topical corticosteroids or non-steroid creams. Other eczema treatments are light therapy (phototherapy) and, for persistent cases that are moderate to severe, oral medicines or injectable biologic medicines that calm the immune system. If your eczema seems to be triggered by an allergy, your dermatology provider may recommend an antihistamine or suggest allergy testing.
Avoiding your eczema triggers, taking shorter, cooler showers and using a thick moisturizing cream or ointment to help keep the skin’s outer layer intact are other smart strategies for reducing flares.
Medically reviewed by Michael Cohen, DO
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.