Why Is My Skin So Dry Even When I Moisturize?
You faithfully slather on moisturizer morning and night, but you still have tight skin that feels parched and may be flaky or itchy. What’s the deal? If the mystery of “Why is my skin so dry even when I moisturize?” has you stumped, discover some common reasons why moisturizer doesn’t work and how to fix dry skin for more than a few minutes at a time.
Your moisturizer is too light
Frequently, the reason a moisturizer doesn’t work is that it’s the wrong product for your skin type. Light moisturizers and lotions typically contain a lot of water. That means they have less of the lipids (fats, oil) that lock in moisture.
Dry skin responds best to heavier creams rather than lotions or water-based gels. Good ones to try include Eucerin Original Healing Cream and CeraVe Moisturizing Cream. For dry hands, you may need a dedicated hand moisturizer such as Eucerin Advanced Repair Hand Cream.
Choose a moisturizer labeled “fragrance free,” since fragrances can irritate dry, sensitive skin. Don’t pick one labeled “unscented” as it may contain chemicals that cover up the smell of the other ingredients.
Ointments, while they may be greasy, are even better than creams for very dry skin. Apply an ointment such as petroleum jelly or Aquaphor Healing Ointment to your driest patches of skin.
You need to exfoliate
If you never exfoliate, a pile-up of dead skin cells may be preventing your moisturizer from penetrating. The solution to your dry skin could be as simple as regularly sloughing off those dead cells with a mild chemical exfoliant. Look for an exfoliating face wash or body wash that contains salicylic acid, glycolic acid or lactic acid and use it once or twice a week.
You’re moisturizing at the wrong time
There’s really no wrong time to apply moisturizer, but there is one time you definitely should: right after you pat yourself dry from a shower or bath, while your skin is still slightly damp.
Your wrinkle cream or acne treatment is drying out your face
Over-the-counter retinol products and prescription retinoids such as tretinoin are great for treating wrinkles, but they can make your skin dry and flaky. That’s because they speed up the skin’s natural exfoliation process. Use them sparingly at first. You may need to start with a lower-dose product. Your dermatologist can recommend or prescribe the right anti-wrinkle product for you and advise you whether to put on moisturizer before or after.
Topical acne treatments can also dry out your face. Talk to your dermatologist about the best way to treat your acne.
Your habits are robbing your skin of moisture
Love long, steamy showers? Your dry skin doesn’t. Keep showers short—less than 10 minutes—and use warm water, not hot. If you don’t sweat a lot, try showering less frequently than once a day.
Other habits that can dry the skin include:
- Using a drying soap, such as a deodorant soap, instead of a gentle skin cleanser such as Dove
- Using toners and other skincare products that are too harsh for your skin type
- Wearing tight clothes that rub against the skin
- Smoking cigarettes
- Swimming in chlorinated pools
You’re getting older
Once you reach your 40s, your skin’s production of sebum (oil) plunges and continues to decline less dramatically as you get older. Switching to a heavier cream or ointment will do a better job of keeping aging skin hydrated and can even reduce the appearance of fine lines.
You have certain skin conditions or other health issues
Several common skin problems cause dryness, flaking and peeling, including eczema, contact dermatitis and psoriasis. But even diseases you might not think affect the skin can leave it parched. These include diabetes, hypothyroidism, lymphoma and kidney failure. Dialysis for kidney disease leaves skin even drier. Talk to your doctor for advice.
You take medications that dry out the skin
Dry, peeling skin is a side effect of many drugs. Common culprits include Accutane, beta blockers, hormonal birth control, cholesterol-lowering statins, diuretics (“water pills”) and chemotherapy drugs. Using a thicker moisturizer or switching to an ointment can help.
You’re deficient in certain nutrients
Stubborn dryness may occur if your body is low in vitamin A, vitamin D, iron, niacin or zinc, all of which are a must for healthy skin. Talk to your doctor about whether you might be deficient in one of these nutrients, and if you are, whether or not to take supplements.
Extreme calorie limitation due to anorexia also deprives the skin of nutrients it needs to stay hydrated.
You’re frequently exposed to dry air
If you live in a place where the air is cold and dry, or the air in your home is dry due to forced air heating in the winter or even air conditioning in the summer, keeping your skin moist may be an uphill battle. In addition to switching to a heavier cream or ointment, try running a humidifier in the room where you spend the most time.
Medically reviewed by Jennifer Wong, DO
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Fingernail Ridges: What Causes Them?
Your nails may hold subtle clues to your overall health. So, what does it mean if you have fingernail ridges? They’re not uncommon, especially with age, and usually, they’re nothing to worry about. Occasionally, however, vertical ridges on nails can be a sign of an underlying medical issue, as can deeper horizontal ridges on nails. What exactly do ridges indicate? Read on for answers and to learn how to get rid of ridges on nails.
Why do my nails have ridges?
The causes of vertical and horizontal fingernail ridges are different, so check out the possible causes for the type of ridges you have.
Causes of vertical ridges on nails
Aging is one of the most common causes of tiny vertical nail ridges (onychorrhexis), which extend from the bottom of the nail to the tip. Most people have some faint vertical nail ridges when they’re younger. The ridges may become more pronounced over time as the nails naturally get thinner and more brittle.
Sometimes, vertical ridges on nails are a sign of vitamin deficiency or other nutrient deficiency. You may notice them if you have an eating disorder or if you’re low in nutrients such as iron, folic acid (vitamin B9) or protein.
Health conditions that can cause vertical fingernail ridges include:
- Dry skin accompanied by dehydration of the nail plate
- Psoriasis, lichen planus and other inflammatory skin conditions
- Hypothyroidism
- Rheumatoid arthritis
- Rare diseases such as amyloidosis and Witkop syndrome
Repeated trauma to the nails during manicures or pedicures and chemicals found in nail polish removers and cuticle softeners can also make vertical nail ridges more visible.
Causes of horizontal ridges on nails (Beau’s lines)
Grooves or indentations running across your nail are called Beau’s lines. You may have a single groove on a single nail or one or more grooves on all your nails.
Horizontal nail ridges usually develop when nail growth is disrupted by something. Nail trauma is one possible culprit—maybe you closed a door on your finger or dropped something heavy on your toe. Using artificial nails or getting gel manicures for long periods can also harm the nails and lead to horizontal ridges.
Medical causes of Beau’s lines include:
- Eczema
- Psoriasis
- Zinc or protein deficiency
- Extreme emotional stress or anxiety
- Conditions that interfere with blood flow to the nail, including peripheral vascular disease, diabetes, hypothyroidism and Raynaud’s disease
- Chronic kidney disease
- Severe illness from pneumonia, strep, COVID-19 or another infection
- Chemotherapy
How to get rid of ridges on nails
Make an appointment with your dermatologist if you’ve developed fingernail ridges or any other nail changes. Chances are they’re nothing to worry about, but it’s important to determine if there’s a medical cause that requires treatment, especially if you have horizontal nail ridges.
Treating or managing the underlying medical condition or nutrient deficiency usually allows smoother, healthier nails to grow in. It may take several months to see a difference, since fingernails grow only a few millimeters per month and toenails grow even slower. If you have horizontal ridges caused by an illness or other short-term issue, the ridges should grow out with the nail plate over time.
Unfortunately, it’s not possible to get rid of age-related nail ridges. Using a nail buffer can smooth them a bit, but if you buff too often—say, more than once a month—you can weaken the nails. Still, there are several things you can do to avoid dry, brittle nails, which make ridges look more pronounced.
- Apply a heavy moisturizing cream to your nails and cuticles during the day and before going to bed (cover your hands and feet with thin cotton gloves and socks to protect your sheets).
- Don’t bite or pick at your nails or cuticles.
- Don’t cut your cuticles or push them back.
- Wear gloves when you’re working with harsh products such as household cleaners.
- Take breaks from gel manicures and artificial nails, which can dry out and weaken nails.
- When you cut your nails, stick to traditional shapes: Fingernails should be trimmed in a curved shape and toenails should be cut straight across.
Medically reviewed by Stephanie McNamara, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Get Riverchase Updates in Your Inbox
"*" indicates required fields
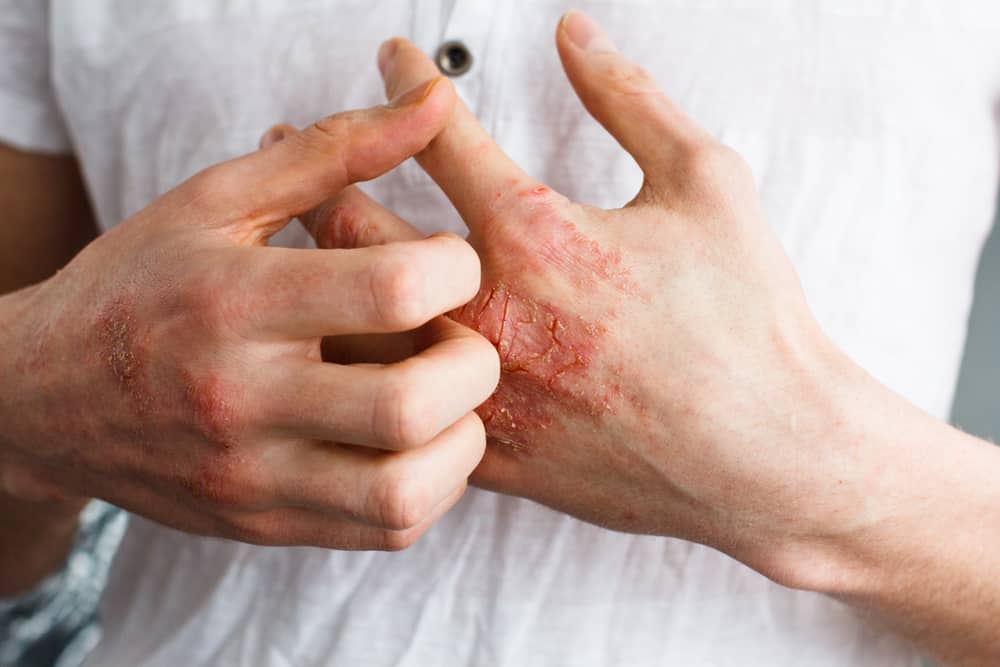
Treating Stress-Related Eczema on Hands
Stress and hand eczema deliver a one-two punch: Not only can stress trigger hand eczema flares in some people, but dealing with everyday life when you have itchy, red, blistering, cracked skin can cause stress, which—you guessed it—can make eczema on the hands worse. So how do you treat stress-related eczema on the hands?
You may be able to tame flares by using an over-the-counter hand eczema cream or hydrocortisone cream, or even taking oral antihistamines. But if stress or anxiety sends your eczema into overdrive, you’ll want to add some stress reduction techniques to your eczema treatment plan.
Read on to learn more about stress-related eczema on hands and what you can do to make it go away.
Can stress cause eczema?
Stress eczema is real. While hand eczema is often caused by frequent or prolonged water exposure, contact with irritating chemicals or contact with allergens such as nickel, stress can worsen eczema, especially a kind of eczema called dyshidrotic eczema. This type of eczema causes tiny, itchy, painful blisters, typically on the palms.
How does stress compound the problem? By causing additional inflammation, which lies at the root of the condition. Stress releases chemicals such as cortisol. Over time, too much cortisol causes an immune system reaction that creates inflammation throughout the body, including the skin. Skin inflammation can lead to swelling and rashes.
In addition, stress that’s poorly managed can increase the risk of anxiety and depression, which are also associated with increased inflammation.
Does stress cause your palms to sweat? That sweat can make dyshidrotic eczema worse.
How to treat stress-induced eczema on your hands
If you have hand eczema, start by seeing a dermatologist. They can give you an accurate diagnosis, help you identify your triggers and develop a customized treatment plan to get the eczema under control.
Hand eczema treatments
To treat hand eczema, your dermatologist may recommend an over-the-counter antihistamine and prescribe a topical medicine. If your eczema doesn’t improve significantly, another treatment option is phototherapy, aka light therapy. For more severe cases, dermatologists sometimes prescribe oral immune system suppressants or strong medicines known as biologics, which may be given by injection.
Your dermatologist will probably also suggest that you:
- Avoid excessive water exposure, for instance by taking shorter showers and washing dishes in the dishwasher instead of by hand or wearing waterproof gloves while you wash them.
- Refrain from using alcohol-based hand sanitizers when possible.
- Avoid harsh cleansers, detergents and other chemicals (and wear cotton-lined gloves when you can’t).
- Wear gloves when you work with your hands in the garden or elsewhere.
- Wear disposable gloves if preparing onions or citrus fruits irritates your hands.
It’s also important to use an emollient, thick moisturizer or ointment, especially after you wash your hands or shower. Look for a moisturizer with bonus ingredients such as ceramides and glycerin to help repair the outermost layer of skin, called the skin barrier. The skin barrier protects your hands against dryness and irritation, and stress can weaken it.
Stress management strategies
If you think stress is making your hand eczema worse, ask yourself what you can do to reduce or eliminate the biggest sources of stress in your life. At the same time, adopt daily habits that help you feel calmer. It may take some trial and error to find ones that work for you, but research has shown that these approaches can help relieve stress and anxiety:
- Mind-body practices such as yoga and meditation
- Deep breathing exercises
- Progressive muscle relaxation (sit or lie down and tense and then relax one muscle group at a time)
- Regular physical activity, such as brisk walks
- Spending time outdoors or watching nature videos
- Hanging out with family and friends, especially people who are good at listening or offering practical support
- Cultivating a hobby
If you find that you can’t quite manage stress or anxiety on your own, seek help. You might look for a therapist who offers cognitive behavioral therapy (CBT). According to the American Psychological Association, CBT works by teaching people how to think differently about the things that stress them out or trigger anxiety.
The combination of treatments from your dermatologist and lifestyle changes should help you get control of stress-related eczema on your hands so you can text, type and button your shirt with hands that don’t itch, burn, blister or bleed.
Medically reviewed by Stephanie A. McNamara, MD
Written by Maura Rhodes, a writer and editor specializing in health and well-being.
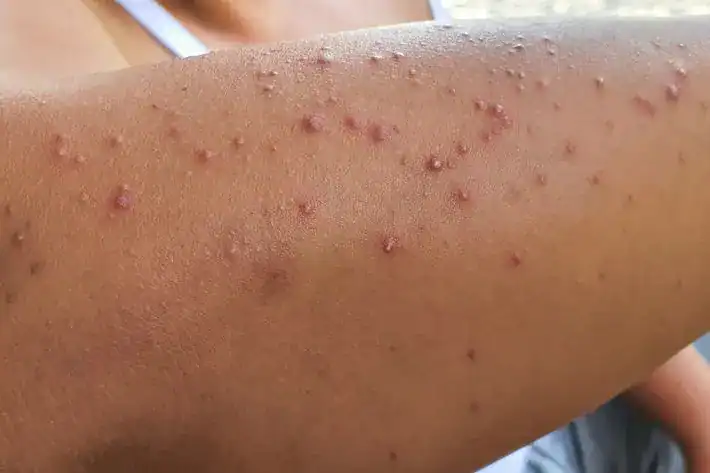
Pimples on Your Arms? How to Get Rid of Arm Acne
Acne is an equal opportunity annoyance: Wherever you have oil glands, you can get breakouts. Pimples on your arms, however, might be some other skin condition masquerading as acne. If you want to know how to get rid of arm acne, first make certain that’s what you’re dealing with. Your dermatologist can tell you for sure.
Arm 'pimples': What else could they be?
Sometimes, arm acne really is acne. But often, what looks like acne on arms is one of these three problems instead.
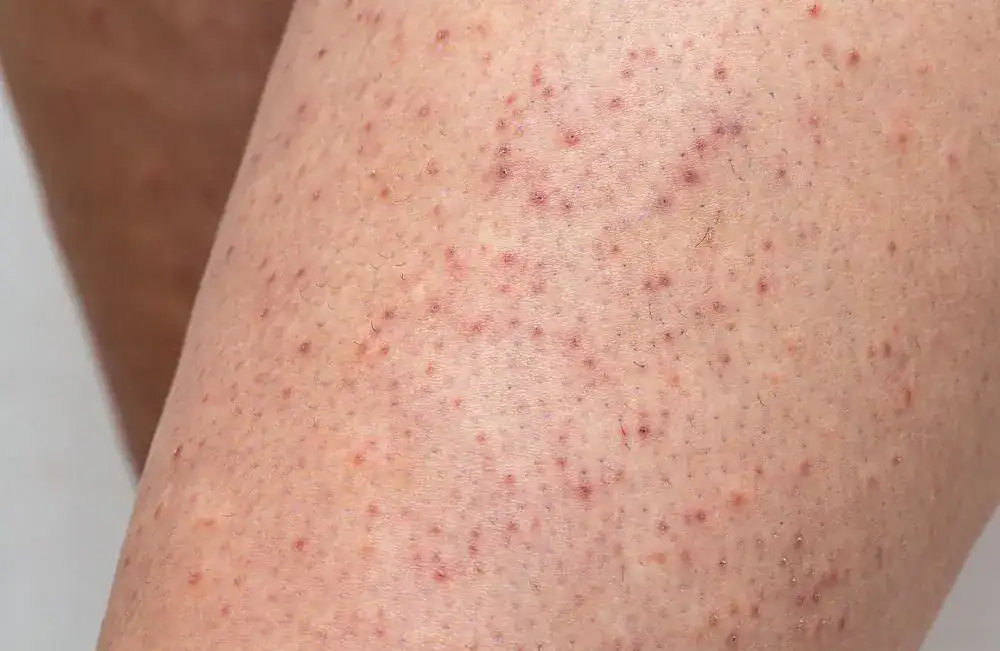
Keratosis pilaris
If your arms look like the skin of a plucked chicken, you could have keratosis pilaris (KP), also called chicken skin. It happens when the hair follicles are clogged by a buildup of keratin, a protein found in skin. The hallmark is small, rough, red or white bumps that may be itchy. What looks like upper leg acne could be KP, too. KP is especially common when the skin is dry.
It’s practically impossible to get rid of these bumps entirely, but you can minimize them by using an over-the-counter, acid-based exfoliating product followed by a rich moisturizer.
Folliculitis
Folliculitis—literally, swelling of the hair follicles—causes acne-like bumps that may have a red ring around them. The bumps may itch and contain pus. Sometimes the cause is unknown, but folliculitis usually happens when bacteria enter the follicles. You’re more susceptible if you wear tight clothes that rub against you, sweat a lot or use hot tubs that aren’t well maintained.
Applying a warm compress for 15 to 20 minutes several times a day should help. Your dermatologist might prescribe an antibiotic cream or recommend using an anti-bacterial cleanser.
Hives
Allergic to something? A sudden outbreak of itchy raised bumps on your arm may be hives. A case of hives may come and go quickly or last for months (chronic hives). Common triggers include pet dander, pollen, bug bites, latex and certain foods and medicines, so if you know you’re allergic to any of these, it’s best to steer clear of them. Hives can also be brought on by extreme stress and even some viral or bacterial infections, like strep throat.
If you break out in hives, you can relieve the itching with cold compresses, anti-itch cream and an oral antihistamine recommended or prescribed by your doctor. Seek immediate medical help if you have trouble breathing.
Why do I have acne on my arms? (True acne)
If you really do have arm acne—blackheads, whiteheads or pimples filled with pus—it’s caused by the same problems that cause acne elsewhere, namely, pores clogged by dead skin cells, dirt and oil, which block the flow of oxygen and allow bacteria to thrive. Factors that might put you at higher risk of arm acne include:
- Your genes
- Hormone fluctuations during adolescence or pregnancy
- Medications that cause can acne, including corticosteroids, lithium, isoniazid (an antibiotic) and some cancer drugs
- Chemical sunscreens, which can cause breakouts in some people
How to get rid of arm acne: An array of treatment options
Managing true arm acne comes down to fighting clogged pores and bacteria.
“There are many treatment options for body acne, ranging from body washes to prescription medications,” said Roxanna M. Menendez, DO, a board-certified dermatologist with Riverchase Dermatology. Here are some of the go-to approaches to treating arm acne.
Benzoyl peroxide body wash
"For inflammatory acne on the arms and the trunk, I usually start by recommending a 10% benzoyl peroxide body wash or foaming cleanser,” said Dr. Menendez. (If you have red, swollen, pus-filled blemishes, you probably have inflammatory acne.) “Leave it on for three to five minutes before rinsing well,” she added. This gives the benzoyl peroxide time to sink in and do its job of killing bacteria.
If the body wash over-dries or irritates your skin, switch to one with a lower percentage of benzoyl peroxide. Keep in mind that while a 10% benzoyl peroxide product is often effective for body acne, it may be too strong for your face.
Avoid exfoliating scrubs. "These can actually make acne worse,” said Dr. Menendez.
Exfoliating salicylic or glycolic acid wash
“For patients with more comedonal acne—whiteheads or blackheads—I suggest an exfoliating salicylic or glycolic acid body wash,” said Dr. Menendez. Some body washes contain both benzoyl peroxide and one or more of these chemical exfoliants.
Topical retinols or retinoids
These products, such as over-the-counter Adapalene (Differin), are vitamin A derivatives that help acne by unclogging pores. They come in different forms, including creams, lotions and gels. Stronger prescription versions are available from your dermatologist.
Topical and oral antibiotics
For stubborn cases of body acne, your dermatologist might prescribe a topical antibiotic or even an oral antibiotic to get bacteria growth under control.
Lifestyle changes
Medicines aside, a few simple steps can help keep arm acne at bay.
Wear looser sleeves. If you favor tight, long-sleeved tops, choose tops with looser sleeves and breathable fabric.
Wash yourself, and your clothes, after your sweat. Hit the shower right after a workout or other sweat-inducing activity. Wash your skin, but don’t scrub it. Then toss your clothes into the laundry pile so you don’t wear them again and re-introduce sweat and bacteria to your skin.
Wash your sheets and towels regularly. Cotton absorbs oil and retains bacteria.
Use (the right) sunscreen. Don’t think that sun exposure will clear up your arm acne. If anything, it could make it worse by drying out your skin, causing it to produce more oil to compensate. If you think your sunscreen may be contributing to your arm acne, switch to an oil-free sunscreen. Some people have better luck with mineral sunscreens, which contain zinc oxide and/or titanium dioxide and stay on top of the skin rather than sinking in.
If over-the-counter products along with these lifestyle measures don’t help your arm acne, see your dermatologist. They can determine if you have pimples on your arms or something else entirely and develop a treatment plan that’s right for you.
Make an appointment today at one of our locations near you.
Medically reviewed by Roxanna M. Menendez, DO
Written by Maura Rhodes, a writer and editor specializing in health and well-being.
Keratosis Pilaris Treatment: How to Get Rid of Chicken Skin
If clusters of small red or white bumps are making your skin look like freshly plucked poultry flesh and feel like sandpaper, you’re probably wondering how to get rid of keratosis pilaris, aka chicken skin. Chicken skin on the arms can banish short-sleeved shirts and sleeveless tops to the back of the drawer, and bumps on the butt cheeks or face can be even more embarrassing. In most cases, keratosis pilaris treatment is simple.
“The condition is harmless and may eventually resolve on its own,” said Stephanie McNamara, MD, a dermatologist at Riverchase Dermatology. “But if it bothers you, you can reduce the symptoms at home with regular use of an exfoliating product and a good moisturizer.” In extreme cases, she added, if keratosis pilaris self-care measures don’t work, you may want to see a dermatologist for prescription topical medication or perhaps laser treatment.
What is keratosis pilaris?
Chicken skin is caused by blocked hair follicles, which is why it shows up only in places that have hair—typically the backs of the arms, the front of the thighs, the cheeks and the buttocks. Clogging the follicles are dead skin cells and keratin, a protein found in skin, hair and nails. On fair skin, the bumps may be whitish, skin-colored, red or pinkish purple. On dark skin they may be brownish black.
It’s not clear what causes keratosis pilaris, though genes play a role. It tends to show up in childhood and often flares at puberty. Between 50 percent and 80 percent of teens have keratosis pilaris, and approximately 40 percent of adults develop it. It’s slightly more common in females and more common in people with close family members who have it.
Certain medical conditions and treatments may increase the risk of keratosis pilaris, including:
- Asthma
- Hay fever
- Overweight or obesity
- Eczema
- Ichthyosis vulgaris (a condition in which skin becomes flaky)
If you’re prone to keratosis pilaris, certain circumstances can make it worse.
“The bumps often appear in cold weather, when skin is especially dry,” said Dr. McNamara. “Lack of hydration can exacerbate keratosis pilaris, and some people find that stress can also cause it to flare up.”
Keratosis pilaris treatment
To treat keratosis pilaris, first see your dermatologist, who can confirm that the bumps aren’t caused by something else — say, acne or a rash.
Next, “Start with a simple two-step approach,” said Dr. McNamara. “Apply an acid-based, over-the-counter topical exfoliating product to loosen and slough off dead skin cells.” Ingredients to look for include:
- Lactic acid
- Salicylic acid
- Glycolic acid
- Urea
Skip the body scrubs for keratosis pilaris that offer physical exfoliation. They may be too harsh for the skin.
“Then, follow up with a moisturizing cream to lock in moisture and prevent skin from becoming dry and flaky,” said Dr. McNamara. If the bumpy skin itches, try using an over-the-counter corticosteroid cream, but follow the directions on the package, and don’t use it more often than recommended.
Tempted to use an exfoliating sponge, loofah, gloves or brush? Don’t. “It really is never beneficial to use abrasive apparatus on the skin, unless it's the soles of the feet for callus removal,” said Dr. McNamara.
Keratosis pilaris creams and lotions
A variety of creams and lotions are designed to treat rough, bumpy skin via chemical exfoliation. When it comes to the best cream for keratosis pilaris, here are some of Dr. McNamara’s top picks.
AmLactin KP Bumps Be Gone
This body cream combines 15% lactic acid plus a moisturizer to exfoliate and hydrate the skin.
CeraVe SA Cream for Rough & Bumpy Skin
A salicylic acid cream, this also contains lactic acid, hyaluronic acid and niacinamide (vitamin 3). Ceramides lock in hydration for all-day moisture.
Eucerin Roughness Relief Lotion
If you find creams to be too thick, consider this fast-absorbing lotion, which contains urea for exfoliation and shea butter for moisturizing.
Touch KP Exfoliating Lotion
Some people swear by this lotion, which contains 12% glycolic acid and 2% salicylic acid and reduces redness as well as minimizing bumps. Because of the high glycolic acid concentration, you may experience a burning sensation when first using the lotion.
Professional treatment for keratosis pilaris
If your keratosis pilaris is stubborn or severe, your dermatologist may recommend a prescription topical product. Laser therapy is another option if the practice is equipped with the right lasers.
One effective laser treatment is IPL (intense pulsed light), which uses high-intensity pulses of light to smooth the skin and lighten dark spots. A CO2 fractional laser is another option for smoothing the skin and also improving the look of wrinkles and dark spots. Some skincare practitioners recommend microdermabrasion to enhance the effects of laser resurfacing treatments.
Treating keratosis pilaris may take some trial and error. Start with over-the-counter skin care products, experiment to see what works best, and give them time to work—they aren’t instant cures. Don’t skip the moisturizer, which is essential. If you’re not satisfied with the results of keratosis pilaris self-care after you’ve tried several products, see your dermatologist for help.
Medically reviewed by Stephanie McNamara, MD
Written by Maura Rhodes, a writer and editor specializing in health and well-being.
How to Get Rid of Skin Tags Without Hurting Yourself
Skin tags are incredibly common and completely harmless. There’s no need to remove these fleshy little growths that protrude or hang from the skin—but plenty of people prefer to get rid of them, either because they rub against their clothes or they simply look unattractive. Want to know how to get rid of skin tags? Rule number one: Don’t try to do it yourself. There are good reasons to leave skin tag removal to a dermatologist.
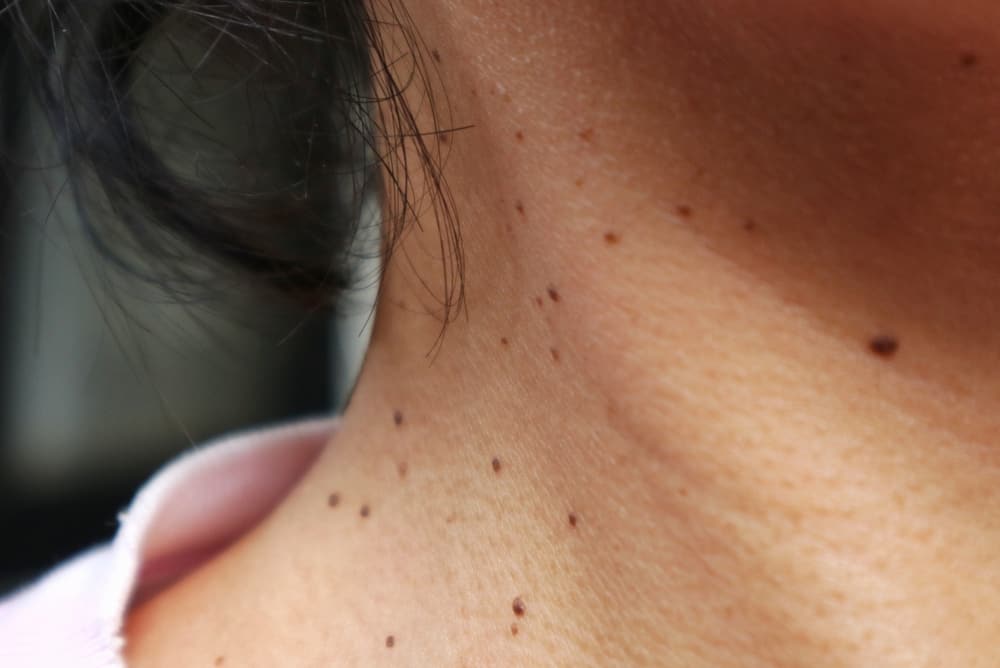
What are skin tags?
Skin tags (medical term: acrochordons) are soft, noncancerous tumors made up of collagen fibers, nerve cells and small blood vessels wrapped in layers of skin. They may take the form of flat bumps or growths that dangle from the skin on a short, thin stalk. Skin tags are usually small (2 to 5 millimeters), but some can become as long as half an inch. They may be the same color as your skin or darker.
These growths can appear on any part of your body, but they’re most likely to develop in areas where skin rubs against skin, creating friction. Common locations include the armpits, eyelids, groin and beneath the breasts. Skin tags on the neck are also common, possibly due to clothes or jewelry rubbing against the neck.
If a skin tag becomes uncomfortable or irritated, or it bleeds, skin tag removal may be recommended. This tends to happen if a skin tag is located in an area you shave or where clothing, jewelry or a seat belt rubs against it. It’s also fine to have a skin tag removed just because its appearance bothers you.
What causes skin tags?
The causes of skin tags are unclear, but there are several possible triggers in addition to friction. You’re more likely to get skin tags if you:
-
- Are obese or have loose, sagging skin, which creates more skin folds
- Have relatives with skin tags
- Have diabetes or metabolic syndrome, a group of conditions that include high blood pressure and high blood sugar
- Have Crohn’s disease (an inflammatory bowel disease) or colon polyps
- Are pregnant
- Have a hormonal condition such as acromegaly (an excess of growth hormone) or polycystic ovary syndrome
- Have acanthosis nigricans, a skin condition that causes dark, velvety patches
Dangers of skin tag removal at home
Tempted to get rid of skin tags yourself? As badly as you may want them gone, cutting or clipping them off hurts—a lot. And it can cause uncontrollable bleeding and infection. The damage may be even worse if you use nail clippers or scissors on skin tags near your eye or genitals.
There’s an even bigger risk to home remedies for skin tags, however: The growth you try to remove may not be a skin tag at all.
“I often find in our practice that a patient comes in complaining of a “skin tag” and it is in fact a mole or even a skin cancer” said Gia Edge, an APRN with Riverchase Dermatology. Trying to remove one of these growths at home could worsen the lesion and delay a medical diagnosis.
Even seemingly safer home remedies for skin tags may not work, and they aren’t without risk. “I would strongly advise against home remedies such as tea tree oil or apple cider vinegar because most of the time they will lead to a secondary condition that can cause a rash,” said Edge. Over-the-counter skin tag remover products such as freezing kits and patches can cause scarring, bleeding and damage to the surrounding skin.
Skip the “tie off the skin tag with dental floss” strategy, too. While it’s sometimes effective on smaller skin tags, this approach can take a long time to work, and it’s not worth the pain and increased risk of infection. Also, you don’t want to find out what a decaying skin tag smells like (hint: it’s not pleasant).
Removing skin tags: How dermatologists do it
Professional skin tag removal is a safer, quicker and nearly painless process. Plus, your dermatologist can confirm that your growths are in fact skin tags and not warts, moles, seborrheic keratosis, molluscum contagiosum or skin cancer.
Depending on the size and location of the skin tags, your dermatology provider may use one of the following skin tag removal techniques.
Excision
If your skin tags are small, the dermatologist may snip them off with surgical scissors or, for larger skin tags, shave them off. They may inject a numbing medication into the area first.
Cryosurgery with liquid nitrogen
Liquid nitrogen, a very cold gas, is applied to the skin tag or its stalk to freeze it, which destroys the tissue. The procedure tends to cause a brief stinging or burning sensation. You can expect the skin tag to fall off in about 10 to 14 days. Cryosurgery is often used for thicker skin tags.
Electrocauterization
Some dermatologists use electrocauterization for thicker skin tags and skin tags in delicate areas such as the eyelids. In this procedure, a pen-like device delivers a heated electrical current to burn off the skin tag. You’ll develop a scab, which disappears in one to three weeks.
After any of these procedures, you’ll need to keep the treated area clean, and you may be advised to cover it with a bandage for a few days to prevent friction. Applying petroleum jelly while the skin heals can help prevent or reduce scarring. Using sunscreen is a must.
If a beloved necklace triggered the growth of skin tags on your neck, consider putting it away or at least removing it in the evening so the skin tags are less likely to return.
Medically reviewed by Gia Edge, APRN
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
7 Psoriasis Self-Care Tips to Soften Psoriasis Plaques
If you have plaque psoriasis, the best treatment is the plan your dermatologist recommends, which may include topical medicines, oral medicines and even light or laser therapy. The dermatologist can finetune the plan based on what’s working and address concerns such as worsening plaques or signs of psoriatic arthritis. But there’s plenty of psoriasis self-care strategies you can follow to help minimize scaly skin patches, calm the irksome psoriasis itch and fend off psoriasis flare-ups.
Below are seven dermatologist-approved tips to help you manage psoriasis at home.
1. Reboot your showers and baths
Long, hot showers and baths can be your skin’s worst enemy. They rob it of moisture and leave it more vulnerable to flare-ups. Try this routine instead:
- Turn the tap to warm (not hot).
- Use an unscented, non-soap cleanser or body wash. Steer clear of deodorant soaps, which tend to be too harsh.
- Lather up with your hands, not a washcloth or loofah. Any kind of manual exfoliation can make psoriasis worse.
- Limit showers to five minutes and baths to 15 minutes.
- Rinse off thoroughly and blot your skin gently with a clean towel until you are damp, not dry.
- Immediately apply a thick cream or an ointment to seal in moisture. Some moisturizers, such as Curél Hydra Therapy Wet Skin Moisturizer, are designed to be used on wet skin.
2. Use a psoriasis cream regularly
Moisturizing often to skin hydrated is an essential psoriasis self-care strategy. A thick, fragrance-free cream is the best psoriasis moisturizer. But you may want more than a simple moisturizer. Psoriasis creams go a step further: They contain one or more moisturizers as well as ingredients designed to smooth the skin and reduce flaking, redness and scaling.
Many of the best creams for psoriasis contain salicylic acid, a beta-hydroxy acid that exfoliates the dead skin cells that form psoriasis plaques. Salicylic acid also calms inflammation and itching and makes it easier for topical medications to penetrate the skin.
Choose a product that’s unscented or fragrance free, since added fragrance can irritate the skin and trigger flares. Products labeled “gentle” or “for sensitive skin” are free of chemicals and dyes that might make psoriasis worse.
The National Psoriasis Foundation maintains a list of recommended psoriasis self-care products, including psoriasis creams. Check their product directory, or look for the National Psoriasis Foundation Seal of Recognition when you shop. Among the creams they recommend are:
- CeraVe Psoriasis Moisturizing Cream
- Dermarest Psoriasis Medicated Treatment Gel
- Gold Bond Psoriasis Relief Multi-Symptom Cream
- MG217 Medicated Moisturizing Psoriasis Cream
Keep in mind that creams and ointments (including petroleum jelly) tend to be thicker than lotions and better at locking in moisture. That said, they may also be greasier. You may want to use a cream or ointment at night and after your shower and a lotion when you don’t have time to let a cream sink in.
3. Stop yourself from picking or scratching
As tempting as it may be to pick at scaly skin patches, peeling off flakes before they fall off naturally can make psoriasis worse. Damaging the healthy skin next to psoriasis plaques, even slightly, can inflame it and cause new scales to form. Even absentmindedly scratching can damage the skin, so keep your fingernails short.
If the plaques itch, keeping them moisturized should help. Applying a cold compress can also ease a bout of itching. A washcloth soaked in cold water will do the trick.
4. Switch laundry detergents
If you aren’t already using a laundry detergent that’s free of fragrance, dyes and chlorine and designed for sensitive skin, try switching to one.
5. Hydrate your home
Dry air is thirsty air: It will sap moisture from wherever it can, including your skin. Add moisture to the air by running a humidifier in the room you spend most of your time in, especially in the winter, when home heating systems leave air especially dry. If you can afford to splurge on a higher-end product, consider buying a humidifier that’s also an air purifier.
6. Explore natural remedies for psoriasis
Your kitchen cabinet or pantry may contain a home remedy or two that could be effective for you. Among the natural remedies for psoriasis that show promise are these.
Turmeric
Psoriasis is driven by inflammation, and the active ingredient in this colorful spice, called curcumin, has been shown to ease inflammation when applied to skin as part of a topical psoriasis treatment. Consult your dermatologist if you’re interested in trying it. Turmeric supplements have also been found to tamp down inflammation. Talk to a registered dietitian about a dose that’s appropriate for you.
Epsom salts
Using Epsom salts or salts from the Dead Sea as a bath soak has been found to help ease inflammation and itching from psoriasis. This may be due in part to the anti-inflammatory effects of the salt’s magnesium. (Regular table salt has no magnesium.) To find out if a salty soak helps your psoriasis, run a tub of warm water, add the amount of Epsom salts or Dead Sea salts recommended on the package or by your dermatologist (likely around 2 cups per gallon of water) and soak for no more than 15 minutes.
Colloidal oatmeal
Oats ground to a fine powder also make for a soothing soak. You can buy a colloidal oatmeal bath soak or make your own by grinding regular oats in a food processor, coffee grinder or spice grinder. Follow the directions on the package or ask your dermatologist how much homemade colloidal oats to use.
7. Address stress
Stress and anxiety can make psoriasis worse. In fact, a review of multiple studies found that 31% to 88% of people with psoriasis said stress triggered flares.
If your psoriasis flares when you’re under pressure or feeling down, prioritize daily physical and mental breaks.
- Start a yoga, meditation, deep breathing or journaling practice.
- Get outside to walk, bike ride or enjoy a dose of fresh air and sunshine. Talk to your dermatologist about how much unprotected sun exposure, if any, is right for you. Small doses of sunlight may help some people with psoriasis, but if you’re taking a medication that makes your skin more sensitive to the sun, it’s a bad idea.
- Take up a relaxing hobby, whether it’s gardening, knitting, drawing or playing an instrument.
If you need help managing stress and anxiety, consider therapy or counseling. As with many chronic conditions, it sometimes takes a village of experts to tame psoriasis, and adding a mental health practitioner to your psoriasis care team could be a game changer.
Medically reviewed by Lucy L. Chen, MD
Written by Maura Rhodes, a writer and editor specializing in health and well-being.
A Guide to UV Rays and the UV Index
You can’t see UV rays, but you can easily see how they can affect the skin—sunburns, age spots, wrinkles and, worst-case scenario, cancerous lesions after years of exposure.
Using a broad-spectrum sunscreen daily is key to preventing short-term and long-term skin damage caused by UV radiation. But knowledge is another good weapon against UV rays. Understanding the different types of UV rays, which UV rays cause cancer, and how to use the UV index to plan outdoor activities can help you preserve healthier, younger-looking skin.
What are UV rays?
UV radiation is electromagnetic radiation from the sun that has a shorter wavelength than visible light does, so it isn’t apparent to the eye. It’s grouped into three wavelength bands: UVA rays, UVB rays and UVC rays.
What are UVA rays?
Most of the radiation that reaches the earth is UVA radiation. It has the longest wavelength of the three types of UV rays and is not absorbed by the ozone layer that surrounds and shields the planet. This makes UVA rays especially dangerous for the skin. In addition to piercing through the ozone layer, these rays can penetrate the middle layer of skin (the dermis).
What are UVB rays?
Most UVB radiation is absorbed by the ozone layer, though some does manage to get through to the earth. It has a shorter wavelength than UVA radiation and affects only the outer layer of skin (the epidermis).
What are UVC rays?
UVC radiation emitted by the sun is absorbed by the ozone layer and doesn’t affect the skin. However, there are artificial sources of UVC radiation that can damage skin, including sun lamps and lasers.
Health effects of UV radiation: UVA vs. UVB rays
Because they reach different layers of skin, UVA and UVB rays are linked to different types of sun damage. UVA rays are largely responsible for signs of aging, such as wrinkles and age spots (think “a” for “aging”), while UVB rays cause sunburn (think “b” for “burning”).
Which UV rays cause cancer?
UVA and UVB rays both damage the DNA of skin cells and increase the risk of the most common skin cancers— basal cell carcinoma, squamous cell carcinoma and melanoma. The risk of melanoma, the most lethal of the trio, increases dramatically when skin gets burned badly or repeatedly.
Are UV rays bad for your eyes?
Too much exposure to UVA rays can damage the eyes, including the retina, the light-sensing layer in the back of the eye. Damage can lead to vision changes, age-related macular degeneration and cataracts. UV rays can also contribute to basal cell or squamous cell carcinoma on eyelids.
Do clouds block UV rays?
Clouds do block some UV rays, but you still need sunblock on a cloudy day. Up to 80% of UV radiation can pierce through a layer of light clouds according to the Environmental Protection Agency (EPA). Because clouds can scatter incoming radiation, they may actually intensify the effects of UV rays in some cases.
UV rays and vitamin D
UVB rays are the most important source of vitamin D. Your bones need vitamin D because it helps the body absorb bone-strengthening calcium and phosphorous from food.
The World Health Organization recommends getting five to 15 minutes of sun exposure two to three times a week, though at some latitudes, it’s all but impossible to get enough vitamin D from the sun except in summer. Vitamin D supplements and fortified foods and beverages can supply the rest.
What is the UV index?
The UV index is a forecast that describes the risk of overexposure to UV rays on a given day in a given area. It’s calculated by the National Weather Service based on how much UV radiation is expected to make it through to the earth’s surface. The UV Index scales goes from one to 11. The higher the number, the greater the risk.
To check the UV rays today, download the EPA’s free app, called the UV Sunwise Index, or search by ZIP code on the EPA’s website. The best way to use the UV index is to get into the habit of checking it each day, just as you do the weather forecast.
Protecting yourself from UV radiation
Sunscreen and commonsense measures can help protect you from the damage caused by too much exposure to UVA and UVB rays. You probably know the drill:
- Use a broad-spectrum sunscreen with an SPF of 30 or more. “Broad spectrum” means the sunscreen protects against both UVA and UVB rays. Reapply every two hours or after you swim or sweat.
- Cover up. Don’t make sunscreen do all the work. Cover as much skin as possible with clothing and wear a wide-brimmed hat.
- Wear UV-blocking sunglasses. Choose ones with large frames.
- Seek shade. The sun’s rays are strongest between 10 a.m. and 4 p.m., even when it’s cloudy. When possible, stay in the shade during that window of time.
Medically reviewed by Ashley E. Falzone, MD
Written by Maura Rhodes, a writer and editor specializing in health and well-being.
Men, Healthy Tans and Melanoma Prevention
The gender divide is real. Case in point: Men are less likely to wear sunscreen than women and more likely to believe in the concept of healthy tans. Chances are, they're also less concerned about melanoma prevention. Yet according to the Skin Cancer Foundation, melanoma hits males harder than females.
Consider these eye-opening statistics about skin cancer in men:
- Starting at age 50, men are more likely than women to develop melanoma.
- Melanoma accounts for 6% of cases of new skin cancer in men compared to 4% in women.
- Melanoma survival rates are considerably lower for men. For example, males between ages 15 and 39 are 55% more likely to die of melanoma than females.
It may not have to be this way. If you’re a guy (or someone who loves a guy), knowing the facts about skin cancer in men and melanoma prevention could prove lifesaving.
Melanoma in men: Why the risk is different
Biological differences between the sexes make men’s skin more vulnerable to sun damage. But common attitudes and popular misconceptions are also to blame. Here’s a look at some reasons men are more likely to die of melanoma than women.
Men's biology is different
Some research suggests that men have at least a couple of biological factors working against them when it comes to melanoma.
- Skin structure. Men tend to have thicker skin than women, with more collagen to support its structure and less fat. According to the American Academy of Dermatology, these differences can make men more vulnerable to sun damage. Compounding the problem, there’s some evidence that men’s skin doesn’t heal as well from sun damage.
- Hormones. A small study found that estrogen (the “female hormone”) may strengthen the immune system’s response to melanoma and help make treatment more effective. Other research suggests that testosterone (the “male hormone”) is linked to an increased risk of skin cancer.
Guys believe in healthy tans and lack skin cancer smarts
According to a survey from the American Academy of Dermatology, more men than women believe in healthy tans and think a “base tan” offers protection from harmful ultraviolet rays.
The truth is, even a carefully nurtured “base” tan provides little protection from sunburn — an SPF of only around 3 or 4, experts say. And any amount of frequent, unprotected exposure to UV rays from the sun or a tanning bed causes skin damage that can eventually turn into cancer. Even people who don’t burn are at risk for skin cancer, which means no tans are healthy tans. (People who do burn should know that getting five or more sunburns over the course of a lifetime doubles the risk of melanoma.)
Men are also less likely to know that skin cancer can develop in areas that don’t often see the sun, so they may not look for suspicious skin changes in places like their armpits or between their toes.
Men say no to sunblock and health screenings
Many women are in the habit of using a plethora of skin care products, from face cleansers to moisturizers to anti-aging serums, but a lot of men rarely use anything on their skin — including sunscreen. It’s probably no coincidence that sunscreen advertising rarely targets men. When is the last time you saw an ad for men's sunscreen?
Guys are also notoriously doctor shy. They’re less likely than women to see a physician, including to have regular skin cancer screenings or get a suspicious mole checked out. This means that early signs of skin cancer, such as a change in the shape or color of a mole, may go unevaluated.
Melanoma prevention tips for men
Men can follow the same skin-protection playbook women do and greatly improve their odds of avoiding skin cancer, including melanoma.
Use sunscreen every day, rain or shine
Wearing sunscreen with an SPF of 15 every day can lower the risk of skin cancer by as much as 50%, but dermatologists recommend an SPF of 30 or more. Reapply every couple of hours and after you get wet or sweaty.
Wear sun-protective clothing
When you’d normally go shirtless, spare your skin by wearing a sunscreen shirt or a rash guard (tight-fitting top made of synthetic fabric and designed to protect the skin from surfboards and boogie boards). More and more companies are making sun-protective clothing for men. According to the Skin Cancer Foundation, sun-protective clothing with an ultraviolet protection factor (UPF) of 50 blocks 98% of UVA and UVB rays.
Keep an eye out for skin changes
The American Cancer Society advises doing a skin self-exam once a month, ideally after a shower or bath. Check everywhere, including your scalp, armpits, genitals, between your toes and under your toenails. Look for symptoms of melanoma such as new growths, moles that change appearance or look different from other moles, and sores that bleed or scab over but don’t heal. Use a mirror to check your back and other hard-to-see areas. Better yet, if you have a partner, ask them to scan your skin.
Get regular screenings
The Skin Cancer Foundation advises yearly skin checks for people at average skin cancer risk. If you’ve had skin cancer in the past, your dermatologist may recommend more frequent screenings.
Medically reviewed by Todd Williams, MSN, DCNP
Written by Maura Rhodes, a health writer and editor based in Montclair, New Jersey.
Eczema vs. Psoriasis: What’s the Difference?
Most people get the occasional bout of dry, itchy skin, and it’s often nothing a good moisturizer can’t fix. But if patches of dry, red, inflamed skin keep coming and going, a chronic skin condition such as eczema or psoriasis may be to blame. How can you tell if it's eczema vs. psoriasis? Surely there are dead giveaways that it’s one or the other?
Not necessarily.
“While there are some clues that can help set them apart, the difference between eczema and psoriasis is more subtle than many people realize,” said Robert Snyder, MD, a board-certified dermatologist and internist at Riverchase Dermatology.
Not even the severity of symptoms can tell you which condition you have. “It’s a common assumption that psoriasis symptoms are much worse than eczema symptoms, but both conditions can range from mild to severe,” Dr. Snyder added.
To add to the confusion, it’s possible to have eczema and psoriasis at the same time, though that’s uncommon (phew). Read on to learn more about these conditions and the symptoms of eczema vs psoriasis.
What is eczema?
Eczema is an inflammatory skin condition in which the immune system overreacts to certain triggers, including irritants and allergens. Itching leads to scratching and then an eczema rash. Common eczema triggers include skincare products, detergents, fragrances, hot or cold weather and stress. The exact cause of eczema is unknown, but it’s thought to be a combination of environmental factors and genetics.
What is psoriasis?
Like eczema, psoriasis is driven by inflammation, and the symptoms can be worsened by triggers such as allergens and certain weather conditions. But unlike eczema, psoriasis is an autoimmune disease. In these diseases, the immune system mistakenly attacks healthy tissue. If you have psoriasis, your immune system is constantly in overdrive. This causes new skin cells to grow up to 10 times faster than usual and pile on top of the skin instead of shedding. The result is raised patches. What causes psoriasis isn’t well understood, but as with eczema, genetic and environmental factors are probably involved.
What does eczema look like?
There are several types of eczema. The most common one, atopic dermatitis, involves dry, cracked skin that itches. Scratching causes a rash that’s red in people with lighter skin and may be brown or purple in people with darker skin. You may notice scaly patches or see small, rough bumps that ooze a clear or straw-colored fluid and eventually crust over. Over time, you may develop thick, leathery patches of skin.
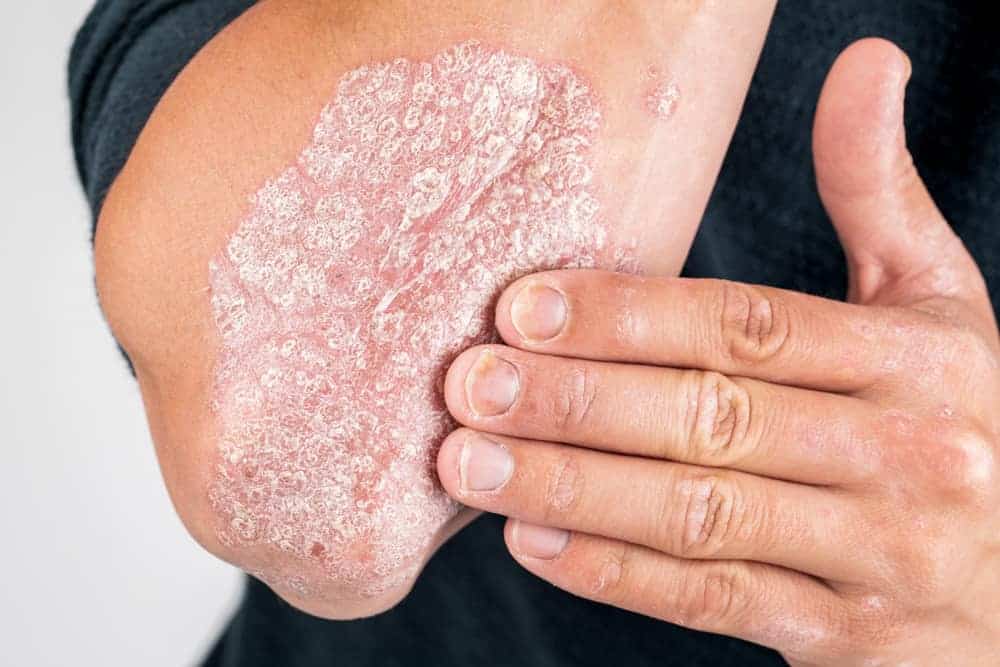
What does psoriasis look like?
The most common type of psoriasis, plaque psoriasis, causes thick, raised patches called plaques. Psoriatic plaques can look a bit like an eczema rash and are similar in color, but they are typically covered in distinctive silvery-white scales or, in dark skin, gray scales. It’s harder to tell the conditions apart if you have early psoriasis, since the only symptoms of early psoriasis tend to be an inflamed, raised patch of skin and itching.
The difference between psoriasis and eczema: potential clues
Eczema is between three and four times more common in the United States than psoriasis, but psoriasis affects more than 8 million people nationwide, so don’t discount it as a possibility. Here are some clues that help distinguish psoriasis vs eczema.
- Oozing. Unlike an eczema rash, psoriatic plaques don’t ooze. “Oozing is probably the closest thing to a telltale sign that a patient has eczema and not psoriasis,” said Dr. Snyder.
- Level of itching. Itching is the most common symptom of eczema, and at times, it can be intense. Psoriasis also causes itching, but it’s usually milder.
- Level of pain. Eczema usually doesn’t hurt, though it can sting or burn, especially if you scratch hard enough to break the skin. Psoriasis is more likely to be painful, causing stabbing, throbbing or aching sensations.
- Skin thickness. Psoriatic plaques are usually thicker than the leathery patches of skin sometimes seen in eczema.
- Age symptoms first appear. Both conditions can emerge at any age, but eczema most commonly develops in babies and children and sometimes persists into adulthood. Psoriasis is likely to first appear between ages 15 and 35.
- Affected areas. Eczema and psoriasis can appear on any part of the body, but eczema is most likely to show up on the hands, face, back of the neck, back of the knees and crooks of the elbow. Psoriasis often appears on the knees and elbows as well (on the front of the knee and outer elbows, however) and also the scalp and lower back.
- The edges of the dry patches. Psoriasis plaques have sharply defined edges, while the edges of eczema patches are less distinct.
- Nail symptoms. Eczema and psoriasis can affect the fingernails and toenails. Both conditions can cause pitting (pinprick holes) in the nails, but people with nail psoriasis may also notice white discoloration and lifting of the nails from the nail bed.
If you suspect you have eczema or psoriasis, see a dermatologist. Left untreated, both conditions can decrease your quality of life and even contribute to depression.
“Psoriasis in particular should be treated right away,” said Dr. Snyder. “If you have it, you’re at greater risk for psoriatic arthritis as well as cardiovascular disease, type 2 diabetes and high blood pressure."
Your dermatologist can provide an accurate diagnosis and develop a treatment plan that’s right for you.
Schedule an appointment today if you have symptoms of eczema or psoriasis.
Medically reviewed by Robert A. Snyder, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.