Baby Acne: What Parents Need to Know
Acne is the bane of teenage life, but babies can get it, too, which often comes as a surprise to parents. Many newborns have baby acne (also called newborn acne or neonatal acne). Less often, babies develop acne as infants (infantile acne).
Baby acne is usually harmless and typically clears up on its own. Still, it’s important to know how to avoid aggravating the baby’s skin and when to bring your baby to a dermatologist to make sure the condition doesn’t require treatment.
What causes baby acne?
In most cases, newborn acne isn’t technically acne at all.
“Very early neonatal acne is more likely an inflammatory reaction to a yeast overgrowth,” said Robin Gehris, MD, a board certified adult and pediatric dermatologist at Riverchase Dermatology.
It may start when hormones passed on from the mother just before she gives birth stimulate the glands that produce sebum, the oily substance that can clog pores.
“Yeast that normally live on the skin, called Malassezia, flourish when sebum production increases in newborns. The yeast, in turn, creates inflammation that results in neonatal acne,” said Dr. Gehris. “The condition is better termed neonatal cephalic pustulosis since the blackheads and whiteheads you see with true acne aren’t present,” she added.
Neonatal cephalic pustulosis (NCP) may appear when babies are about two or three weeks old and typically peaks at four to six weeks.
What causes infant acne?
"Infantile acne is more what we consider to be true acne,” said Dr. Gehris. It’s much less common than newborn acne, occurring in less than 2% of infants. Babies who develop infant acne usually get it when they are several months old.
The causes are unknown, but genetics may play a role. In some babies, the sebum-producing glands are overactive despite normal levels of androgens, the so-called “male” sex hormones. These hormones are a major factor in adult acne.
What does baby acne look like?
Acne can look different in newborns and infants.
Signs of baby acne
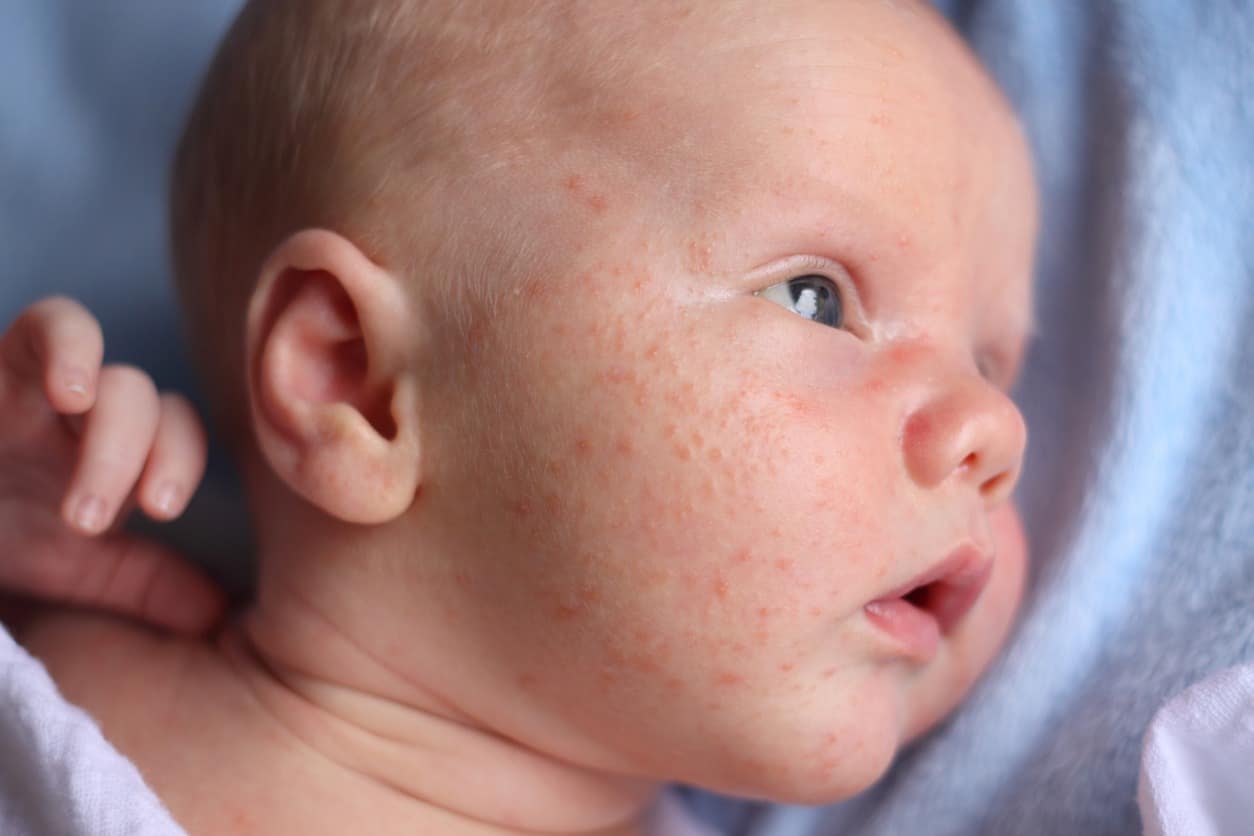
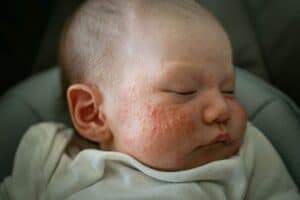
Newborn acne (NCP) can appear as small, greasy, red-pink pimples or red or white pustules (bumps filled with pus) and may include a rough, bumpy rash. Blemishes usually develop on the cheeks, though they can also appear on the nose, eyelids, forehead, chin, scalp, neck and upper torso. NCP does not normally cause blackheads or whiteheads.
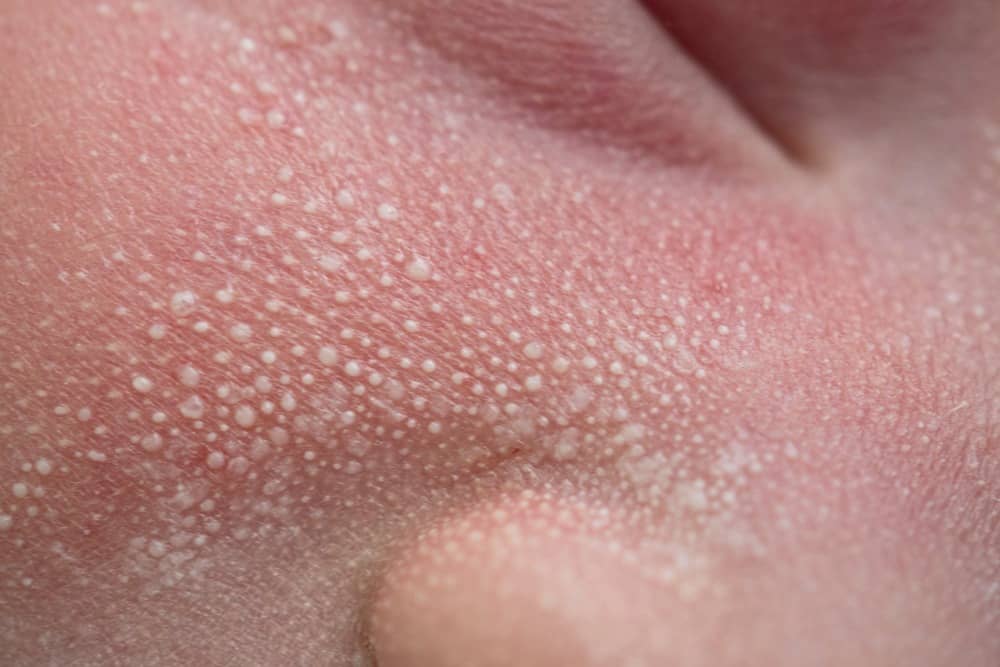
Newborn acne is sometimes confused with baby milia. These small, pearl-like white or yellowish bumps are very common in newborns. One difference between baby acne and milia is the texture: Milia are firmer. They also tend to be tiny (almost the size of a pinhead), and they contain a white plug, whereas newborn acne looks pink, greasy and inflamed.
Infant acne symptoms
Infant acne looks more like adult acne. You might see whiteheads and blackheads in addition to solid bumps (papules or nodules) and pustules. Infant acne usually affects the face but can sometimes appear on the chest and back.
When does baby acne go away?
While newborn acne usually goes away on its own in a matter of weeks or months, infant acne can take six to 12 months or more to clear. In some babies, the acne may cause scars if it isn’t treated.
When should baby acne be treated?
If your newborn has acne, bring the baby to a dermatologist if the condition hasn’t improved after several weeks.
“While NCP can resolve on its own, seeing a pediatric dermatologist can be helpful,” said Dr. Gehris. “We can recommend topical therapy to help it resolve faster. We can also make sure it isn’t true infantile acne, which would also require therapy.”
Infant acne is a different story.
“Infant acne does not always resolve on its own and deserves medical attention from a pediatric dermatologist,” said Dr. Gehris. “Failure to treat it, especially if inflammatory lesions are present, can result in scarring.”
Since infant acne is uncommon, the doctor will want to make sure the symptoms aren’t caused by another issue, such as baby eczema or a skin infection. Rarely, infant acne can be a sign of an endocrine disorder.
Baby acne treatment
If your newborn has NCP, the dermatologist may prescribe a topical anti-yeast cream.
If your baby has true acne and the dermatologist decides it should be treated, they may prescribe a topical acne medicine or, if the acne is severe, an antibiotic.
Never use any acne treatment or acne wash on your baby unless the baby’s dermatologist recommends it. Acne products intended for teens and adults may be too harsh for babies.
How should I care for my baby’s acne at home?
A baby’s skin needs gentle care. To care for a baby with acne:
- Wash the affected area daily. Use plain water, or alternate between plain water and a gentle, unscented cleanser. Don’t scrub. Lightly pat the skin dry with a towel instead of rubbing it dry.
- Don’t use oily or greasy skin care products on areas with acne. These could make the acne worse.
- Refrain from picking at the acne. Picking at or popping pimples can aggravate the acne and lead to infection.
Medically reviewed by Robin Gehris, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Baby Milia: What Are These Little White Bumps on the Skin?
Does your newborn baby have clusters of little white bumps on their face? There’s a good chance they are milia, which are sometimes called milk spots or milk bumps. You may have seen a few of these harmless cysts on your own face at some point, since adults get milia, too. But baby milia, particularly milia in newborns, is even more common. As many as half of all newborns have milia.
In babies, milia often appear on the nose, cheeks, eyelids or scalp, and sometimes on the gums or the roof of the mouth. Less commonly, they form on the upper toro. Read on to learn more about them and how long they last.
What causes milia in newborns?
Milia begin when dead skin cells get trapped in small pockets near the surface of the skin. The protein in those cells, called keratin, hardens into tiny cysts that look like raised white bumps on the skin.
It’s not clear why milia in newborns are so common. Genes may play a role. They are typically present at birth, but in premature babies, they may develop after a few weeks. Either way, they usually aren’t cause for concern.
“Milia are not typically associated with anything abnormal,” said Robin Gehris, MD, a board certified adult and pediatric dermatologist at Riverchase Dermatology.
Baby acne vs. milia
Parents commonly mistake milia on a newborn for baby acne, but milia aren’t whiteheads or any other form of acne. They are smooth, dome shaped and firmer than acne papules (bumps). In babies with light skin, they are typically white or yellowish. In babies with dark skin, they may have a faintly blue cast.
Unlike acne, milia don’t cause swelling, redness or inflammation. The bumps can’t be “popped” like pus-filled acne blemishes can because they don’t have an opening at the top.
Another difference: While newborn acne most often appears when the baby is about two weeks old, milia in full-term babies are usually present at birth or develop within a few days.
How to get rid of milia on a newborn
In most cases, milia will disappear by the time your baby is one month old.
“I see parents who think their baby's milia need to be treated, but most of the time milia resolve on their own,” said Dr. Gehris.
In the meantime, follow these tips:
- Wash your baby’s face every day with warm water. If you want to use a cleanser, choose one that’s mild and unscented. Pat the skin dry; don’t rub.
- Don’t use an exfoliating product intended for adults on your baby, since these products are too harsh for a newborn’s skin.
- Never pick at, squeeze or try to pop the milia. They won’t go away, and you may create scars.
If your baby still has milia after a few weeks or has a large number of milia, see a pediatric dermatologist to rule out other baby skin conditions and discuss treatment.
Medically reviewed by Robin Gehris, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Baby Eczema: What to Know About Causes, Symptoms and Treatment
A baby’s skin is velvety soft and ever so delicate, but as many new parents discover, it’s not always picture perfect. In fact, babies can experience a number of skin conditions, ranging from whitish bumps called milia to baby “acne” to infantile eczema, aka baby eczema. Eczema in babies can be so uncomfortable that it keeps the baby, and the parents, awake at night.
“Eczema can be exceedingly itchy,” said Robin Gehris, MD, a board certified adult and pediatric dermatologist at Riverchase Dermatology. You may catch your baby scratching the dry, itchy patches against their mattress, carpets and objects such as toys to get relief.
“Babies with eczema can easily scratch themselves until they bleed,” said Dr. Gehris. “Scratching is what brings out the rash.” It also creates breaks in the skin that provide easy entry for germs.
Read on to learn the signs and symptoms of eczema (also called atopic dermatitis) and how to treat baby eczema. Even if your child’s eczema is mild, it’s important to address it early to keep your baby comfortable, lower the risk of skin infections and prevent the condition from getting worse. As baby eczema progresses, it becomes harder to treat.
What does baby eczema look like?
Baby eczema causes dry, rough or scaly patches that can appear on any part of the body but often occur on the face, especially the cheeks, and the scalp. When scratching causes a rash, the rash is typically red and easy to see in babies with light skin. In babies with dark skin, it may be pink or a subtle gray-brown to violet-brown.
“In some cases, eczema in babies with dark skin can be easy to miss, which can delay the diagnosis,” said Dr. Gehris.
Blisters that ooze a straw-colored or clear liquid sometimes appear. Once the liquid leaks out, the rash may crust over. The rash site may develop a bacterial or viral infection if left untreated.
Baby eczema symptoms typically appear during the first three to six months of life. They may come and go for no obvious reason.
What causes eczema in babies?
The causes of baby eczema aren’t well understood, but certain genetic factors make some people more susceptible to it. One genetic factor is a mutation in the filaggrin gene. This mutation weakens the skin barrier, the outer layer of skin that locks in moisture and keeps germs out. Other gene mutations cause the immune system to overreact to common substances. If eczema, hay fever or food allergies run in your family, your baby has a higher chance of developing eczema.
Living in a city or a cold, damp climate increases the risk of baby eczema, as does frequent exposure to tobacco smoke and pollution.
Some parents worry that their baby developed eczema because they bottle feed instead of breastfeed, but bottle feeding does not cause eczema. That said, some evidence suggests that breastfeeding may reduce the risk.
Can a food allergy cause eczema?
Many parents have questions about foods that cause eczema in babies, but diet isn’t usually a direct cause of eczema. Babies who have eczema do have a slightly higher risk of food allergies, however.
“Understandably, parents often hope to find a single cause for their baby's eczema so, they’ll perform food elimination trials to see if that helps,” said Dr. Gehris. “The American Academy of Pediatrics does not recommend random dietary elimination, however.”
“I typically advise parents to eliminate a single food only if they notice that their child’s eczema flares after eating it or if the child has had a severe reaction, such as hives or wheezing, to that food. In those cases, it can be helpful to seek the opinion of an allergist.”
Having your child undergo broad food allergy testing to see if they might have food allergies, without evidence that they react to specific foods, is not recommended. Food allergy tests can be subject to false positives, which means they can find a food allergy that isn’t there. You could end up cutting out a good-for-you food that is fine for your child to eat.
Baby eczema treatment
There’s no single, one-time cure for eczema, but there are plenty of ways to reduce flares, protect against infections and make the baby more comfortable.
Trigger avoidance
A host of irritants and allergens can cause an eczema flare. These include:
- Dry air
- Tobacco smoke
- Pet dander, dust, pollen, foods and other allergens if your baby is allergic
- Fragrances in soap, laundry detergent and fabric softener
- Baby powder
- Baby wipes
- Wool and other scratchy fabrics
- Heat and sweat
- Saliva (from drooling)
Baby eczema creams
Baby eczema creams, lotions and ointments help ease symptoms and soothe and protect the skin. Creams and ointments are thicker and may be more effective than lotions, but don’t use an ointment if the rash is weeping. Avoid moisturizers that contain fragrance.
Good choices include:
- CeraVe or CeraVe Baby Moisturizing Cream
- Cetaphil Moisturizing Cream
- Aquaphor Baby Healing Ointment
- Aveeno Baby Eczema Therapy Moisturizing Cream
- Eucerin Baby Eczema Relief Body Creme
- Petroleum jelly (such as Vaseline)
Apply a moisturizer two or three times a day.
If your baby’s drool causes eczema on their chin or around their mouth, try coating those areas with petroleum jelly to act as a barrier between the saliva and the skin.
Short, lukewarm baths
A short, lukewarm (not hot) bath can be soothing to baby’s skin. Keep baths to just 5 or 10 minutes, or 15 to 20 minutes if longer baths don’t make your baby’s eczema worse. Choose a fragrance-free cleanser instead of soap, and don’t apply it directly to areas with a rash. After the bath, gently pat your baby dry with a towel, leaving the skin slightly damp. If you are using a corticosteroid cream, apply it now. Then apply moisturizer to seal in the moisture.
Topical corticosteroids
If your baby’s eczema is mild, an over-the-counter corticosteroid lotion, cream, ointment or spray can help calm the inflammation and itching. Talk to your pediatric dermatologist before using one. The doctor can recommend the best product for your baby and tell you how to use it. Infants are more sensitive to corticosteroids than adults, so it’s important to follow directions closely to avoid side effects.
If your baby has moderate to severe eczema, your doctor may recommend a prescription steroid ointment.
Dilute bleach baths
If your baby’s eczema is hard to control, your doctor may recommend very dilute bleach baths to kill bacteria on the skin. Do not try this treatment on your own, since adding too much bleach to the bath water can make symptoms worse. Follow your doctor’s instructions carefully. Never apply bleach directly to a baby’s skin.
Dupilumab (Dupixent)
Dupixent, an injectable biologic medicine, was recently approved for treating moderate to severe eczema in children as young as 6 months old. Your baby’s doctor might prescribe it if topical prescription treatments haven’t improved the symptoms or they aren’t recommended for your baby. Injections are given every four weeks, either by the doctor or by you.
“Dupixent is much safer and more effective than older treatments such as oral steroids,” said Dr. Gehris. “Oral steroids are not recommended for treating childhood eczema as they suppress the entire immune system and stunt growth.”
Does baby eczema go away?
In many cases, children can gradually outgrow their eczema. Only half of babies who develop eczema when they’re less than a year old still have it three years later. While most children no longer have eczema by the time they turn 5, it may return later in life.
Medically reviewed by Robin Gehris, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
What’s the Best Ointment or Cream for Insect Bites?
Are you the person mosquitos single out to dine on? Whether you’ve been eaten alive by these tiny, buzzing drones or bitten up by flies, fleas or other insects, your local drugstore — not to mention the internet — has products that can ease the itch and/or soothe the pain, and it’s smart to keep one in your medicine cabinet and travel bag. But what’s the best ointment or cream for insect bites?
That depends in part on your symptoms (do you have pain or just itching?) and your personal preferences (do you prefer a gel, love the idea of a handy applicator or favor plant-based ingredients?). The most important consideration, of course, is the active ingredients.
Ingredients to look for
Several ingredients can effectively tackle itching and inflammation, which are caused by the body’s response to the saliva of the critter that bit you.
“Itching and swelling develop because the body interprets the saliva as a foreign substance and attacks it,” said Jennifer Wong, D.O., a board-certified dermatologist at Riverchase Dermatology.
It begins its assault by releasing histamine, the same chemical that’s released when you have an allergy attack. Histamine creates inflammation at the site of the bite, which tells immune cells to flock to the area. Many insect bite treatments contain hydrocortisone to tamp down the inflammation, which also calms the itching.
Others contain ingredients such as lidocaine that numb the skin, which can lessen both itching and pain. “Bonus” ingredients in some products moisturize and soothe.
Prefer a plant-based option? Natural insect bite treatments contain a variety of ingredients that cool or soothe the skin. Some natural ingredients, such as camphor, are known to reduce inflammation and pain.
“Just keep in mind that natural ingredients may not be as effective at reducing swelling or numbing the skin as hydrocortisone or lidocaine, and you may have to apply the product more often,” said Dr. Wong.
What to put on insect bites: 5 dermatologist-approved choices
For mosquito bite relief or relief from pain and itching caused by other insect bites, here are five top picks according to Dr. Wong.
Benadryl Itch Stopping Gel Extra Strength
This gel contains 2% diphenhydramine hydrochloride, an antihistamine that effectively knocks out the itching and swelling according to many users. Other ingredients include glycerin, which soothes the skin, and camphor, which helps relieve pain and itching. Camphor was traditionally made from the bark and wood of the camphor tree, but the camphor used in most products today comes from turpentine.
Gold Bond Medicated Pain & Itch Relief Cream with Lidocaine
This remedy uses the maximum amount of lidocaine allowed in over-the counter products to numb the itch away. The anesthetic power of lidocaine makes this cream handy for easing the pain of scrapes and sunburns, too. Aloe leaf juice is a “bonus” ingredient that soothes the skin and reduces inflammation. Aloe fights bacteria, too, so it may help prevent the bite from becoming infected if you scratch it too fervently.
Aquaphor Itch Relief Ointment Maximum Strength
Hydrocortisone (1%, the maximum strength allowed) is the main ingredient in this hypoallergenic ointment, which boasts long-lasting relief — up to 12 hours, per the manufacturer. Additional soothing ingredients include petrolatum, mineral oil and glycerin. Keep a tube on hand for soothing skin rashes and eczema, too. Remember, ointments are a bit greasier than creams, but they’re more effective at sealing in moisture.
Cortizone-10 Maximum Strength 1% Hydrocortisone Anti-Itch Liquid with Easy Relief Applicator
A great non-messy, on-the-go option, this liquid bug bite treatment is packaged in a lip balm-like tube with a spongy tip. To apply, just press on the bite with the tip of the tube. In addition to hydrocortisone, it contains other calming ingredients such as aloe leaf juice and avena sativa (oat) kernel extract. Stash these tubes in your pocket, purse and glove compartment.
Murphy’s Naturals Insect Bite Relief Soothing Balm
Fans of natural products will appreciate this pleasant-smelling balm, which is packed with soothing ingredients including glycerin and a variety of essential oils (andiroba, eucalyptus, tea tree and chamomile). Bonus: The balm comes in a travel-friendly tin that can be reused or recycled.
When to see a dermatologist
If over-the-counter insect bite treatments don’t help enough, your dermatologist can prescribe a stronger topical medicine to relieve the itch, inflammation and swelling.
Most insect bites are nothing more than a nuisance, but some bites can lead to complications if you’re allergic to the venom, you were bitten by a large number of insects or the bites remain for a long period of time. In addition, some insect bites can cause systemic complications. Make an appointment with a dermatologist right away if you develop a rash, headache, fever, body aches or constant tiredness.
In some cases, a reaction may be so severe that it requires emergency treatment. Call 911 or go to the ER immediately if you develop difficulty breathing, chest pain, dizziness, vomiting or swelling of the lips, face or tongue.
Medically reviewed by Jennifer Wong, DO
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Does Sunscreen Prevent Tanning?
For some people, the desire for that tawny glow from a tan can be hard to resist, even if they know the risks of tanning. But does sunscreen prevent tanning altogether, or can you tan with sunscreen? And can you wear sunscreen for UV protection and still get a “healthy” tan?
“Sunscreen is effective at preventing tans in most cases, but only if you use it properly,” said Annie Gonzalez, MD, a board-certified dermatologist at Riverchase Dermatology. “If you do get a tan, it means your skin has suffered skin damage. There is no such thing as a healthy tan. The UV rays that contribute to wrinkles and skin cancer are also what cause the skin to tan.”
What is a tan, really?
Many people associate tanned skin with attractiveness and good health, but here’s what happens when you spend time in the sun without wearing protective clothing or sunscreen. First, the UV rays damage the outer layer of skin. To try to protect itself from further damage, the skin produces more melanin, the pigment that gives skin its color. The extra melanin is what creates a tan.
Meanwhile, the UVA radiation that causes tans speeds skin aging — think wrinkles, dark spots and a leathery texture. Both UVA radiation and UVB radiation, which is the main cause of sunburn, increase the risk of developing skin cancer, in part by damaging the DNA in skin cells.
Is there a safe way to tan?
The bottom line: No tan is safe. This includes a base tan, which may make you burn a little slower but still creates skin damage, as well as tans from a tanning bed, which are no safer than outdoor tans.
If you’re tanning to look better, remember this: “The more often you tan, the greater the damage to the collagen and elastin that keeps skin looking supple and youthful,” said Dr. Gonzalez.
How to avoid an accidental tan
If you’re not trying to get tan but you do anyway, it’s probably a sign you’re spending too much time in the sun during peak hours and not using sun protection, including sunscreen, correctly. Sunscreen mistakes include:
- Applying too little sunscreen. To cover the exposed areas of your body, you should use at least an ounce of sunscreen, enough to fill a shot glass (or two tablespoons). Most people use about 25% to 50% of that amount.
- Forgetting to re-apply. Protection from one application of sunscreen doesn’t last all day. Reapply every two hours when you’re outside or immediately after you swim or sweat.
- Using old sunscreen. Sunscreen degrades over time. If your sunscreen is expired or you can’t remember how long you’ve had it, throw it out. To help prevent degradation, keep it out of direct sunlight, and don’t leave it in your hot car.
- Choosing a low-SPF sunscreen. For the most effective protection, choose a sunscreen with an SPF of 30 or greater, and make sure the label includes the words “broad spectrum,” which means it protects against both UVA and UVB rays.
Get glowing with a self-tanner
If you like how you look with a tan, get it from a bottle instead of the sun. The better self-tanners have come a long way since the early versions that turned people orange.
Finding the best self-tanner can take some trial and error. Some have an off-putting smell, and yes, some still manage to make you look more orange than tan. If you aren’t sure where to start, try one of these high-rated picks.
Drugstore options:
- Jergens Natural Glow Daily Moisturizer
- L’Oréal Sublime Bronze Self-Tanning Water Mousse
- Alba Botanica Sunless Tanner
Higher-end options:
- Coola Sunless Tan Firming Lotion
- Tan-Luxe The Water Hydrating Self-Tan Water
- Isle of Paradise Self-Tanning Water
For a convincing sun-kissed look, follow the instructions carefully. Exfoliate and moisturize your skin in advance to avoid unevenness, which screams “fake tan.” When you’re ready to apply the self-tanner, make sure your skin is dry (no moisturizer). That said, you might want to smooth a little moisturizer into areas that are prone to developing self-tanner stains, including the elbows, knees and heels.
Medically reviewed by Annie Gonzalez, MD.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Sunburn Peeling: What It Means and What to Do About It
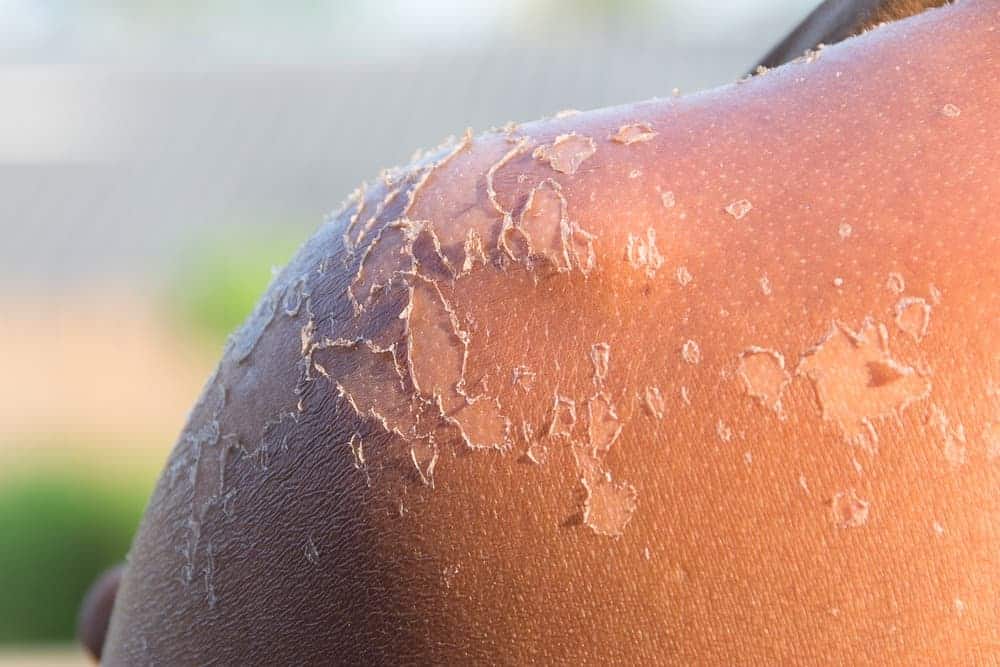
You got scorched by the sun, and now that the sunburn has faded, you’re facing the less-than-attractive after effects: peeling skin. If you’re wondering how to get rid of peeling skin from a sunburn, the answer is simple: don’t.
“Pulling off the dead skin is counterproductive, as is any form of exfoliation,” said Stacy Chimento, MD, a board-certified dermatologist at Riverchase Dermatology.
Granted, leaving it alone may be easier said than done. For certain folks, peeling off skin after a sunburn is deeply satisfying in ways that are hard to explain. For others, it’s more of a mindless habit, like biting your nails or cracking your knuckles. Some people rip off the dead skin just to be rid of it or because they think they’re doing their skin a favor.
The temptation increases when dried-out edges rise up like so many pull tabs, all but inviting you to grab and yank. But understanding what you’re really doing when you peel sunburned skin might help you stop.
Why does skin peel after a sunburn?
If your skin is peeling from a sunburn, it means your body is ridding itself of cells that have been critically damaged by UV rays. The damage may include DNA mutations that could eventually lead to skin cancer.
What happens when you peel sunburned skin?
Before they fall off on their own, the dead skin cells serve a purpose: protecting the damaged but still-living skin underneath.
“When you pull off or otherwise exfoliate dead skin before it’s ready to come off, you expose the very tender skin beneath it, which is still healing,” said Dr. Chimento. That can prolong the healing process. Because the unhealed skin is less able to fight off bacteria, it can even lead to an infection.
It’s best to let the dead skin shed naturally to allow new, healthy skin to form.
How to treat peeling skin from a sunburn
Now that you know the number one rule of dealing with peeling skin (leave it alone), what should you do while you wait for the dead cells to make their exit? Moisturize, moisturize, moisturize.
Slathering on moisturizer not only keeps the skin hydrated, it also helps restore the skin barrier, the top layer of skin under those dead cells. It may also help curb additional peeling. Another bonus: Emollients such as petrolatum, lanolin, mineral oil, glyceryl stearate and dimethicone, found in some moisturizers, soften the dead skin, making those “pop tops” less alluring. Ingredients such as soy and ceramides may help your skin heal faster.
Don’t apply petroleum jelly or an oil-based cream when your sunburn is fresh. These can trap the heat, prolonging the pain.
What is the best lotion for peeling skin after a sunburn?
The best lotion for peeling skin after a sunburn isn’t a lotion. Lotions contain a lot of water, so the skin dries out again quickly after you apply it. Instead of a lotion, use a thick cream or an ointment to seal in moisture. Choose a fragrance-free product to avoid skin irritation.
Creams Dr. Chimento recommends include:
- Cetaphil Soothing Gel Cream with Aloe
- Vanicream Moisturizing Cream
- Aveeno Restorative Skin Therapy Oat Repairing Cream
- Aquaphor Healing Ointment
Whatever product you apply, apply it gently — don’t try to sneak in some exfoliation through vigorous rubbing.
While you’re waiting for your skin to repair itself, keep it under wraps if you must go out in the sun.
How to prevent a sunburn from peeling
There’s no way to prevent a sunburn from peeling if the skin cells are damaged enough that they need to come off. That said, you might peel less if you limit the inflammation caused by the burn right after it happens. How?
“I’m a big fan of using anti-inflammatories after a severe burn,” said Dr. Chimento. “You can apply an over-the-counter hydrocortisone cream for up to a week to soothe the skin. You can also take aspirin, ibuprofen or naproxen for pain relief.” For a soothing hydrocortisone cream, Dr. Chimento likes Aveeno 1% Hydrocortisone Anti-Itch Cream.
Aloe vera gel is another good choice. Dr. Chimento’s pick: Sun Bum After Sun Cool Down Gel.
You can avoid peeling skin from a sunburn in the future by — you guessed it — avoiding the sunburn. Choose a sunscreen with an SPF of at least 30, apply it 20 minutes before sun exposure and don’t skimp. Reapply every two hours or immediately after swimming or sweating. If you tend to skip the sunscreen because it feels too greasy or it’s annoying to put on, find a sunscreen that works better for you.
Wearing sun protective clothing with an ultraviolet protection factor (UPF) of at least 30 is another smart option. Don’t want to invest in UPF tops or bottoms? Search your closet for dark or bright clothes made of dense (not loosely woven) fabric. To guesstimate how much sun protection a clothing item offers, hold it to the light. If you can see through it, it doesn’t offer much.
Medically reviewed by Stacy Chimento, MD
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Get Riverchase Updates in Your Inbox
"*" indicates required fields
Scalp Psoriasis Treatment: What Works?
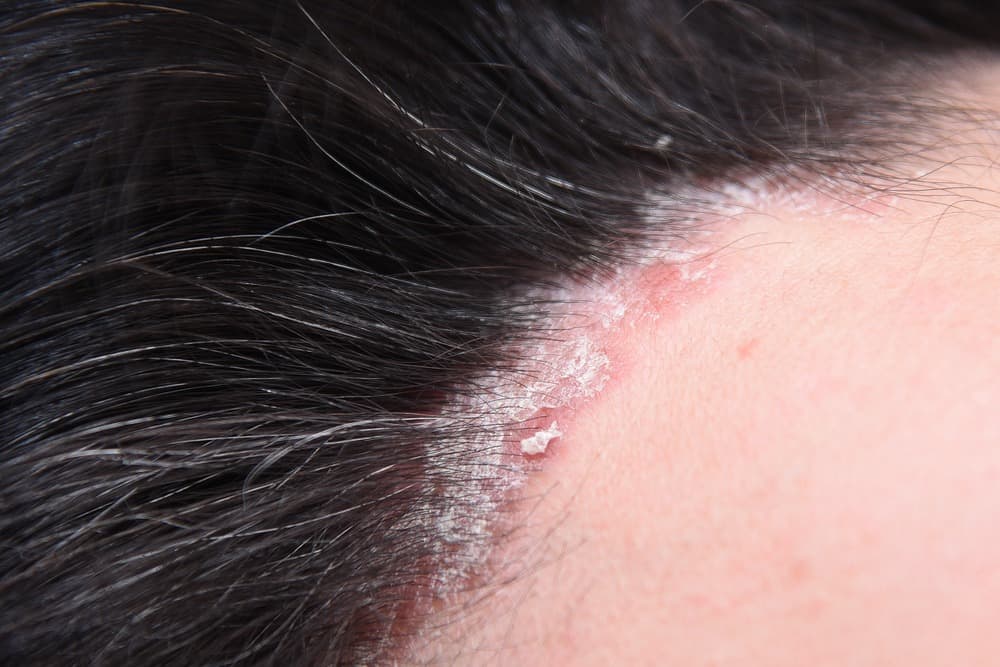
Scalp psoriasis can be so mild you don’t even realize you have it — or it can be impossible to ignore, causing patches of thick and inflamed skin, silvery white scales and a scalp so dry it may crack and bleed. The condition can be embarrassing to live with, and it may be physically painful, too, due to intense itching, burning and soreness.
If you’re one of the 45% to 56% of people with plaque psoriasis who have scalp psoriasis, rest assured that there’s no shortage of treatments available. That said, treating psoriasis of the scalp may take some trial and error, so be patient.
“Scalp psoriasis often proves to be rather stubborn,” said Stephanie Simmerman, APRN, an Advanced Practice Registered Nurse with Riverchase Dermatology.
The scalp psoriasis treatment that works best for you will depend on the severity of your condition and what your skin responds to.
What is scalp psoriasis?
Scalp psoriasis is an inflammatory skin condition in which the immune system causes skin cells to grow too fast — in days instead of weeks. The cells pile up on top of each other, creating thick red patches and skin flakes with a silvery-white sheen. In addition to the scalp, the condition can affect the back of the neck, the forehead and behind the ears.
What causes scalp psoriasis?
The exact cause is unknown, but genes play a role. A variety of triggers can lead to a first episode or a flare-up, including severe stress, cuts and burns, cold and dry weather, tobacco use, heavy drinking, infections such as strep throat and taking medications such as lithium and prednisone.
Scalp psoriasis can be a sign of psoriatic arthritis, a form of arthritis that causes joint inflammation. Skin and joint symptoms can develop at the same time, but most people with psoriatic arthritis develop skin symptoms first.
Scalp psoriasis treatment
There’s no cure for scalp psoriasis, but treatment can reduce the scale and slow the growth of new skin cells.
“The treatment options for psoriasis have exploded over the last few years,” said Simmerman. “Numerous new topicals and systemic medications have come to market with incredible efficacy, safety and prescription drug coverage. While a cure for psoriasis has not been discovered, we have a full tool chest of treatment options.”
At Riverchase Dermatology, treatment often follows a certain pattern. “Each case is unique, but many patients prefer to start with a topical steroid,” said Simmerman. “Usually these are applied to the plaques twice a day for two weeks. If treatment failure presents or a patient has a more severe case, an oral medication or injected biologic may be more appropriate. We also use in-office phototherapy, which is UV light. The light is used to slow skin cell growth and calm inflammation.”
Here’s a closer look at the most common approaches to treating scalp psoriasis. In some cases, your dermatologist may recommend more than one type of treatment. You may be advised to switch treatments after a while to avoid side effects.
Shampoos
What is the best shampoo for psoriasis of the scalp? Coal tar shampoo and salicylic acid shampoo are go-to treatments. Coal tar slows the growth of skin cells, which helps alleviate symptoms such as scaling and itching. You can find coal tar shampoos, such as Neutrogena T/Gel Therapeutic Shampoo, at your local pharmacy.
Salicylic acid shampoo helps soften and dislodge scales. It can be drying and irritating, so ask your dermatologist if it’s right for you. You can buy a salicylic acid shampoo at the drugstore, but a stronger prescription version is often what does the trick.
Topical corticosteroids
Topical corticosteroids are available in a range of potencies and come in foams, solutions, ointments and other forms. They slow the growth rate of skin cells and help relieve redness, scaling and itching.
Long-term use of corticosteroids can cause side effects, such as thinning of the skin, so they’re used for only two to 12 weeks at a time, depending on the severity of your scalp psoriasis and other factors. If you have a mild to moderate case, a topical corticosteroid may be the only treatment you need. But even people with severe psoriasis can benefit from these medications when they’re used together with other treatments.
Intralesional corticosteroids
If you have very thick psoriasis lesions on your scalp, your doctor may recommend intralesional corticosteroids, which are injected into the lesions with a very fine needle.
Topical vitamin D analogues
While not as effective as the most potent topical corticosteroids, these medications, which include calcipotriene and calcitriol, can help with mild to moderate psoriasis. They work by binding to vitamin D receptors, and they slow skin cell production, flatten lesions and remove scale.
Calcipotriene is available in various forms, including creams and foams, but calciferol is available only as an ointment. Treatment with vitamin D analogues lasts for four to eight weeks.
For maximum effect, your dermatologist may prescribe a topical medicine that includes a vitamin D analogue and a corticosteroid.
Topical and oral retinoids
Retinoids, which are derivatives of vitamin A, aren’t just for wrinkles. The topical retinoid tazarotene is helpful for mild to moderate scalp psoriasis. Like other drugs, it slows the overproduction of skin cells. Tazarotene is available as a cream, lotion, foam and gel. Because it can be irritating, it’s often prescribed along with a corticosteroid.
If you have severe scalp psoriasis, your dermatologist may recommend taking an oral retinoid called acitretin to slow cell growth and reduce inflammation. It can be used in combination with other treatments, including phototherapy.
Phototherapy (light therapy)
Various types of phototherapy, particularly narrow band UVB light therapy, have been shown to be effective against scalp psoriasis. Some are delivered by the excimer laser.
Phototherapy controls the condition in several ways, including by suppressing the immune system, slowing cell growth and reducing inflammation. The treatments are administered two to five times a week, usually at a psoriasis treatment center or hospital, and are given for anywhere from weeks to months to years. You may be advised to avoid using salicylic acid shampoo beforehand.
If phototherapy works for you, your dermatologist might prescribe a light box or handheld device you use at home to maintain the benefits.
Apremilast
Apremilast (Otezla) is a twice-a-day pill for moderate to severe scalp psoriasis that reduces redness, scale and plaque thickness. It also reduces itching in some people. The drug is thought to work by reducing the body’s production of inflammatory molecules. In a clinical trial, 43% of patients were clear or almost clear by week 16.
Methotrexate
Intended for severe psoriasis, this strong medication, usually taken in pill form, may be prescribed if you haven’t seen improvement with topical medications or phototherapy. It works by suppressing parts of the immune system.
Cyclosporine
Like methotrexate, cyclosporine is recommended for severe, disabling psoriasis and may be prescribed if other treatments have failed. It’s available as a pill and a liquid. Also like methotrexate, it works by suppressing parts of the immune system. Cyclosporine is very potent and can lead to serious side effects, so it’s not used as a long-term scalp psoriasis treatment.
Biologics
Instead of being synthesized from chemicals, biologics are grown, often with the help of living cells. Many different biologics are FDA approved to treat moderate to severe psoriasis.
Biologics target specific cells and proteins that cause psoriasis and its symptoms, and they often have fewer side effects than drugs that suppress more of the immune system. They can be very effective in patients who haven’t gotten good results from other treatments. These drugs are given intravenously or via injection, some with as few as four doses a year.
For people who also have psoriatic arthritis, biologics can help prevent joint damage or slow the rate of the damage.
Off-label medications
If you have severe scalp psoriasis that hasn’t improved with FDA-approved psoriasis medications, your doctor may prescribe other medications off-label. These include azathioprine, sulfasalazine and tacrolimus, all of which work by suppressing the immune system and are normally used to treat rheumatoid arthritis and/or prevent organ rejection. Another is fumaric acid esters (FAE), which may also suppress the immune system.
Treating scalp psoriasis isn’t one-size-fits all. Working with a dermatologist is the best way to find treatments that help you look better, feel better and restore your confidence.
At Riverchase Dermatology, “Our goal is to help you feel empowered and in control of your chronic inflammatory skin condition,” said Simmerman.
Medical reviewed by Stephanie Simmerman, APRN
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
What Is Alopecia Areata? Understanding Autoimmune Hair Loss
Most men and many women will experience hair loss, or alopecia, at some point in their lifetime. Often it’s due to male-pattern or female-pattern baldness or hairstyles that pull the hair too hard. But for nearly 7 million people, including children, bald patches in hair appear out of the blue. The likely cause: an autoimmune hair loss disorder called alopecia areata.
What is alopecia areata?
Alopecia areata occurs when the immune system mistakenly attacks hair follicles, the openings in the skin through which hair grows. These attacks trigger inflammation, which causes the follicles to shrink and slows the production of hair. Hair production can eventually stop altogether.
It's unclear what causes alopecia areata. Genetics probably plays a role, since the condition often runs in families. It sometimes happens after pregnancy, trauma or significant stress, but usually there’s no obvious trigger.
Because it’s such a visible condition, alopecia areata can be tough to live with. There are plenty of treatment options, though, so if you start finding clumps of hair in your comb or swirling toward the drain when you shampoo, or you notice smooth, shiny, hairless areas on your head, see your dermatologist.
Alopecia areata symptoms
Alopecia areata causes patchy hair loss on the scalp and often on other parts of the body, including the beard area, eyebrows, eyelashes, armpits and pubic area. It can sometimes result in total baldness (alopecia totalis). Even hair follicles inside the nose and ears can be affected. Some people with alopecia areata also develop ridges or pitting (tiny dents) on their fingernails and toenails.
In the most severe cases, all or nearly all of the hair on the body is lost. This type of alopecia areata (alopecia universalis) is rare.
Alopecia areata can have several distinctive characteristics:
- Round or oval bald patches in the hair of the scalp. The skin where the hair has fallen out tends to be smooth and may be peach-colored.
- Small bald patches that merge together to form larger ones. Sometimes one patch will fill in with new hair while a new bald patch forms. The new growth is often white or grey, but it usually returns to your hair’s original color.
- Short, broken hairs shaped like exclamation points (narrow at the base and wider at the top) around the edges of the patches. You would need a magnifying glass to see this.
Some people experience tingling, itching or a burning sensation just before hair falls out.
How long does an episode of alopecia areata last?
Alopecia areata is highly unpredictable. Some people may lose and regrow hair in different areas on and off for many years. Others may get back all their hair after a few months, especially if they don’t have widespread hair loss. If a person loses all the hair on their head and/or their body, it typically happens very fast — within six months.
Alopecia areata treatment
Some alopecia areata treatments work by interrupting the immune system attacks that stifle hair growth. Others directly stimulate the growth of new hair.
Topical medications
Topical medications include minoxidil (Rogaine and others), anthralin (a tar-like substance) and topical corticosteroids. Sometimes two or more topical medications are used at the same time. For example, minoxidil alone is rarely effective for alopecia areata but in some cases it works well when combined with a corticosteroid.
Injectable corticosteroids
A dermatologist administers these shots directly into bald areas, typically every four to six weeks. They’re safe and can be highly effective for people with just a few bald patches. A possible side effect are small dents in the scalp called dells, which eventually go away.
Oral corticosteroids
Oral corticosteroids are sometimes prescribed to treat widespread alopecia areata. Long-term use of these drugs poses serious side effects.
Topical immunotherapy medications
These medicines, intended for widespread or rapid autoimmune hair loss, work by causing a rash that changes how the immune system behaves, but they aren’t widely used. They include diphencyprone (DPCP), dinitrochlorobenzene (DNCB) and squaric acid dibutyl ester (SADBE).
Immunomodulators
Immunomodulators are oral medications that either stimulate or suppress the immune system. Most, including methotrexate, are designed to treat autoimmune conditions other than alopecia areata and are prescribed off-label to treat this form of hair loss.
The exception is Olumiant (baricitinib), the newest alopecia areata medication. It’s a kind of immunomodulator called a JAK inhibitor and was originally developed to treat rheumatoid arthritis. The Food and Drug Administration approved it in June 2022 for adults with severe alopecia areata. In clinical trials, some people got back 80% of the hair on their scalp after taking Olumiant for 36 weeks.
In time, more immunomodulators may become available for autoimmune hair loss.
The best way to deal with alopecia areata is to see a dermatologist, who can develop a custom treatment plan. While you’re waiting for treatment to work, consider wearing a wig or hairpiece if your bald patches are making you embarrassed or depressed, and protect bald areas exposed to the sun or cold with a hat or other cover-up.
Medically reviewed by Dunnett Durando, DO
Written by Maura Rhodes, a health writer and editor based in Montclair, New Jersey
How to Get Rid of Heat Rash (Prickly Heat)
Even if you love hot weather, baking temperatures don’t seem quite as enjoyable when you develop heat rash, also known as prickly heat. How to get rid of heat rash? It typically goes away on its own within a few days. If you need relief in the meantime, heat rash treatment takes the form of cooling the skin and soothing the itching.
What causes heat rash?
Heat rash, or miliaria, happens when sweat ducts and pores become blocked and sweat leaks into the surrounding skin instead of evaporating into the air through the pore. It’s particularly common in infants, whose sweat ducts aren’t fully developed, but adults can develop it too.
Exercising in hot, humid weather is one trigger. A high fever is another. People who sweat a lot or take medication that increases sweating may be especially vulnerable. Wearing tight clothes adds to the problem.
What does heat rash look like?
Heat rash symptoms vary depending on the type of heat rash you have. The rash can develop on the arms and legs, the armpits, the neck, the torso and anywhere clothing or a diaper presses against the skin. It doesn’t usually affect the face.
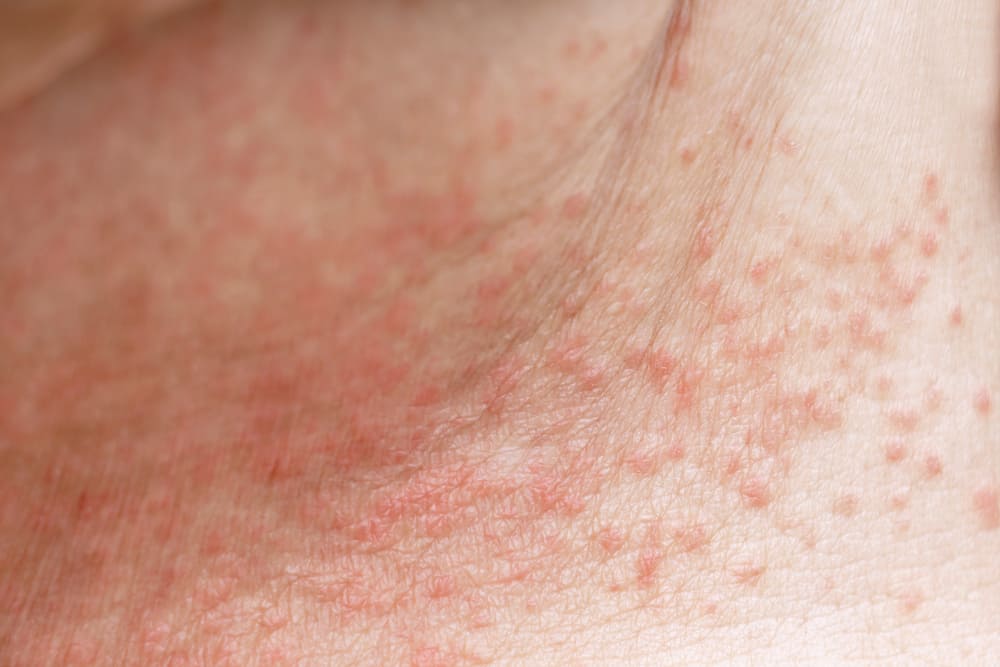
Miliaria rubra
The most common form of heat rash, miliaria rubra, causes small, red, blister-like bumps. It can produce significant itching and a prickly sensation, both of which may get worse when you sweat. In some cases, the bumps may fill with pus.
Miliaria crystallina
Miliaria crystallina is the mildest form of heat rash. It affects sweat ducts close to the surface of the skin. You’ll see tiny, clear, fluid-filled blisters that burst easily.
Miliaria profunda
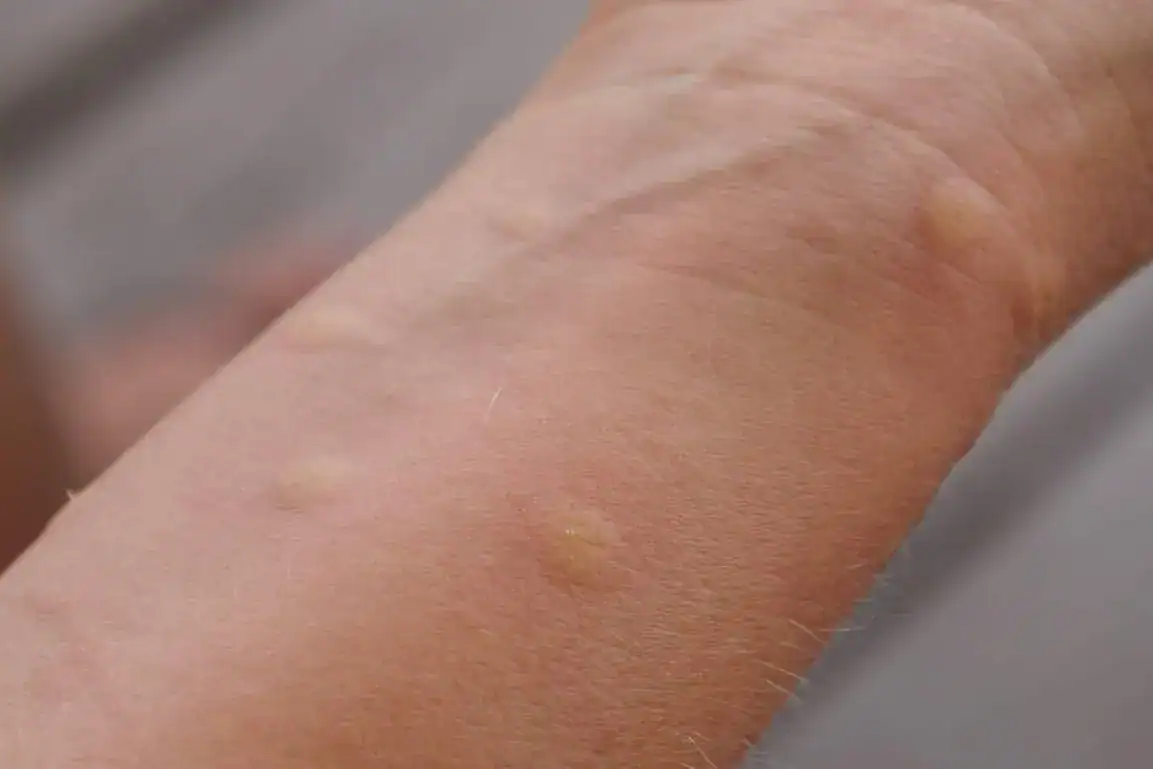
A less common form of heat rash, miliaria profunda can be painful because the bumps are larger and develop deeper in the skin. They can be itchy, but they’re flesh-colored, feel firm and look more like goosebumps than blisters. Miliaria profunda usually affects people who have had several episodes of miliaria rubra in the past.
Heat rash treatment
The number one strategy for easing the itching, bumps or blisters is to get out of the heat and stay somewhere cooler and less humid if possible.
Taking a cool shower or bath and placing a cold washcloth or an ice pack wrapped in a towel on your skin can help. If the rash is itchy, apply calamine lotion or an over-the-counter hydrocortisone cream according to the package directions. Taking an over-the-counter antihistamine may also help.
Don’t use heavy skincare products or talcum powder while you recover since these can block pores. Wear light, loose-fitting clothing that won’t rub on the affected parts of your body. Try your best to avoid scratching, which can lead to skin infection.
For severe cases of heat rash, see a dermatologist, who can prescribe stronger medications to soothe itching and pain. If an infection develops, you may need topical or oral antibiotics. Signs a heat rash is infected include skin that’s warm to the touch, a white or light coloring over the rash, flaking skin, pus that oozes from the rash and boils.
How long does heat rash last? On average, most cases clear up after three or three days.
How to prevent heat rash
To reduce your risk of developing heat rash, follow these tips.
- When possible, limit the amount of time you spend in hot, humid environments.
- Choose light, loose-fitting clothes. Avoid wearing synthetic fabrics that don’t allow skin to breathe.
- Try to exercise during cooler times of day and wear moisture-wicking workout clothing.
- Drink plenty of fluids.
- Take cool showers or baths on hot, humid days.
Medically reviewed by Andrew Jaffe, MD, FAAD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Get Riverchase Updates in Your Inbox
"*" indicates required fields
Best Nail Fungus Treatment: What Works for Yellow Nails
Nail fungus isn’t pretty. The nails can become misshapen, thick, crumbly and brittle. They may turn a nasty color — yellow, green or brown. Fungal infections of the nail (onychomycosis) can also produce a slightly foul smell. If you’ve developed toenail fungus or fingernail fungus, you’re no doubt searching for the best nail fungus treatment, one that will restore your nails to normal as quickly as possible.
So, how to get rid of nail fungus fast? Unfortunately, it’s not easy. It may take trial and error to find the best nail fungus treatment for you, and no treatment for nail fungus can get rid of it overnight.
There are many over-the-counter nail fungus medicines available, but they may take two months or longer to work, if they work at all — and the nail fungus may return. Topical medicines treat the fungus on the skin surrounding your nail but aren’t as effective at killing fungus in the nail bed.
If you think you have nail fungus, see you dermatologist to make sure. The dermatologist can make an accurate diagnosis and come up with a treatment plan.
Your dermatologist will likely trim the infected nail and scrape away any debris under it, which helps get rid of some of the fungus. The doctor may take a sample of the fungus to identify which type is causing the infection, which helps them decide the best treatment. Your nail fungus treatment plan may include any of the following.
Topical nail fungus medicines
Topical nail fungus medicines are available in several forms, including nail polishes and solutions applied by dropper. Prescription topicals include ciclopirox (Penlac), efinaconazole (Jublia), amorolfine (Curanail and others) and tavaborole (Kerydin). You’ll have to you use them every day or every week for up to a year.
Using topical anti-fungal products alone isn’t always effective, however, because nails are thick and difficult to penetrate. Unless your infection is mild, your dermatologist may suggest you combine a topical medicine with a prescription oral anti-fungal medication.
There are some exceptions. Topicals alone may be prescribed if you have a fungal nail infection caused by a mold, or if you have a less common form of nail fungus called white superficial onychomycosis, which affects only the surface of the nail and causes white spots that eventually become powdery.
Oral anti-fungal medicines
In many cases, you’ll need to take oral anti-fungal medicine prescribed by your dermatologist to get rid of nail fungus completely. Commonly prescribed anti-fungals include itraconazole (Onmel, Sporanox) and terbinafine (Lamisil). These medications are usually taken for at least three to four months.
The downside to oral anti-fungals is the potential for side effects. Side effects may include fever, dry mouth, nausea and diarrhea. Very rarely, liver damage occurs.
Laser treatment for nail fungus
Certain types of laser therapy can tackle stubborn nail fungus by destroying the fungus with heat. One research review showed that laser treatment using a perforated CO2 laser or yttrium-aluminum-garnet (YAG) laser has a moderately high cure rate and strong safety record. Multiple treatments are typically needed. Side effects can include mild to moderate pain and bleeding.
Removing the nail
If other treatments fail, your dermatologist may recommend removing the nail and allowing a healthy nail to grow in its place. Nail removal can be done in the office by applying a chemical that destroys the nail or by removing it surgically. It takes four to six months for a fingernail to regrow and at 12 to 18 months for a toenail to regrow.
Home remedies for nail fungus
Some people try over-the-counter products such as Vicks VapoRub or tea tree oil as home remedies for nail fungus. Vicks VapoRub contains camphor and eucalyptus oil, which may have anti-fungal effects when applied regularly over time. Tea tree oil for nail fungus could in theory help because the oil has anti-fungal properties. But don’t count on either of these for a fast or permanent cure. Seeing a dermatologist is your best bet for treating nail fungus.
Medically reviewed by Andrew Jaffe, MD, FAAD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.