Poison Ivy Rash: The 6 Best Home Remedies
Even if you know exactly what the poison ivy plant looks like (“leaves of three, let it be”), it’s easy to stumble into a patch of it without noticing. Your mistake may become clear hours or days later, when the poison ivy rash appears, complete with redness, intense itching and blisters. As far as poison ivy treatment goes, most cases can be tended to at home. If you’re itching to know the best home remedies for poison ivy, look no further.
Below are six dermatologist-recommended home remedies that should help calm the rash and ease the itching.
If the rash hasn’t gotten better after 7 to 10 days or if pus is oozing from it (a sign of infection), make an appointment with your dermatologist, who might prescribe a prescription corticosteroid or an oral antibiotic. If you have a severe allergic reaction to poison ivy, see a doctor right away or go to the emergency room. Signs of a severe reaction include facial swelling, a fever, itching that gets worse or prevents you from sleeping, a rash around your mouth, genitals or one or both eyes, and a rash that covers most of your body.
1. Calamine lotion
This distinctive pink lotion contains zinc oxide, which relieves itching by creating a cooling sensation when it evaporates from your skin. Wash your skin first. Shake the calamine lotion bottle, apply some lotion to a cotton ball or pad, gently apply it to the rash area and let it dry. Don’t bandage your skin or wrap it with anything. You can reapply calamine lotion every six to eight hours.
2. Hydrocortisone cream
A topical steroid, hydrocortisone cream stops the release of inflammatory substances that cause the itching, redness and swelling of poison ivy rash. Dab a thin layer onto the affected area and rub it in gently two to three times a day. Wash your hands afterward. Again, don’t bandage your skin or wrap it with anything. Don’t use a hydrocortisone product for more than a week unless your doctor instructs you to.
3. An oral antihistamine
Over-the-counter allergy medicines such as Zyrtec, Allegra, Claritin and Benadryl can help calm inflammation and itching. So-called “first generation” antihistamines, such as Benadryl, cause drowsiness and are particularly helpful when taken at night if the itching makes it hard to sleep. Don’t use an antihistamine cream or lotion, however, as these can make the rash worse.
4. Short, lukewarm baths or cool showers
If you take baths, add a colloidal oatmeal treatment to the bath water to soothe your skin and reduce itching. You can buy these at your local pharmacy (Aveeno Soothing Oatmeal Bath Treatment is one example), or you can make your own. Simply grind uncooked whole oats in a food processor down to a fine powder. Add 1 cup of it to your bath water and soak for 10 to 15 minutes. If you don’t have oats on hand, use 1 cup of baking soda instead.
5. Cool compresses
Soak a clean washcloth in cold water, wring it out, and apply it to the rash to ease the itch and reduce swelling. Leave it on for 15 to 20 minutes and repeat throughout the day.
6. Aluminum acetate gel or powder
Aluminum acetate is an astringent that cools and calms skin conditions such as poison ivy rash. It also has a drying effect on wet or weeping blisters. Aluminum acetate solution is available as a gel, such as TriCalm Hydrogel, and as a powder (Gordon’s Boro-Packs, Domeboro) that you combine with water to create a compress. To make a compress, follow the instructions on the box, then place the compress on the rash for 15 to 30 minutes.
Medically reviewed by Andrew Jaffe, MD, FAAD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
What’s the Best Sunscreen for You?
Wearing sunscreen daily, rain or shine, is a must for fighting signs of aging and reducing your risk of skin cancer. But what’s the best sunscreen? Sunscreens aren’t one-size-fits-all. Picking one is like choosing a hat: You need to find one that works for you. Do you run from products that feel greasy? Prefer all-natural ingredients? Want to avoid skin irritation at all costs? Hate to reapply?
To find the best sunscreen for your face and body, read on to learn the standards it should meet and which formulations are likely to keep you coming back for more. You may decide you want different sunscreens for different parts of your body or different circumstances. Do a little experimentation to find what works.
The three essential requirements
For adequate protection from the sun’s damaging rays, your sunscreen should meet certain basic requirements. Choose a sunscreen that:
- Is labeled “broad spectrum,” which means it shields you from UVA and UVB rays, both of which damage the DNA in skin cells and increase the risk of skin cancer
- Has an SPF of at least 30
- Is labeled “water resistant”
Cream, gel, stick, spray or powder? Take your pick
Convenience and comfort matters. If you choose a sunscreen you like and find easy to apply, you’ll be more inclined to use it regularly and apply a sufficient amount.
Sunscreen formulation is mostly a matter of personal preference. The best sunscreen for men may be a gel formulation, since these go on light and are ideal for hairy areas such as the face, chest and scalp.
Cream sunscreens are ideal for dry skin and are often considered the best sunscreen for the face, although if your face is oily or acne prone, you’ll want a lighter, oil-free version.
Sunscreen sticks are handy to throw into a bag and are particularly useful for covering the area around your eyes, since they don’t run. If you’ve sworn off sunscreen because it stings your eyes, try a sunscreen stick.
Powder sunscreens are increasingly popular. They’re not ideal as your primary sunscreen, but they’re perfect for reapplications in the car and on the go, especially when you’re wearing makeup.
Some people like spray-on sunscreen the best. Many parents find it the easiest formulation to apply to kids — but you need to hold it close to their body and spray generously. It’s hard to tell if you’ve missed any spots, so you should rub it in to be safe. On windy days, skip the spray and opt for a different formulation.
Deciding between chemical and mineral
Sunscreen is sold in two varieties: chemical and mineral. Chemical sunscreens absorb UV rays before your skin can soak them up. Mineral sunscreens, also called physical sunscreens, sit on your skin and create a barrier that UV rays can’t penetrate. Both have pros and cons.
Are you the type who never remembers to apply sunscreen until you’re already on the beach or golf course? Mineral sunscreens may not go on as smoothly, but they start working right away. Chemical sunscreens, on the other hand, don’t work until they have been absorbed into the skin, which can take 10 minutes or more.
Hate that white sunscreen cast on your skin? Choose a chemical sunscreen, or look for a mineral sunscreen that’s tinted.
Sensitive skin? If you have a skin issue such as rosacea, mineral sunscreens may the better bet, since ingredients in some chemical sunscreens can irritate the skin. If sun exposure makes your melasma worse despite wearing sunscreen, try a tinted mineral sunscreen that contains iron oxide as an additional ingredient (look for it in the inactive ingredient list).
Concerned about potential harm caused by sunscreen chemicals that enter the bloodstream? Choose a mineral sunscreen, since these stay on top of skin.
Want to make the more environmentally friendly choice? Again, for go for mineral sunscreen. Some chemical sunscreens contain ingredients, including oxybenzone, moctinoxate, and octocrylene, that can be harmful to marine life and coral reefs.
Water resistance: How much is enough?
There’s no such thing as a waterproof sunscreen, except maybe a wetsuit. But some sunscreens are more water resistant than others. If you tend to wash or sweat your sunscreen off, know that chemical sunscreens are typically more water resistant than mineral sunscreens.
The FDA requires manufacturers of water resistant sunscreens to test how long the water resistance lasts and indicate on the label how often the product should be reapplied — after either 40 or 80 minutes when swimming or sweating. If water resistance is a big concern for you, look for one that’s rated water resistant for up to 80 minutes.
Top sunscreen picks for all of your needs
Among the countless sunscreens on the market, here are 13 that make the list of dermatologist favorites.
Best sunscreen for the body
EltaMD UV Sheer Broad-Spectrum 50+
SkinCeuticals Physical Fusion UV Defense Sunscreen SPF 50
Best sunscreen for the face
EltaMD UV Sheer Broad-Spectrum SPF 50+
COOLA Classic Face Organic Sunscreen Lotion SPF 50
Best sunscreen for men
Supergoop Unseen Sunscreen SPF 40
Neutrogena Hydro Boost Water Gel Lotion SPF 50
Best sunscreen for sensitive skin
Neutrogena Sensitive Skin Face Mineral Sunscreen SPF 50
CeraVe Hydrating Mineral Sunscreen SPF 50 Body Lotion
TiZO3 Primer/Sunscreen Tinted SPF 40
Best sunscreen for oily or acne-prone skin
La Roche-Posay Anthelios Clear Skin Oil Free Sunscreen SPF 60
Neutrogena Clear Face Breakout Free Liquid Lotion Sunscreen SPF 50
Best sweat-resistant sport sunscreen
Neutrogena Ultimate Sport Face Oil-Free Lotion Sunscreen SPF 70+
Coppertone Sport Mineral Sunscreen Lotion SPF 50
Best tinted mineral sunscreen
Alastin HyrdaTint Pro
Medically reviewed by Lucy L. Chen, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Hand, Foot and Mouth Disease in Adults and Kids: Get the Facts
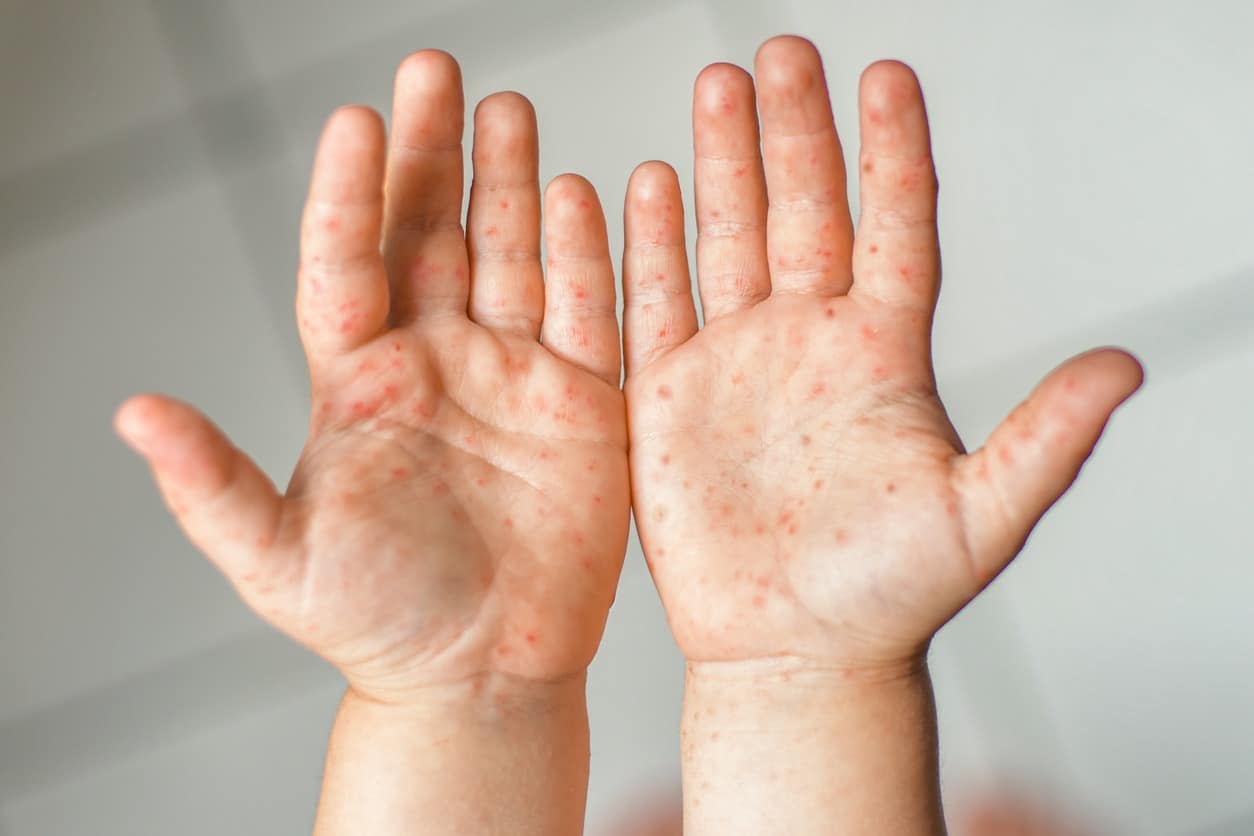
When your child develops an itchy rash in the summer or fall, you might first suspect poison ivy or heat rash, but there’s another potential culprit to consider: Hand, foot and mouth disease. This highly contagious viral infection usually occurs in children under age 5. Hand, foot and mouth disease in adults is less common and often causes mild symptoms or no symptoms.
What is hand, foot and mouth disease?
As you can guess from the name, hand, foot and mouth disease rash affects the hands, feet and mouth. It can also appear on other parts of the body, such as the diaper area, knees and elbows. The disease is caused by viruses that are part of the enterovirus family, which usually cause mild illnesses. In the United States, coxsackievirus A16 is to blame in most cases. Young children are more susceptible to hand, foot and mouth disease than adults in part because they haven’t yet developed immunity to these viruses.
Hand, foot and mouth disease symptoms
Different stages of hand, foot and mouth disease are associated with different symptoms. During the first day or two of infection, symptoms can include a sore throat, low fever, stomach pain and reduced appetite. A sick person is most contagious at this point.
Around day three, these symptoms go away and are replaced by:
- Mouth sores. The sores can develop anywhere in the mouth, or even the back of the throat, but they often appear on the tongue. At first they look like tiny bumps or bright pink spots, but they eventually become blisters, which can be painful. Swallowing may be uncomfortable, so young children may drool more than usual, refuse to eat or want only cold drinks.
- Itchy rash. The hand, foot and mouth disease rash looks like red, flat spots that quickly give way to bumps or small, red blisters that have fluid near the surface. The blisters scab over as they heal. Some children don’t develop a rash, only mouth sores.
- Swollen glands (lymph nodes) in the neck. Some people develop these, others don’t.
How the disease spreads
There are several ways to contract the virus. These include:
- Touching the blisters of someone who has it
- Kissing, hugging or sharing utensils with someone who has it
- Touching an infected child’s feces while changing their diaper and then touching your eyes, nose or mouth
- Touching objects contaminated with the virus, such as doorknobs or toys
- Breathing droplets expelled by an infected person’s cough or sneeze
The virus is particularly common in kids who attend daycare, for reasons you can well imagine — the toilet training and countless diaper changes that happen there, as well as small children’s fondness for putting their hands and objects in their mouth.
Treatment for hand foot and mouth disease
There is no particular treatment for the virus, which typically improves on its own in seven to 10 days. Adults can relieve a fever with aspirin, but infected children and teens should be given acetaminophen (Tylenol) instead.
These strategies can help soothe mouth sores:
- Avoid spicy, salty or acidic foods and beverages (such as orange juice and soda)
- Drink cold beverages
- Suck on ice cubes or popsicles
- Eat cold foods such as ice cream, sherbet or sorbet
- Swish warm salt water around the mouth several times day (for adults and for children who can avoid swallowing the water)
If mouth sores are particularly painful and the child is old enough to gargle, a doctor can prescribe a mouthwash that contains several beneficial ingredients, including a painkiller.
If an infected child is under six months old or has a weakened immune system, or if the symptoms are severe, go to a doctor. Contact your child’s pediatrician if the fever lasts longer than three days, symptoms don’t improve after 10 days or your child is dehydrated. Signs of dehydration in kids include dry lips, dark urine, decreased urination, and dizziness, fatigue or lightheadedness.
Any woman who gets hand, foot and mouth disease while pregnant should contact her doctor.
In very rare cases, hand, foot and mouth disease can lead to serious complications such as viral meningitis and encephalitis. Symptoms of meningitis include an extremely painful headache and neck stiffness. Encephalitis causes a painful headache and confusion. Loss of fingernails or toenails is another rare complication, but the nails usually regrow.
Medically reviewed by Andrew Jaffe, MD, FAAD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Dermatologist’s Best Face Moisturizer for Every Skin Type
Are you still searching for your “holy grail” face moisturizer? The one that makes your skin soft and supple and not greasy or irritated? It’s easy to get overwhelmed by the sea of options when you’re trying to figure out the best choice for your skin type and concerns, yet the right face moisturizer can do wonders for the health of your skin barrier as well as your appearance.
Whether you’re looking for the best drugstore moisturizer or you’re willing to splurge a little, read on to find your perfect moisturizer match with advice from Lucy L. Chen MD, FAAD, a board-certified dermatologist at Diane Walder Dermatology by Riverchase.
Best moisturizer for dry skin
Dry skin isn’t just a cosmetic issue. It indicates that your skin barrier, the outermost part of the skin’s top layer, is weakened and less effective at retaining moisture and blocking the entry of bacteria, pollution and allergens.
“To repair the skin barrier, one of the best ingredients to look for in a face moisturizer is ceramides,” Dr. Chen said. Ceramides are fats naturally found in the skin barrier. When levels decrease — which tends to happen with age — skin can become dry and easily irritated.
The consistency of the moisturizer is also key. Creams are best, since lotions and gels might not provide enough hydration. If your skin is very dry, you may want to bypass creams and choose an occlusive balm or ointment. Occlusives create a protective seal over the skin that traps water and keeps it from evaporating. Occlusive ingredients include lanolin, mineral oil and squalene.
Top picks
Here are Dr. Chen’s top picks for dry skin.
Creams
- SkinCeuticals Triple Lipid Restore 2:4:2
- LaRoche-Posay Toleriane Double Repair Face Moisturizer
- CeraVe Moisturizing Cream
Balms and ointments
- SkinCeuticals Hydra Balm hydrating occlusive ointment for traumatized or severely dry skin
- Aquaphor Skin Soothing Balm
- Vaseline Healing Jelly
Best moisturizer for acne-prone skin
If you’re prone to pimples, you might be tempted to steer clear of moisturizer for fear it could make your acne worse. But using a lightweight face moisturizer designed for your skin type is an important part of an acne-fighting skincare routine.
“If you have acne, your skin barrier is compromised, and this can be worsened by products you use to treat pimples that make skin dry and more irritated,” Dr. Chen said. “By keeping your face moisturized, you can better tolerate acne medications.”
The best face moisturizer for you is one with a light consistency, such as a water-based gel cream labeled “non comedogenic,” meaning it won’t clog pores. These products often contain hyaluronic acid, which acts as a humectant — an ingredient that draws moisture into the upper layer of skin. Or you may prefer to use a hyaluronic acid serum. Avoid products with heavy ingredients that can exacerbate acne, such as mineral oil and coconut oil.
Top picks
Here are Dr. Chen’s top picks for acne-prone skin.
- Riverchase Skin Solutions Pure Hydration Hyaluronic Acid
- Riverchase Skin Solutions Ultra Lite Moisturizer
- Neutrogena Hydro Boost Water Gel with hyaluronic acid
Best moisturizer for oily skin
Like people who have acne-prone skin, those with oily skin also sometimes hesitate to use moisturizer. But unless your skin is extremely greasy, it’s a good idea to make moisturizer part of your skincare routine, especially since many moisturizers also contain anti-aging ingredients that can keep your skin looking youthful, Dr. Chen said.
She recommends many of the same types of lightweight moisturizers for oily skin that she does for acne-prone skin, such as water-based gel creams. “However, many people with oily skin find they really like mattifying moisturizers, which are formulated to absorb some of the extra oil you produce,” Dr. Chen added.
Skip heavy creams and any moisturizer that promises to give your skin a “dewy” look, which can make your face shinier.
Top picks
Here are Dr. Chen’s top picks for oily skin.
- Riverchase Skin Solutions Ultra Lite Moisturizer
- Neutrogena Hydro Boost Water Gel with hyaluronic acid
- LaRoche-Posay Effaclar Mat mattifying moisturizer for oily skin
- Cetaphil Derma Control Oil Absorbing Moisturizer SPF 30
Best moisturizer for combination skin
“When you have combination skin, finding the best moisturizer is particularly tricky,” Dr. Chen said. “It can take a lot of trial and error to see what works best.”
To avoid making oilier parts of the skin worse, she recommends lightweight moisturizers such as water-based gel creams. If your skin has more dry patches than oily ones, look for a moisturizer that contains glycerin, a more powerful humectant than hyaluronic acid.
Top picks
Here are Dr. Chen’s top picks for combination skin.
- Vichy Aqualia Thermal Water Gel hydrating gel moisturizer
- Neutrogena Hydro Boost Water Gel with hyaluronic acid
- SkinCeuticals Daily Moisture lightweight pore-minimizing moisturizer for normal or oily skin
Best moisturizer for sensitive skin
If you have sensitive skin, “the simpler, the better” should be your motto when you’re shopping for moisturizer. Ideally, the ingredient list is short and the product doesn’t contain any fragrance, which is a common irritant. Avoid moisturizers with exfoliating alpha-hydroxy and beta-hydroxy acids such as salicylic, lactic and glycolic acid. These may be helpful for other skin types but they can disrupt the skin barrier in people with sensitive skin.
“Look for calming ingredients, including colloidal oatmeal and soy,” Dr. Chen said. “They’re both generally well tolerated, whereas some people’s skin is so sensitive that they may develop a contact allergy to other ingredients that are normally soothing, such as aloe.”
Top picks
Here are Dr. Chen’s top picks for sensitive skin.
- CeraVe Daily Moisturizing Lotion
- Aveeno Calm + Restore Oat Gel Moisturizer for sensitive skin
- LaRoche-Posay Toleriane Fluide lightweight moisturizer for sensitive skin
Medically reviewed by Lucy L. Chen MD, FAAD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Dr. Dunnett Durando's Tips for Skin Cancer Awareness Month
Every May, dermatologists use skin cancer awareness month as an opportunity to educate their patients and the public about the important steps they can take to prevent skin cancer. In this interview, Riverchase Dermatology’s Dr. Dunnett Durando shares her tips for protecting yourself and your loved ones from skin cancer. From wearing sunscreen, protective clothing, hats, and glasses to limiting your exposure to the sun during the peak hours of 10 a.m.-2 p.m. and seeking shade when you are outside, there are a number of ways you can prevent your exposure to the sun.
The three major types of cancer are basal cell carcinoma, squamous cell carcinoma, and melanoma. Since melanoma is the most-deadly form of skin cancer, Dr. Durando explains what you need to know about the ABCDEs of melanoma and how you can identify whether you need to make an appointment to see your dermatologist.
One of the keys to treating and surviving skin cancer is early detection, so Dr. Durando recommends her patients conduct monthly skin checks to monitor their skin over time and spot moles that are new and changing.
6 Melanoma Symptoms You Should Never Ignore
You’ve probably heard that melanoma is the deadliest form of skin cancer, but be honest: When was the last time you scanned your skin for any suspicious growths? Even if you’re keeping an eye on a mole or two, you may not realize that the majority of melanomas don’t start from existing moles — and some grow on under a nail, where most people don’t think to look. Knowing what melanoma symptoms to watch for can help you spot this cancer early, when it’s more treatable.
Look out for the following symptoms of melanoma in between regular skin cancer screenings at your dermatologist’s office. If you’re not sure whether a new growth or spot or a change in an existing one is cause for concern, err on the side of caution and report it to your dermatologist.
A new spot anywhere on the skin (even where the sun doesn’t shine)
While melanoma can develop in a mole you already have, 70% to 80% of these cancers occur on normal-looking skin. If you perform regular skin self-exams, you’ll get familiar with the location and pattern of your moles and spots and have a much better chance of noticing new growths.
Melanoma can develop anywhere on the body, even in areas that don’t get any sun. Be sure to check your whole body, including areas you can’t see on your own, like your back. Use a full-length mirror and a hand mirror to check them, or have a friend or partner check them for you.
These are areas people often miss:
- The bottoms of your feet
- The palms of your hands
- The skin between your fingers and toes
- Your scalp
- Your eyelids
- Behind your ears
A mole with one or more ABCDEs of melanoma traits
Dermatologists use the ABCDE rule to identify potentially cancerous moles and spots. Here’s what each letter stands for.
- A is for asymmetry. Most melanomas aren’t symmetrical. In other words, one half of the mole doesn’t look like the other half.
- B is for border. Melanomas may have irregular borders, with edges that may be notched or scalloped.
- C is for color. While noncancerous moles are usually a single shade of brown, melanomas can be multicolored. A melanoma may be a combination of tan, black and brown. As the cancer grows, it might look red, white or blue.
- D is for diameter. A mole that’s 1/4 inch in diameter (the size of a pencil eraser) or larger can be cause for concern.
- E is for evolving. Melanoma tends to change over time. Be on the lookout for changes in size, shape, color or elevation. If a mole or growth starts to bleed, hurt or itch, or if it becomes scaly or crusted, those changes count as evolving, too.
An ugly duckling mole
Experts recommend checking for “ugly duckling moles,” moles that look clearly different from nearby moles. An ugly duckling mole may be larger, smaller, lighter or darker than the others. Ugly ducklings can also be lone moles that don’t have any other moles nearby.
Are ugly duckling moles always melanoma? No, but if you spot one, it’s worth bringing to your dermatologist’s attention right away.
A pink, red, purple or colorless spot
While it’s unlikely to be cancerous, a pink, red, purple or clear growth or spot can be a sign of a rare, aggressive type of melanoma called amelanotic melanoma, especially if it changes over time. It may be the same color as your normal skin color or very close to it, making it difficult for you and even your doctor to detect.
Amelanotic melanomas are easily mistaken for scars or cysts. Fair-skinned people are more likely to develop them.
Nail streaks, bumps or splitting
Rarely, melanoma can develop under or around the fingernails or toenails. Melanoma that grows in the nailbed (under the nail) is called subungual melanoma. The thumb and the big toe, especially of the dominant hand, are the most common sites.
Melanoma in the nail can appear as a brown or black streak or an irregularly shaped spot in the nail, or as a bump or nodule under the nail. As the disease advances, the nail may lift and separate from the nail bed and split. You may notice dark skin next to the nail.
Ocular melanoma symptoms (floaters, iris spots and others)
Ocular melanoma, or melanoma in the eye, is very rare. It’s also hard to detect because oftentimes there are no signs that you can see in the mirror, and many people don’t have symptoms in the early stages — a good reason to have regular eye exams.
Signs and symptoms of ocular melanoma include blurred or changed vision, floaters (drifting specks in your vision), flashes, a dark spot on the iris (the colored part of your eye), a blind spot in your peripheral (side) vision and a change in the shape of one of your pupils.
Melanoma strikes people of all races and ages. Performing a simple skin self-exam once a month to look for melanoma symptoms takes only a few minutes. If you notice something suspicious, don’t try to decide if it’s likely to be melanoma or not — that’s what your dermatologist is for. Be on the safe side and make an appointment.
Medically reviewed by Andrew Jaffee, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How Often Should You Exfoliate Your Face?
You absolutely love the smooth-as-a-baby’s-bottom feeling that exfoliating gives your skin. But the phrase “too much of a good thing” applies to skin exfoliation. So how often should you exfoliate your face?
The answer depends on your skin and how it reacts to exfoliation. The right frequency for you may be three times a week, once a week, every other week, or never. Read on to learn more.
What is exfoliation?
Exfoliating means removing dead skin cells from the top layer of skin. These cells slough off on their own eventually, but sometimes they need a little encouragement.
You can exfoliate in two ways. One is by using an exfoliating scrub, sponge, brush or glove or even just a washcloth to scrape away the dead cells. The other is by using an exfoliating product that contains a chemical that dissolves the cells, revealing the living cells underneath.
“Chemical exfoliants contain acids such as salicylic acid, glycolic acid and lactic acid,” said Annie Gonzalez, MD, a board-certified dermatologist at Riverchase Dermatology.
The best exfoliating method for your face depends on your skin type, Dr. Gonzalez noted.
“Mild chemical exfoliants are a better choice if you have dry, sensitive or acne-prone skin because they’re gentler than exfoliating scrubs,” she explained. Scrubs are easy to overuse and may damage your skin.” Mild chemical exfoliants are also the best bet for mature skin, which tends to be thinner and drier than younger skin.
Physical exfoliants and stronger chemical exfoliants are more suitable for oily, thicker skin. But if your skin is dark, or if it develops dark marks after skin injuries or breakouts, you may want to avoid them, since more aggressive exfoliants can cause dark spots.
The benefits and risks of exfoliating your face
By sloughing off dead skin cells and other debris that accumulates on your face, exfoliating makes your skin looks healthier, brighter and more youthful. Over time, it can also increase the production of collagen, which decreases as you get older. Collagen is a protein naturally found in the skin that keeps it looking firm.
If your skin has age spots from sun damage, exfoliating regularly can make them less noticeable. And if you have acne, skin exfoliation can help reduce breakouts. People with acne-prone skin don’t shed dead skin cells as effectively as those who aren’t prone to breakouts. When dead skin cells accumulate on the face, they can clog pores and lead to blemishes. Exfoliation helps keep pores clear.
Exfoliating your face too often, however, can dry out your skin and worsen your complexion, causing redness, irritation and breakouts.
How often to exfoliate your face: The best schedule for you
You may need to experiment to find the exfoliation frequency that gives you all of the perks of exfoliation and none of the downsides. Start with the general guidelines below. Cut back if you develop dryness, redness or irritation or you start to break out. Take a break from exfoliating your face if you have a sunburn, rash or open cut.
Keep in mind that if you use an exfoliating cleanser such as SkinCeuticals Clarifying Exfoliating Cleanser every day, you may not need to do any additional exfoliation.
Normal skin
People with normal skin should start by exfoliating two to three times a week.
Dry, sensitive skin
For people with dry or sensitive skin, exfoliating twice a week is the maximum frequency dermatologists recommend. You may want to exfoliate only once a week or even every other week if you use products that can cause dryness and irritation, such as retinoids.
Rosacea-prone skin
If you have rosacea, your dermatologist may recommend avoiding exfoliation so as not to cause further redness, irritation or stinging.
Combination skin
People with combination skin can typically exfoliate their face twice a week.
Oily skin
If you have oily skin, you can probably exfoliate two or three times a week, and possibly more often depending on what exfoliation method or product you use and how your skin reacts.
Medically reviewed by Annie Gonzalez, MD
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Water’s Edge Dermatology, Prevention magazine, jnj.com, BCRF.org, and many other outlets.
What Are Infantile Hemangiomas? Dr. Robin Gehris Explains
Riverchase Dermatology’s Dr. Robin Gehris is triple board-certified in pediatric dermatology, dermatology and pediatrics, and she has a special focus on treating infantile hemangiomas. In this interview, she explains what infantile hemangiomas are and how they are treated.
Infantile Hemangiomas
About 4% of babies are born with hemangiomas either at birth or that develop shortly after birth. Hemangiomas represent a collection of extra blood vessels in the skin that are not always present at birth. Many parents think of these growths as birthmarks, but they can develop very rapidly in the first few months of a baby’s life. The most rapid growth phase is from months 0-4 with more gradual growth phase during months 6-12. Infantile hemangiomas seem to be more common in baby girls and babies who are born prematurely. Little is known about why some babies have them and others do not. This is an area of active research. Hemangiomas can occur anywhere on a baby’s skin, but the locations that are most concerning to doctors are on the face, around the eyes, the mouth or nose, on the neck or around the diaper area – places where the hemangioma could impact breathing or vision, cause discomfort or ulcerate. If a baby has a hemangioma in these areas, parents should have them checked out by a pediatrician or pediatric dermatologist as soon as possible. Since hemangiomas can grow rapidly, the earlier the hemangioma is identified, the easier it can be to treat. Dr. Gehris says that in the last five to 10 years, new oral medications have been approved by the FDA to help treat infantile hemangiomas and they can be used to treat babies topically with a gel formulation. The treatment options now available are life changing and they can make a great difference in the quality of a baby’s life.
Learn more about hemangiomas and how to treat other vascular malformations.
The State of Psoriasis
Having investigated and treated Psoriasis for over 40 years now, I am writing this article to honor the millions of patients and their families who have been affected by the disease. Psoriasis is common, affecting 2.5% of the US population, estimated at over 8 million people. Psoriasis does not discriminate: it affects all races, men, women and children.
Psoriasis is not only skin-deep. Psoriasis was initially thought to be just a skin disease with rapidly dividing cells that accumulated on the surface. After decades of laboratory research using blood and skin samples donated by patients, we now know that psoriasis is a type of autoimmune disease which affects skin, joints, and almost every other organ system caused by self-made natural inflammatory substances.
In the remainder of this article, I will include questions from patients on my blog which I have updated to shed some light on some of the latest developments in psoriasis research:
Where are the most common areas to get psoriasis?
Psoriasis seems to be induced or aggravated by trauma. Thus, the most commonly involved areas are the scalp (often first to appear), elbows and knees, tailbone area, and genitalia.
Is psoriasis genetic? No one in my family has it.
Psoriasis is considered a genetic disease because many different genes have been discovered in family members that are associated with psoriasis. The gene or genes are only one part of the story, however. There also has to be trigger from the environment.
What are some of the triggers for psoriasis?
The trigger that is most well known is infection, particularly with the Streptococcus bacteria. In people who don’t have the genetics for psoriasis, the skin disease may go away after the infection, but in those who do, it may progress into chronic psoriasis.
Other triggers include severe stress, cold and dry climates, smoking, and some drugs such as beta-blockers, lithium, hydroxychloroquine, and interferon. Prednisone is more likely an aggravator of existing psoriasis rather than a trigger of new psoriasis.
What is Psoriatic Arthritis?
Psoriatic arthritis is an inflammatory arthritis that is caused by the same genes and circulating chemicals that cause the skin disease. It may affect up to 30% of patients with skin psoriasis. There are a few types of arthritis, but the most common one affects the small joints of the hands and feet and causes morning stiffness and swelling, very similar to rheumatoid arthritis.
Can children get psoriasis? Most of the people I know with psoriasis are adults.
Absolutely yes! Psoriasis is often considered an adult disease because the average age of onset is about 30 years. Here are some surprising statistics: 30% of all new cases of psoriasis start before age 15, 10% before 10 years, and 2% before 2 years. Babies can even be born with psoriasis! The incidence of psoriasis is estimated to be 3 new cases per year per 1000 children.
Besides the skin and joints, what other organ systems are affected by psoriasis?
The most important association is the “metabolic syndrome” which includes obesity, type 2 diabetes, hypertension, high cholesterol, and coronary artery disease. All of these features can be improved or prevented with weight loss, exercise, and medical management. Other less commonly affected organs may include the liver and the eyes.
How is psoriasis treated?
There are now many different ways of treating psoriasis. When I first started treating psoriasis, we only had steroid creams, coal tar, and ultraviolet light called phototherapy. We actually admitted the more severe cases to hospital for 2-4 weeks and treated daily with these modalities.
They cleared up and stayed clear for about 3 months. Then it all gradually came back, and we started over again. We still use outpatient phototherapy without the tar for psoriasis and continue maintenance to prevent flare ups.
Please tell me about some of the newer internal treatments for psoriasis.
For the last 15 years there has been an explosion of new drugs for psoriasis that have been developed to block some specific chemicals that are increased in patients and which cause inflammation in the skin and joints. The inflammation then promotes the rapid overgrowth of skin cells and damages the joints.
Most of these drugs are synthesized in the laboratory. They are injectable proteins called Biologics that block tumor necrosis factor and various interleukins. Most of these can be injected by the patient at home or at the office by us if you prefer. Some familiar names are Enbrel, Humira, Stelara, and Taltz. There are at least 8 others approved and more in development.
We use all of these drugs in the Psoriasis Treatment Center at Riverchase Dermatology.
Does psoriasis affect the nails?
Yes. As psoriasis affects the skin under the nail (nailbed) and the skin around the nail (nailfolds), it causes changes in the growth rate, color, attachment, and the surface such as ridges and pitting.
How is nail psoriasis treated?
Psoriasis of the nails is very difficult to treat. Ultraviolet or laser light helps the psoriasis around the nail but can’t penetrate into the nailbed. Topical creams and solutions also can improve the appearance of the nail. The treatments that work best for the nail are the Biologic injections discussed above or pills such as Otezla or Methotrexate which are taken internally.
I have some pain in my fingers. How do I know if I have Psoriatic Arthritis?
If your pain, swelling, and stiffness is mainly in the morning, and takes 15 minutes to an hour to loosen up, that may be a sign of psoriatic arthritis. If you have one finger that’s swollen like a sausage, that is called dactylitis which is also a strong sign. Psoriatic arthritis may also affect tendons. If you have swelling or tenderness of the Achilles tendon at the heel, that may be a sign. Nail pitting and psoriasis on the same finger with joint pain may also indicate psoriatic arthritis.
Psoriatic arthritis may be difficult to diagnose. If you have psoriasis, there is about a 1 in 3 chance that you would develop psoriatic arthritis during your lifetime, but it can be confused with or overlap with rheumatoid arthritis or osteoarthritis. For this reason, we may order blood tests, X-rays, of a consultation with a Rheumatologist.
How is Psoriatic Arthritis treated?
Some of the drugs mentioned earlier are FDA-approved, meaning safe and effective, for psoriatic arthritis. Thus, if you have both psoriasis and psoriatic arthritis, you may improve if treated with Enbrel, Humira, Cimzia, Stelara, Tremfya, Taltz, Cosentyx, or Otezla. Methotrexate is often used in combination with these medicines. Xeljanz is only approved for psoriatic arthritis.
I understand that Biologic drugs are immunosuppressive. Should I stop them during the Covid-19 pandemic?
The Biologics are targeted to specific components of the immune system that lead to inflammation of psoriasis skin and joints. Although necessary for normal immunity, these components are found in excess in psoriasis patients. They are not blocked completely by the drugs.
Therefore, the National Psoriasis Foundation has recommended continuing the Biologic that has been prescribed for you because of the risk of recurrence of the psoriasis and arthritis, while still following all of the well-known CDC recommendations for prevention of Covid-19 infection. Moreover, when a Biologic is stopped for a while, there is a possibility that some its effectiveness will be reduced.
What can I expect for the future?
Even though we have so many new drugs for psoriasis, there is still no cure. Treatments need to be continued long-term to maintain clearance of the skin and remission of the arthritis. There are many new drugs under development that work by novel mechanisms as biologic injections, pills, and creams. Be on the lookout for these in the next few years.
Charles Camisa, MD, FAAD
Director, Psoriasis Treatment Center and Phototherapy Department
Recommended Reading:
Handbook of Psoriasis, 2nd Edition, 2005, Blackwell Publishing, by C. Camisa
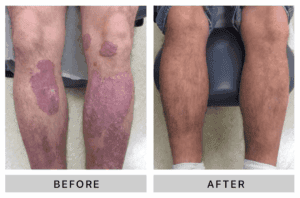
What is Phototherapy?
Phototherapy is the use of specific wavelengths of light that have been shown to be very effective in the treatment of psoriasis. This light occurs naturally as a component of sunlight and is called ultraviolet light.
What is UV Light?
Phototherapy, or ultraviolet light, is defined as either mid wave light energy (Ultraviolet-B light [UVB]) or long wave light (Ultraviolet-A [UVA]). UVB is available as narrowband or broadband. It has been known for many years that UVA, UVB, and narrowband UVB light – Ultraviolet phototherapy – slows abnormal growth of normal skin cells which is associated with psoriasis. Narrow band (NB) UVB and PUVA are often used to start the repigmenting process for vitiligo.
What is Narrow Band UVB Light?
Narrow band UVB is light energy which is emitted in a narrow band portion of the UVB light range, 311 nm to 313 nm. UVB-NB has been shown to be the optimal part of the UV light spectrum which slows growth of psoriasis lesions.
Is Phototherapy Safe?
As we all know, virtually every treatment for any type of illness carries with it some level of risk. We know that excessive exposure to UV light over a long period of time may increase the chances of skin cancer. However, unlike oral, IV or IM medications, the safety of UV light therapy (ultraviolet phototherapy) has been proven for over 100 years. Recent studies show that narrowband UVB lamps (UVB-NB) have virtually NO incidence of causing skin cancer.* Ultraviolet phototherapy in general, and particularly narrow band phototherapy light has been proven for long-term use and for treatment of children with minimal side effects.* Ultraviolet phototherapy has been shown to be an extremely effective treatment for controlling psoriasis and vitiligo.
With guidance from your physician, you will find that using UV light will keep you in almost complete remission with minimum side effects. However, to further reduce the risk, National Biological requires a physician’s prescription (U.S. only) to be certain that you have discussed the use of ultraviolet phototherapy at home. Plus, our ultraviolet phototherapy units, most available with narrowband UVB lamps, help to ensure this with numerous safety features including a controlled prescription timer, child-proof key lock switch and more.
Which Form Of Ultraviolet Phototherapy Is Best – UVA, UVB, or UVB-NB?
All of these light treatments are quite effective, and the form of ultraviolet phototherapy you need will be prescribed by your doctor. However, UVA light must always be used with an oral or tropical drug named Methoxsalen. Consequently, treatment with UVA light requires very active participation by your physician who must supervise your treatment closely. In most cases, it is preferable to use narrow band UVB (UVB-NB) light, since there is no need for systemic drugs like Methoxsalen and treatment times are short. Recent studies show that the use of UVB narrow band light (UVB-NB) results in faster responses and longer remissions than with UVB broadband. Using narrowband UVB, results are similar to a PUVA treatment without the adverse effects of the drug. Also, it is relatively easy for both you and your physician to monitor and control treatment. Narrowband UVB is often replacing conventional UVB because in many cases, it is safe and effective while taking less time. UVB-NB is generally considered to be safe for children and lactating mothers. Many practitioners have noted a significant reduction in psoriasis scaling after the first 3 to 6 treatments and improvement may be noted after 6 to 9 treatments. Repigmenting vitiligo is a longer process. We also offer blue (visible) lights to treat acne.
How Does Phototherapy Compare With Other Forms Of Psoriasis Treatment?
Other forms of treatment require the use of very strong steroids, immunosuppressive drugs, other systemic drugs or over the counter topical medications. These alternatives, while heavily promoted by drug companies, are costly, not effective for long term use, and have the potential for serious side effects. Ultraviolet phototherapy has been recognized as safe, effective, and economical and has stood the test of time.
How Often are Treatments Taken and How long Are Treatment Times?
This depends on your condition. For psoriasis, treatments are taken 3 to 5 times per week, with ultraviolet phototherapy treatment times beginning at a few seconds and increasing to several minutes over time. Once clearing is achieved, your doctor will determine whether your maintenance needs require regular phototherapy or whether your remission needs only periodic checkups.
At What Point Is Home Therapy A Viable Option?
Obviously, consult your physician, but if your involvement is 10% or more of your body, ultraviolet phototherapy is the fastest, most effective treatment possible. There is minimal risk involved. You can treat yourself in the privacy of your own home with your physician’s guidance. Together, you will determine an effective schedule of home treatment. All orders for our home therapy devices require a physician’s prescription.
Will I Still Need To See My Physician Once I Begin Treatment?
Yes. You and your physician will determine an effective schedule of home treatment, and he or she will monitor your progress. Only through the correct use of ultraviolet phototherapy and your physician’s guidance can you expect to keep your skin clear and reduce the potential for side effects. This is why all orders for home phototherapy devices require a physician’s prescription and supervision.
Is Home Phototherapy Expensive?
In most cases, no. Today many insurance carriers have recognized the value of a home phototherapy regimen under the guidance of a physician for the treatment of severe psoriasis. As a result, many insurance companies cover 80% or more of the cost of a home treatment device. National Biological accepts most major credit cards, and offers various payment options including extended terms. Plus, we offer FREE insurance claim assistance.
What are the Electrical Requirements?
All home phototherapy units from National Biological plug into standard household grounded electrical outlets. They require 110V and draw anywhere from 0.5 to 13 Amps.
How Long Do Lamps Last?
Under normal usage, the lamps have a useful life of three to five years. After that they will slowly lose power, so treatment times will increase two- or three-fold. Our lamps carry a 90 day warranty, and we always have replacements in stock.
What Maintenance Does A Home Phototherapy Machine Require?
Very little. You can keep lamps and reflector clean by periodically using a soft cloth with common glass cleaner. Timers also should be checked for accuracy.